From Wikipedia, the free encyclopedia
| Anthrax | |
|---|---|

Photomicrograph of a Gram stain of the bacterium Bacillus anthracis, the cause of the anthrax disease
|
|
| Classification and external resources | |
| ICD-10 | A22 |
| ICD-9 | 022 |
| DiseasesDB | 1203 |
| MedlinePlus | 001325 |
| eMedicine | med/148 |
| Patient UK | Anthrax |
| MeSH | D000881 |
Like many other members of the genus Bacillus, B. anthracis can form dormant endospores (often referred to as "spores" for short, but not to be confused with fungal spores) that are able to survive in harsh conditions for decades or even centuries.[1] Such spores can be found on all continents, even Antarctica.[2] When spores are inhaled, ingested, or come into contact with a skin lesion on a host, they may become reactivated and multiply rapidly.
Anthrax commonly infects wild and domesticated herbivorous mammals that ingest or inhale the spores while grazing. Ingestion is thought to be the most common route by which herbivores contract anthrax. Carnivores living in the same environment may become infected by consuming infected animals. Diseased animals can spread anthrax to humans, either by direct contact (e.g., inoculation of infected blood to broken skin) or by consumption of a diseased animal's flesh.
Anthrax does not spread directly from one infected animal or person to another; it is spread by spores. These spores can be transported by clothing or shoes. The body of an animal that had active anthrax at the time of death can also be a source of anthrax spores. Owing to the hardiness of anthrax spores, and their ease of production in vitro, they are extraordinarily well suited to use (in powdered and aerosol form) as biological weapons. Such weaponization has been accomplished in the past by at least five state bioweapons programs — those of the United Kingdom, Japan, the United States, Russia, and Iraq — and has been attempted by several others.[3]
Until the 20th century, anthrax infections killed hundreds of thousands of animals and people worldwide each year.[4] French scientist Louis Pasteur developed the first effective vaccine for anthrax in 1881.[5][6][7] As a result of over a century of animal vaccination programs, sterilization of raw animal waste materials, and anthrax eradication programs in United States, Canada, Russia, Eastern Europe, Oceania, and parts of Africa and Asia, anthrax infection is now relatively rare in domestic animals.[citation needed] Anthrax is especially rare in dogs and cats, as is evidenced by a single reported case in the United States in 2001.[8]
Anthrax outbreaks occur in some wild animal populations with some regularity.[9] The disease is more common in countries without widespread veterinary or human public health programs. In the 21st century, anthrax is still a problem in less developed countries. An outbreak of anthrax in humans who had eaten meat from a dead carabao was reported in Cagayan Province in the Philippines in early 2010, with over 400 cases of illness and at least two fatalities.[10]
B. anthracis bacterial spores are soil-borne. Because of their long lifespan, spores are present globally and remain at the burial sites of animals killed by anthrax for many decades. Disturbed grave sites of infected animals have caused reinfection over 70 years after the animal's interment.[11]
Signs and symptoms
Pulmonary
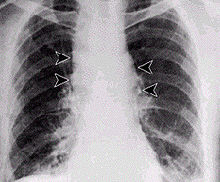
Respiratory infection on humans is relatively rare and initially presents with cold or flu-like symptoms for several days, followed by pneumonia and severe (and often fatal) respiratory collapse. Historical mortality rates were over 85%,[12] but, when treated early (seen in the 2001 anthrax attacks), observed case fatality rate dropped to 45%.[12][13] Distinguishing pulmonary anthrax from more common causes of respiratory illness is essential to avoiding delays in diagnosis and thereby improving outcomes. An algorithm for this purpose has been developed.[14]A lethal infection is reported to result from inhalation of about 10,000–20,000 spores, though this dose varies among host species.[15] As with all diseases, a wide variation in susceptibility is presumed, with evidence indicating some people may die from much lower exposures; little documented evidence is available to verify the exact or average number of spores needed for infection. Inhalational anthrax is also known as woolsorters' or ragpickers' disease. These professions were more susceptible to the disease due to their exposure to infected animal products. Other practices associated with exposure include the slicing up of animal horns for the manufacture of buttons, the handling of hair bristles used for the manufacturing of brushes, and the handling of animal skins. Whether these animal skins came from animals that died of the disease or from animals that had simply lain on ground with spores on it is unknown.
