The biopsychological theory of personality
is a model of the general biological processes relevant for human
psychology, behavior, and personality. The model, proposed by research
psychologist Jeffrey Alan Gray in 1970, is well-supported by subsequent research and has general acceptance among professionals.
Gray hypothesized the existence of two brain-based systems for controlling a person's interactions with their environment: the behavioural inhibition system (BIS) and the behavioural activation system (BAS). BIS is related to sensitivity to punishment and avoidance motivation. BAS is associated with sensitivity to reward and approach motivation. Psychological scales have been designed to measure these hypothesized systems and study individual differences in personality. Neuroticism, a widely studied personality dimension related to emotional functioning, is positively correlated with BIS scales and negatively correlated with BAS scales.
Gray hypothesized the existence of two brain-based systems for controlling a person's interactions with their environment: the behavioural inhibition system (BIS) and the behavioural activation system (BAS). BIS is related to sensitivity to punishment and avoidance motivation. BAS is associated with sensitivity to reward and approach motivation. Psychological scales have been designed to measure these hypothesized systems and study individual differences in personality. Neuroticism, a widely studied personality dimension related to emotional functioning, is positively correlated with BIS scales and negatively correlated with BAS scales.
History
The biopsychological theory of personality is similar to another one of Gray's theories, reinforcement sensitivity theory. The Biopsychological Theory of Personality was created after Gray disagreed with Hans Eysenck's arousal theory that dealt with biological personality traits. Eysenck looked at the ascending reticular activating system
(ARAS) for answering questions about personality. The ARAS is part of
the brain structure and has been proposed to deal with cortical arousal,
hence the term arousal theory. Eysenck compared levels of arousal to a
scale of introversion versus extraversion. The comparison of these two
scales was then used to describe individual personalities and their
corresponding behavioral patterns.
Gray disagreed with Eysenck's theory because Gray believed that things
such as personality traits could not be explained by just classical
conditioning. Instead, Gray developed his theory which is based more heavily on physiological responses than Eysenck's theory.
Gray had a lot of support for his theories and experimented with animals to test his hypotheses.
Using animal subjects allows researchers to test whether different
areas of the brain are responsible for different learning mechanisms.
Specifically, Gray's theory concentrated on understanding how reward or
punishment related to anxiety
and impulsivity measures. His research and further studies have found
that reward and punishment are under the control of separate systems and
as a result people can have different sensitivities to such rewarding
or punishing stimuli.
Behavioral inhibition system
The behavioral inhibition system (BIS), as proposed by Gray, is a neuropsychological
system that predicts an individual's response to anxiety-relevant cues
in a given environment. This system is activated in times of punishment,
boring things, or negative events.
By responding to cues such as negative stimuli or events that involve
punishment or frustration, this system ultimately results in avoidance
of such negative and unpleasant events. According to Gray's Theory, the BIS is related to sensitivity to punishment as well as avoidance motivation. It has also been proposed that the BIS is the causal basis of anxiety.
High activity of the BIS means a heightened sensitivity to nonreward,
punishment, and novel experience. This higher level of sensitivity to
these cues results in a natural avoidance of such environments in order
to prevent negative experiences such as fear, anxiety, frustration, and
sadness. People who are highly sensitive to punishment perceive
punishments as more aversive and are more likely to be distracted by
punishments.
The physiological mechanism behind the BIS is believed to be the septohippocampal system and its monoaminergic afferents from the brainstem.
Using a voxel-based morphometry analysis, the volume of the regions
mentioned was assessed to view individual differences. Findings may
suggest a correlation between the volume and anxiety-related personality
traits. Results were found in the orbitofrontal cortex, the precuneus,
the amygdala, and the prefrontal cortex.
Behavioral activation system
The
behavioral activation system (BAS), in contrast to the BIS, is based on
a model of appetitive motivation - in this case, an individual's
disposition to pursue and achieve goals. The BAS is aroused when it
receives cues corresponding to rewards and controls actions that are not
related to punishment, rather actions regulating approachment type
behaviors. This system has an association with hope. According to Gray's theory, the BAS is sensitive to conditioned appealing stimuli, and is associated with impulsivity. It is also thought to be related to sensitivity to reward
as well as approach motivation. The BAS is sensitive to nonpunishment
and reward. Individuals with a highly active BAS show higher levels of
positive emotions such as elation, happiness, and hope in response to
environmental cues consistent with nonpunishment and reward, along with
goal-achievement. In terms of personality, these individuals are also
more likely to engage in goal-directed efforts and experience these
positive emotions when exposed to impending reward. The physiological
mechanism for BAS is not known as well as BIS, but is believed to be
related to catecholaminergic and dopaminergic pathways in the brain. Dopamine is a neurotransmitter
commonly linked with positive emotions, which could explain the
susceptibility to elation and happiness upon achieving goals which has
been observed. People with a highly active BAS have been shown to learn
better by reward than by punishment, inverse to BIS as mentioned above.
BAS is considered to include trait impulsivity that is also related to
psychopathological disorders such as ADHD, drug abuse, and alcohol
abuse.