Gastrointestinal
Gastrointestinal (GI) infection in humans is most often caused by consuming anthrax-infected meat and is characterized by serious GI difficulty, vomiting of blood, severe diarrhea, acute inflammation of the intestinal tract, and loss of appetite.[16] Lesions have been found in the intestines and in the mouth and throat. After the bacterium invades the bowel system, it spreads through the bloodstream throughout the body, while also continuing to make toxins. GI infections can be treated, but usually result in fatality rates of 25% to 60%, depending upon how soon treatment commences. This form of anthrax is the rarest form. In the United States, only two official cases have occurred, the first reported in 1942 by the CDC and the second reported in 2010 that was treated at the Massachusetts General Hospital.[17][18][19] It is the only known case of survival from GI anthrax in the United States. An outbreak of anthrax among people who had eaten meat from a dead carabao was reported in Cagayan Province in the Philippines in early 2010, with over 400 cases of illness and at least two fatalities.[10]Cutaneous
Cutaneous anthrax, also known as Hide porter's disease, is the cutaneous (on the skin) manifestation of anthrax infection in humans. It presents as a boil-like skin lesion that eventually forms an ulcer with a black center (eschar). The black eschar often shows up as a large, painless necrotic ulcer (beginning as an irritating and itchy skin lesion or blister that is dark and usually concentrated as a black dot, somewhat resembling bread mold) at the site of infection. In general, cutaneous infections form within the site of spore penetration between two and five days after exposure. Unlike bruises or most other lesions, cutaneous anthrax infections normally do not cause pain.[20]
Cutaneous anthrax is typically caused when B. anthracis spores enter through cuts on the skin. This form is found most commonly when humans handle infected animals and/or animal products.
Cutaneous anthrax is rarely fatal if treated,[13] because the infection area is limited to the skin, preventing the lethal factor, edema factor, and protective antigen from entering and destroying a vital organ. Without treatment, about 20% of cutaneous skin infection cases progress to toxemia and death.
Cause
Bacteria

Color-enhanced scanning electron micrograph shows splenic tissue from a monkey with inhalational anthrax; featured are rod-shaped bacilli (yellow) and an erythrocyte (red).
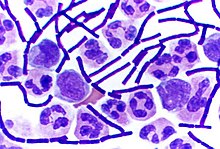
Gram-positive anthrax bacteria (purple rods) in cerebrospinal fluid sample: If present, a Gram-negative bacterial species would appear pink. (The other cells are white blood cells).
The production of two powerful exotoxins and lethal toxin by the bacteria causes death. Veterinarians can often tell a possible anthrax-induced death by its sudden occurrence, and by the dark, nonclotting blood that oozes from the body orifices. Most anthrax bacteria inside the body after death are outcompeted and destroyed by anaerobic bacteria within minutes to hours post mortem. However, anthrax vegetative bacteria that escape the body via oozing blood or through the opening of the carcass may form hardy spores. One spore forms per one vegetative bacterium. The triggers for spore formation are not yet known, though oxygen tension and lack of nutrients may play roles. Once formed, these spores are very hard to eradicate.
The infection of herbivores (and occasionally humans) by the inhalational route normally proceeds as follows: Once the spores are inhaled, they are transported through the air passages into the tiny air sacs (alveoli) in the lungs. The spores are then picked up by scavenger cells (macrophages) in the lungs and are transported through small vessels (lymphatics) to the lymph nodes in the central chest cavity (mediastinum). Damage caused by the anthrax spores and bacilli to the central chest cavity can cause chest pain and difficulty breathing. Once in the lymph nodes, the spores germinate into active bacilli that multiply and eventually burst the macrophages, releasing many more bacilli into the bloodstream to be transferred to the entire body. Once in the blood stream, these bacilli release three proteins named lethal factor, edema factor, and protective antigen. The three are not toxic by themselves, but the combination is incredibly lethal to humans.[22] Protective antigen combines with these other two factors to form lethal toxin and edema toxin, respectively. These toxins are the primary agents of tissue destruction, bleeding, and death of the host. If antibiotics are administered too late, even if the antibiotics eradicate the bacteria, some hosts will still die of toxemia because the toxins produced by the bacilli remain in their system at lethal dose levels.
The lethality of the anthrax disease is due to the bacterium's two principal virulence factors: the poly-D-glutamic acid capsule, which protects the bacterium from phagocytosis by host neutrophils, and the tripartite protein toxin, called anthrax toxin. Anthrax toxin is a mixture of three protein components: protective antigen (PA), edema factor (EF), and lethal factor (LF). PA plus LF produces lethal toxin, and PA plus EF produces edema toxin. These toxins cause death and tissue swelling (edema), respectively.
To enter the cells, the edema and lethal factors use another protein produced by B. anthracis called protective antigen, which binds to two surface receptors on the host cell. A cell protease then cleaves PA into two fragments: PA20 and PA63. PA20 dissociates into the extracellular medium, playing no further role in the toxic cycle. PA63 then oligomerizes with six other PA63 fragments forming a heptameric ring-shaped structure named a prepore. Once in this shape, the complex can competitively bind up to three EFs or LFs, forming a resistant complex.[22] Receptor-mediated endocytosis occurs next, providing the newly formed toxic complex access to the interior of the host cell. The acidified environment within the endosome triggers the heptamer to release the LF and/or EF into the cytosol.[23] It is unknown how exactly the complex results in the death of the cell.
Edema factor is a calmodulin-dependent adenylate cyclase. Adenylate cyclase catalyzes the conversion of ATP into cyclic AMP (cAMP) and pyrophosphate. The complexation of adenylate cyclase with calmodulin removes calmodulin from stimulating calcium-triggered signaling, thus inhibiting the immune response.[22] To be specific, LF inactivates neutrophils (a type of phagocytic cell) by the process just described so they cannot phagocytose bacteria. Throughout history, lethal factor was presumed to caused macrophages to make TNF-alpha and interleukin 1, beta (IL1B). TNF-alpha is a cytokine whose primary role is to regulate immune cells, as well as to induce inflammation and apoptosis or programmed cell death. Interleukin 1, beta is another cytokine that also regulates inflammation and apoptosis. The overproduction of TNF-alpha and IL1B ultimately leads to septic shock and death. However, recent evidence indicates anthrax also targets endothelial cells that line serous cavities such as the pericardial cavity, pleural cavity, and the peritoneal cavity, lymph vessels, and blood vessels, causing vascular leakage of fluid and cells, and ultimately hypovolemic shock and septic shock.