The higher the BAS score, or the higher the impulsive, the more it is
likely to be related to psycho-pathological or dis-inhibitory disorders.
Certain aspects of the dopaminergic reward system activate when reward
cues and reinforcers are presented, including biological rewards such as
food and sex. These brain areas, which were highlighted during multiple fMRI studies, are the same areas associated with BAS.
Compare and contrast
Together,
the two systems work in an inverse relationship. In other words, when a
specific situation occurs, an organism can approach the situation with
one of the two systems. The systems will not be stimulated at the same
time and which system is dominant depends on the situation in terms of
punishment versus reward.
This phenomenon of the differentiation between the two systems is
thought to occur because of the distinct areas in the brain that becomes
activated in response to different stimuli. This difference was noted
years ago through electrical stimulation of the brain.
The behavioral activation system and behavioral inhibition system
differ in their physiological pathways in the brain. The inhibition
system has been shown to be linked to the septo-hippocampal system which
appears to have a close correlation to a serotonergic pathway, with
similarities in their innervations and stress responses. On the other
hand, the activation, or reward system, is thought to be associated more
with a mesolimbic dopaminergic system as opposed to the serotonergic
system.
The two systems proposed by Gray differ in their motivations and
physiological responses. Gray also proposed that individuals can vary
widely in their responsiveness of the behavioral inhibition system and
the behavioral activation system. It has been found that someone who is
sensitive to their BIS will be more receptive to the negative cues as
compared to someone who is sensitive to their BAS and therefore responds
more to cues in the environment that relate to that system,
specifically positive or rewarding cues. Researchers besides Gray have
shown interest in this theory and have created questionnaires that
measure BIS and BAS sensitivity. Carver and White have been the primary
researchers responsible for the questionnaire. Carver and White created a
scale that has been shown to validly measure levels of individual
scores of BIS and BAS. This measure focuses on the differences in
incentive motivations and aversive motivations. As previously mentioned
these motivations correlate to impulsivity and anxiety respectively.
Applications
Since
the development of the BAS and BIS, tests have been created to see how
individuals rate in each area. The questionnaire is called the
Behavioral Inhibition System and Behavioral Activation System
Questionnaire.
People can be tested based on their activation of either systems by using an EEG. These tests will conclude whether a person has a more active BIS or BAS. The two systems are independent of each other.
These tests can determine different things about a person's
personality. They can determine if a person has more positive or
negative moods. Using psychological test scales designed to correlate with the attributes of these hypothesized systems, neuroticism has been found to be positively correlated with the BIS scale, and negatively correlated with the BAS scale.
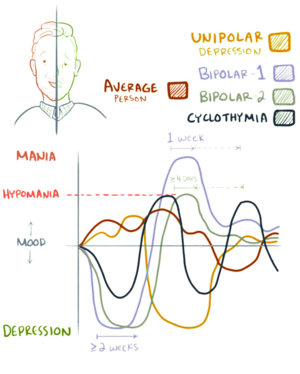
According to Richard Depue's BAS dysregulation theory of bipolar disorders,
now doctors and other professionals can determine if a person with
bipolar disorder is on the brink of a manic or depressive episode based
on how they rate on a scale of BAS and BIS sensitivity. Essentially,
this dysregulation theory proposes that people with BAS dysregulation
have an extraordinarily sensitive behavioral activation system and their
BAS is hyper-responsive to behavioral approach system cues.
If a person with bipolar disorder self-reports high sensitivity to BAS,
it means that a manic episode could occur faster. Also, if a person
with bipolar disorder reports high sensitivity to BIS it could indicate a
depressive phase. A better understanding of BAS dysregulation theory can inform psychosocial intervention (e.g. cognitive behavioral therapy, psychoeducation, interpersonal and social rhythm therapy, etc.).
The BAS/BIS Questionnaire can also be used in the cases of criminal profiling.
Previous research as reported by researchers MacAndrew and Steele in
1991 compared two groups on opposite spectrum levels of fear and the
response of a variety of questions. The two groups in the study varied
on levels of BIS, either high or low, and were selected by the
researchers. One group was composed of women who had experienced anxiety attacks
and together made up the high BIS group. The low BIS group was composed
of convicted prostitutes who had been found to take part in illegal
behavior. Main findings showed that the responses to the questionnaires
were distinctly different between the high BIS group and the low BIS
group, with the convicted women scoring lower. Results from this study
demonstrate that questionnaires can be used as a valid measurement to
show differences in the behavioral inhibition systems of different types
of people.
Gray also introduced his SPSRQ questionnaire to measure sensitivity to
reward (SR) and sensitivity to punishment (SP) in anxiety (2012). It is a
specifically designed questionnaire linking to Gray's theory
referencing the SR to the BAS and the SP to the BIS.
Future research or implications
As
mentioned previously, psychological disorders have been analyzed in
terms of the behavioral inhibition and activation systems. Understanding
the differences between the systems may relate to an understanding of
different types of disorders that involve anxiety and impulsivity. To
date, there are many types of anxiety disorders that deal with avoidance
theories and future research could show that the behavioral activation
system plays a large role in such disorders and may have future
implications for treatment of patients.