Exposure
Occupational exposure to infected animals or their products (such as skin, wool, and meat) is the usual pathway of exposure for humans. Workers who are exposed to dead animals and animal products are at the highest risk, especially in countries where anthrax is more common. Anthrax in livestock grazing on open range where they mix with wild animals still occasionally occurs in the United States and elsewhere. Many workers who deal with wool and animal hides are routinely exposed to low levels of anthrax spores, but most exposure levels are not sufficient to develop anthrax infections. The body's natural defenses presumably can destroy low levels of exposure. These people usually contract cutaneous anthrax if they catch anything. Throughout history, the most dangerous form of inhalational anthrax was called woolsorters' disease because it was an occupational hazard for people who sorted wool. Today, this form of infection is extremely rare, as almost no infected animals remain. The last fatal case of natural inhalational anthrax in the United States occurred in California in 1976, when a home weaver died after working with infected wool imported from Pakistan. To minimize the chance of spreading the disease, the deceased was transported to UCLA in a sealed plastic body bag within a sealed metal container for autopsy.[24]In November 2008, a drum maker in the United Kingdom who worked with untreated animal skins died from anthrax.[25] Gastrointestinal anthrax is exceedingly rare in the United States, with only one case on record, reported in 1942, according to the Centers for Disease Control and Prevention.[17] In December 2009, an outbreak of anthrax occurred amongst heroin addicts in Glasgow, Scotland, resulting in 14 deaths.[26] The source of the anthrax is believed to be dilution of the heroin with bone meal in Afghanistan.[27]
Also during December 2009, the New Hampshire Department of Health and Human Services confirmed a case of gastrointestinal anthrax in an adult female. The CDC investigated the source and the possibility that it was contracted from an African drum recently used by the woman taking part in a drumming circle.[28] The woman apparently inhaled anthrax [in spore form] from the hide of the drum. She became critically ill, but with gastrointestinal anthrax rather than inhaled anthrax, which made her unique in American medical history. The building where the infection took place was cleaned and reopened to the public and the woman recovered. Jodie Dionne-Odom, New Hampshire state epidemiologist, stated, "It is a mystery. We really don't know why it happened."[29]
Mode of infection
Anthrax can enter the human body through the intestines (ingestion), lungs (inhalation), or skin (cutaneous) and causes distinct clinical symptoms based on its site of entry. In general, an infected human will be quarantined. However, anthrax does not usually spread from an infected human to a noninfected human. But, if the disease is fatal to the person's body, its mass of anthrax bacilli becomes a potential source of infection to others and special precautions should be used to prevent further contamination. Inhalational anthrax, if left untreated until obvious symptoms occur, may be fatal.
Anthrax can be contracted in laboratory accidents or by handling infected animals or their wool or hides. It has also been used in biological warfare agents and by terrorists to intentionally infect as exemplified by the 2001 anthrax attacks.
Diagnosis
Various techniques are used for the direct identification of B. anthracis in clinical material. Firstly, specimens may be Gram stained. Bacillus spp. are quite large in size (3 to 4 μm long), they grow in long chains, and they stain Gram-positive. To confirm the organism is B. anthracis, rapid diagnostic techniques such as polymerase chain reaction-based assays and immunofluorescence microscopy may be used.[30]All Bacillus species grow well on 5% sheep blood agar and other routine culture media. Polymyxin-lysozyme-EDTA-thallous acetate can be used to isolate B. anthracis from contaminated specimens, and bicarbonate agar is used as an identification method to induce capsule formation. Bacillus spp. usually grow within 24 hours of incubation at 35 °C, in ambient air (room temperature) or in 5% CO2. If bicarbonate agar is used for identification, then the medium must be incubated in 5% CO2. B. anthracis colonies are medium-large, gray, flat, and irregular with swirling projections, often referred to as having a "medusa head" appearance, and are not hemolytic on 5% sheep blood agar. The bacteria are not motile, susceptible to penicillin, and produce a wide zone of lecithinase on egg yolk agar. Confirmatory testing to identify B. anthracis includes gamma bacteriophage testing, indirect hemagglutination, and enzyme linked immunosorbent assay to detect antibodies.[31] The best confirmatory precipitation test for anthrax is the Ascoli test.
Prevention
Vaccines
Vaccines against anthrax for use in livestock and humans have had a prominent place in the history of medicine, from Pasteur's pioneering 19th-century work with cattle (the second effective vaccine ever) to the controversial 20th century use of a modern product (BioThrax) to protect American troops against the use of anthrax in biological warfare. Human anthrax vaccines were developed by the Soviet Union in the late 1930s and in the US and UK in the 1950s. The current FDA-approved US vaccine was formulated in the 1960s.Currently administered human anthrax vaccines include acellular (United States) and live spore (Russia) varieties. All currently used anthrax vaccines show considerable local and general reactogenicity (erythema, induration, soreness, fever) and serious adverse reactions occur in about 1% of recipients.[32] The American product, BioThrax, is licensed by the FDA and was formerly administered in a six-dose primary series at 0, 2, 4 weeks and 6, 12, 18 months, with annual boosters to maintain immunity. In 2008, the FDA approved omitting the week-2 dose, resulting in the currently recommended five-dose series.[33] New second-generation vaccines currently being researched include recombinant live vaccines and recombinant subunit vaccines.
Prophylaxis
If a person is suspected as having died from anthrax, every precaution should be taken to avoid skin contact with the potentially contaminated body and fluids exuded through natural body openings. The body should be put in strict quarantine. A blood sample should then be collected and sealed in a container and analyzed in an approved laboratory to ascertain if anthrax is the cause of death. Then, the body should be incinerated. Microscopic visualization of the encapsulated bacilli, usually in very large numbers, in a blood smear stained with polychrome methylene blue (McFadyean stain) is fully diagnostic, though culture of the organism is still the gold standard for diagnosis. Full isolation of the body is important to prevent possible contamination of others. Protective, impermeable clothing and equipment such as rubber gloves, rubber apron, and rubber boots with no perforations should be used when handling the body. No skin, especially if it has any wounds or scratches, should be exposed.Disposable personal protective equipment is preferable, but if not available, decontamination can be achieved by autoclaving. Disposable personal protective equipment and filters should be autoclaved, and/or burned and buried. B. anthracis bacillii range from 0.5–5.0 μm in size. Anyone working with anthrax in a suspected or confirmed victim should wear respiratory equipment capable of filtering this size of particle or smaller. The US National Institute for Occupational Safety and Health – and Mine Safety and Health Administration-approved high-efficiency respirator, such as a half-face disposable respirator with a high-efficiency particulate air filter, is recommended.[34] All possibly contaminated bedding or clothing should be isolated in double plastic bags and treated as possible biohazard waste. The victim should be sealed in an airtight body bag. Dead victims who are opened and not burned provide an ideal source of anthrax spores. Cremating victims is the preferred way of handling body disposal. No embalming or autopsy should be attempted without a fully equipped biohazard laboratory and trained, knowledgeable personnel.
Delays of only a few days may make the disease untreatable, so treatment should be started even without symptoms if possible contamination or exposure is suspected. Animals with anthrax often just die without any apparent symptoms. Initial symptoms may resemble a common cold—sore throat, mild fever, muscle aches, and malaise. After a few days, the symptoms may progress to severe breathing problems and shock, and ultimately death. Death can occur from about two days to a month after exposure, with deaths apparently peaking at about eight days after exposure.[35] Antibiotic-resistant strains of anthrax are known.
Early detection of sources of anthrax infection can allow preventive measures to be taken. In response to the anthrax attacks of October 2001, the United States Postal Service (USPS) installed biodetection systems (BDSs) in their large-scale mail cancellation facilities. BDS response plans were formulated by the USPS in conjunction with local responders including fire, police, hospitals and public health. Employees of these facilities have been educated about anthrax, response actions, and prophylactic medication. Because of the time delay inherent in getting final verification that anthrax has been used, prophylactic antibiotic treatment of possibly exposed personnel must be started as soon as possible.
Treatment
Anthrax cannot be spread directly from person to person, but a person's clothing and body may be contaminated with anthrax spores. Effective decontamination of people can be accomplished by a thorough wash-down with antimicrobial soap and water. Waste water should be treated with bleach or other antimicrobial agent. Effective decontamination of articles can be accomplished by boiling them in water for 30 minutes or longer. Chlorine bleach is ineffective in destroying spores and vegetative cells on surfaces, though formaldehyde is effective. Burning clothing is very effective in destroying spores. After decontamination, there is no need to immunize, treat, or isolate contacts of persons ill with anthrax unless they were also exposed to the same source of infection.Antibiotics
Early antibiotic treatment of anthrax is essential; delay significantly lessens chances for survival.Treatment for anthrax infection and other bacterial infections includes large doses of intravenous and oral antibiotics, such as fluoroquinolones (ciprofloxacin), doxycycline, erythromycin, vancomycin, or penicillin. FDA-approved agents include ciprofloxacin, doxycycline, and penicillin.[36]
In possible cases of pulmonary anthrax, early antibiotic prophylaxis treatment is crucial to prevent possible death.
In May 2009, Human Genome Sciences submitted a Biologic License Application (BLA, permission to market) for its new drug, raxibacumab (brand name ABthrax) intended for emergency treatment of inhaled anthrax.[37] If death occurs from anthrax, the body should be isolated to prevent possible spread of anthrax germs. Burial does not kill anthrax spores.
In recent years, many attempts have been made to develop new drugs against anthrax, but existing drugs are effective if treatment is started soon enough.
Monoclonal antibodies
On 14 December 2012, the US Food and Drug Administration approved raxibacumab injection to treat inhalational anthrax. Raxibacumab is a monoclonal antibody that neutralizes toxins produced by B. anthracis that can cause massive and irreversible tissue injury and death. A monoclonal antibody is a protein that closely resembles a human antibody, and identifies and neutralizes foreign material such as bacteria and viruses.[38]History
Etymology
The name comes from anthrax [άνθραξ], the Greek word for coal, because of the black skin lesions developed by victims with a cutaneous anthrax infection. It was discovered and analyzed by Robert Koch (1876).Alternative names include Siberian plague, charbon, splenic fever, malignant edema, and woolsorter's disease.
Discovery
Robert Koch, a German physician and scientist, first identified the bacterium that caused the anthrax disease in 1875 in Wolsztyn.[21][39] His pioneering work in the late 19th century was one of the first demonstrations that diseases could be caused by microbes. In a groundbreaking series of experiments, he uncovered the lifecycle and means of transmission of anthrax. His experiments not only helped create an understanding of anthrax, but also helped elucidate the role of microbes in causing illness at a time when debates still took place over spontaneous generation versus cell theory. Koch went on to study the mechanisms of other diseases and won the 1905 Nobel Prize in Physiology or Medicine for his discovery of the bacterium causing tuberculosis.First vaccination

In May 1881, Louis Pasteur performed a public experiment to demonstrate his concept of vaccination. He prepared two groups of 25 sheep, one goat, and several cows. The animals of one group were injected with an anthrax vaccine prepared by Pasteur twice, at an interval of 15 days; the control group was left unvaccinated. Thirty days after the first injection, both groups were injected with a culture of live anthrax bacteria. All the animals in the unvaccinated group died, while all of the animals in the vaccinated group survived.[40]
The human vaccine for anthrax became available in 1954. This was a cell-free vaccine instead of the live-cell Pasteur-style vaccine used for veterinary purposes. An improved cell-free vaccine became available in 1970.[41]
Society and culture
The virulent Ames strain, which was used in the 2001 anthrax attacks in the United States, has received the most news coverage of any anthrax outbreak. The Ames strain contains two virulence plasmids, which separately encode for a three-protein toxin, called anthrax toxin, and a polyglutamic acid capsule. Nonetheless, the Vollum strain, developed but never used as a biological weapon during the Second World War, is much more dangerous. The Vollum (also incorrectly referred to as Vellum) strain was isolated in 1935 from a cow in Oxfordshire. This same strain was used during the Gruinard bioweapons trials. A variation of Vollum known as "Vollum 1B" was used during the 1960s in the US and UK bioweapon programs. Vollum 1B is widely believed[42] to have been isolated from William A. Boyles, a 46-year-old scientist at the U.S. Army Biological Warfare Laboratories at Camp (later Fort) Detrick, Maryland, (precursor to USAMRIID), who died in 1951 after being accidentally infected with the Vollum strain. The Sterne strain, named after the Trieste-born immunologist Max Sterne, is an attenuated strain used as a vaccine, which contains only the anthrax toxin virulence plasmid and not the polyglutamic acid capsule expressing plasmid.Site cleanup and decontamination
Anthrax spores can survive for very long periods of time in the environment after release. Chemical methods for cleaning anthrax-contaminated sites or materials may use oxidizing agents such as peroxides, ethylene oxide, Sandia Foam,[43] chlorine dioxide (used in the Hart Senate Office Building), peracetic acid, ozone gas, hypochlorous acid, sodium persulfate, and liquid bleach products containing sodium hypochlorite. Nonoxidizing agents shown to be effective for anthrax decontamination include methyl bromide, formaldehyde, and metam sodium. These agents destroy bacterial spores. All of the aforementioned anthrax decontamination technologies have been demonstrated to be effective in laboratory tests conducted by the US EPA or others.[44] A bleach solution for treating hard surfaces has been approved by the EPA.[45]Chlorine dioxide has emerged as the preferred biocide against anthrax-contaminated sites, having been employed in the treatment of numerous government buildings over the past decade. Its chief drawback is the need for in situ processes to have the reactant on demand.
To speed the process, trace amounts of a nontoxic catalyst composed of iron and tetroamido macrocyclic ligands are combined with sodium carbonate and bicarbonate and converted into a spray. The spray formula is applied to an infested area and is followed by another spray containing tert-butyl hydroperoxide.[46]
Using the catalyst method, a complete destruction of all anthrax spores can be achieved in under 30 minutes.[46] A standard catalyst-free spray destroys fewer than half the spores in the same amount of time. They can be heated and exposed to the harshest chemicals, but they do not easily die.[vague]
Cleanups at a Senate office building, several contaminated postal facilities, and other US government and private office buildings showed decontamination to be possible, but it is time-consuming and costly. Clearing the Senate office building of anthrax spores cost $27 million, according to the Government Accountability Office. Cleaning the Brentwood postal facility outside Washington cost $130 million and took 26 months. Since then, newer and less costly methods have been developed.[47]
Cleanup of anthrax-contaminated areas on ranches and in the wild is much more problematic. Carcasses may be burned, though it often takes up to three days to burn a large carcass and this is not feasible in areas with little wood. Carcasses may also be buried, though the burying of large animals deeply enough to prevent resurfacing of spores requires much manpower and expensive tools. Carcasses have been soaked in formaldehyde to kill spores, though this has environmental contamination issues. Block burning of vegetation in large areas enclosing an anthrax outbreak has been tried; this, while environmentally destructive, causes healthy animals to move away from an area with carcasses in search of fresh grass. Some wildlife workers have experimented with covering fresh anthrax carcasses with shadecloth and heavy objects. This prevents some scavengers from opening the carcasses, thus allowing the putrefactive bacteria within the carcass to kill the vegetative B. anthracis cells and preventing sporulation. This method also has drawbacks, as scavengers such as hyenas are capable of infiltrating almost any exclosure.
The experimental site at Gruinard Island is said to have been decontaminated with a mixture of formaldehyde and seawater by the Ministry of Defence. It is not clear whether similar treatments had been applied to US test sites.
Biological warfare
Anthrax spores can and have been used as a biological warfare weapon. Its first modern incidence occurred when Scandinavian rebels, supplied by the German General Staff, used anthrax with unknown results against the Imperial Russian Army in Finland in 1916.[48] Anthrax was first tested as a biological warfare agent by Unit 731 of the Japanese Kwantung Army in Manchuria during the 1930s; some of this testing involved intentional infection of prisoners of war, thousands of whom died. Anthrax, designated at the time as Agent N, was also investigated by the Allies in the 1940s.
A long history of practical bioweapons research exists in this area. For example, in 1942, British bioweapons trials[49] severely contaminated Gruinard Island in Scotland with anthrax spores of the Vollum-14578 strain, making it a no-go area until it was decontaminated in 1990.[50][51] The Gruinard trials involved testing the effectiveness of a submunition of an "N-bomb" — a biological weapon containing dried anthrax spores. Additionally, five million "cattle cakes" (animal feed pellets impregnated with anthrax spores) were prepared and stored at Porton Down for "Operation Vegetarian" — antilivestock attacks against Germany to be made by the Royal Air Force.[52] The plan was for anthrax-based biological weapons to be dropped on Germany in 1944. However, the edible cattle cakes and the bomb were not used; the cattle cakes were incinerated in late 1945.
Weaponized anthrax was part of the US stockpile prior to 1972, when the United States signed the Biological Weapons Convention.[53] President Nixon ordered the dismantling of US biowarfare programs in 1969 and the destruction of all existing stockpiles of bioweapons. In 1978–1979, the Rhodesian government used anthrax against cattle and humans during its campaign against black rebels.[54] The Soviet Union created and stored 100 to 200 tons of anthrax spores at Kantubek on Vozrozhdeniya Island. They were abandoned in 1992 and destroyed in 2002.
American military and British Army personnel are routinely vaccinated against anthrax prior to active service in places where biological attacks are considered a threat.
- Sverdlovsk incident (2 April 1979)
Nearly all of the night-shift workers of a ceramics plant directly across the street from the biological facility (compound 19) became infected, and most died. Since most were men, some NATO governments suspected the Soviet Union had developed a sex-specific weapon.[58] The government blamed the outbreak on the consumption of anthrax-tainted meat, and ordered the confiscation of all uninspected meat that entered the city. They also ordered all stray dogs to be shot and people not have contact with sick animals. Also, a voluntary evacuation and anthrax vaccination program was established for people from 18–55.[59]
To support the cover-up story, Soviet medical and legal journals published articles about an outbreak in livestock that caused GI anthrax in people having consumed infected meat, and cutaneous anthrax in people having come into contact with the animals. All medical and public health records were confiscated by the KGB.[59] In addition to the medical problems the outbreak caused, it also prompted Western countries to be more suspicious of a covert Soviet bioweapons program and to increase their surveillance of suspected sites. In 1986, the US government was allowed to investigate the incident, and concluded the exposure was from aerosol anthrax from a military weapons facility.[60] In 1992, President Yeltsin admitted he was "absolutely certain" that "rumors" about the Soviet Union violating the 1972 Bioweapons Treaty were true. The Soviet Union, like the US and UK, had agreed to submit information to the UN about their bioweapons programs, but omitted known facilities and never acknowledged their weapons program.[58]
- Anthrax bioterrorism
Concentrated anthrax spores were used for bioterrorism in the 2001 Anthrax Attacks in the United States, delivered by mailing postal letters containing the spores.[62] The letters were sent to several news media offices and two Democratic senators: Tom Daschle of South Dakota and Patrick Leahy of Vermont. As a result, 22 were infected and five died.[22] Only a few grams of material were used in these attacks and in August 2008, the US Department of Justice announced they believed that Dr. Bruce Ivins, a senior biodefense researcher employed by the United States government, was responsible.[63] These events also spawned many anthrax hoaxes.
Due to these events, the U.S. Postal Service installed biohazard detection systems at its major distribution centers to actively scan for anthrax being transported through the mail.[64]
- Decontaminating mail
A scientific experiment performed by a high school student, later published in The Journal of Medical Toxicology, suggested a domestic electric iron at its hottest setting (at least 400 °F) used for at least 5 minutes should destroy all anthrax spores in a common postal envelope.[66]