From Wikipedia, the free encyclopedia
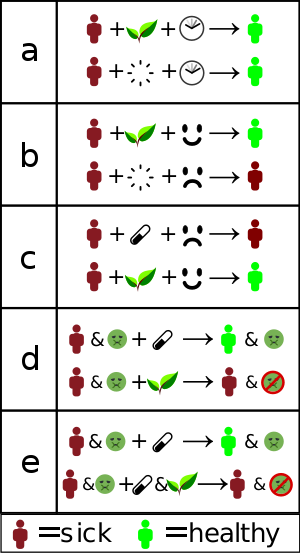
How alternative treatments "work":
a) Misinterpreted natural course – the individual gets better without treatment.
b) Placebo effect
or false treatment effect – an individual receives "alternative
therapy" and is convinced it will help. The conviction makes them more
likely to get better.
c) Nocebo
effect – an individual is convinced that standard treatment will not
work, and that alternative treatment will work. This decreases the
likelyhood standard treatment will work, while the placebo effect of the
"alternative" remains.
d) No adverse effects — Standard treatment is replaced with
"alternative" treatment, getting rid of adverse effects, but also of
improvement.
e) Interference — Standard treatment is "complemented" with something
that interferes with its effect. This can both cause worse effect, but
also decreased (or even increased) side effects, which may be
interpreted as "helping".
|
Alternative medicine,
fringe medicine,
pseudomedicine or simply
questionable medicine
is the use and promotion of practices which are unproven, disproven,
impossible to prove, or excessively harmful in relation to their effect —
in the attempt to achieve the
healing effects of
medicine. They differ from
experimental medicine in that the latter employs
responsible investigation, and accepts results that show it to be ineffective. The
scientific consensus is that alternative therapies either do not, or cannot, work. In some cases
laws of nature are violated by their basic claims; in some the treatment is so much worse that its use is
unethical. Alternative practices, products, and therapies range from only ineffective to having known harmful and
toxic effects.
Alternative therapies may be
credited for perceived improvement through
placebo effects, decreased use or effect of medical treatment (and therefore either decreased
side effects; or
nocebo effects towards standard treatment), or the
natural course of the condition or disease. Alternative treatment is not the same as
experimental treatment or
traditional medicine,
although both can be misused in ways that are alternative. Alternative
or complementary medicine is dangerous because it may discourage people
from getting the best possible treatment, and may lead to a false
understanding of the body and of
science.
Alternative medicine is used by a significant number of people,
though its popularity is often overstated. Large amounts of funding go
to testing alternative medicine, with more than US$2.5
billion spent by the United States government alone. Almost none show any effect beyond that of
false treatment,
and most studies showing any effect have been statistical flukes.
Alternative medicine is a highly profitable industry, with a strong
lobby. This fact is often overlooked by media or intentionally kept
hidden, with alternative practice being portrayed positively when
compared to
"big pharma".
The lobby has successfully pushed for alternative therapies to be
subject to far less regulation than conventional medicine. Alternative
therapies may even be allowed to promote use when there is demonstrably
no effect, only a tradition of use. Regulation and licensing of
alternative medicine and
health care providers
varies between and within countries. Despite laws making it illegal to
market or promote alternative therapies for use in cancer treatment,
many practitioners promote them. Alternative medicine is criticized for
taking advantage of the weakest members of society. For example, the
United States National Institutes of Health department studying alternative medicine, currently named
National Center for Complementary and Integrative Health, was established as the
Office of Alternative Medicine and was renamed the
National Center for Complementary and Alternative Medicine before obtaining its current name. Therapies are often
framed
as "natural" or "holistic", in apparent opposition to conventional
medicine which is "artificial" and "narrow in scope", statements which
are intentionally misleading. When used together with functional medical
treatment, alternative therapies do not "complement" (improve the
effect of, or mitigate the side effects of) treatment. Significant
drug interactions caused by alternative therapies may instead negatively impact functional treatment, making it less effective, notably in
cancer.
Alternative diagnoses and
treatments are not part of
medicine, or of science-based curricula in
medical schools, nor are they used in any practice based on scientific knowledge or experience. Alternative therapies are often based on
religious belief, tradition,
superstition, belief in
supernatural energies,
pseudoscience,
errors in reasoning, propaganda, fraud, or lies. Alternative medicine is based on misleading statements,
quackery,
pseudoscience,
antiscience,
fraud, and poor
scientific methodology. Promoting alternative medicine has been called dangerous and
unethical.
Testing alternative medicine that has no scientific basis has been
called a waste of scarce research resources. Critics state that "there
is really no such thing as alternative medicine, just medicine that
works and medicine that doesn't", that the very idea of "alternative"
treatments is
paradoxical, as any treatment proven to work is by definition "medicine".
Definitions and terminology
Alternative medicine
Alternative medicine
is defined loosely as a set of products, practices, and theories that
are believed or perceived by their users to have the healing effects of
medicine,
[n 1][n 2] but whose
effectiveness has not been clearly established using
scientific methods, or whose theory and practice is not part of
biomedicine or whose theories or practices are directly contradicted by
scientific evidence or
scientific principles used in biomedicine. "Biomedicine" or "medicine" is that part of
medical science that applies principles of
biology,
physiology,
molecular biology,
biophysics, and other
natural sciences to
clinical practice, using scientific methods to establish the effectiveness of that practice. Unlike medicine,
[n 4] an alternative product or practice does not originate from using scientific methods, but may instead be based on
hearsay,
religion, tradition,
superstition, belief in
supernatural energies,
pseudoscience,
errors in reasoning,
propaganda,
fraud, or other unscientific sources.
In
General Guidelines for Methodologies on Research and Evaluation of Traditional Medicine, published in 2000 by the
World Health Organization
(WHO), complementary and alternative medicine were defined as a broad
set of health care practices that are not part of that country's own
tradition and are not integrated into the dominant health care system.
[12]
The expression also refers to a diverse range of related and
unrelated products, practices, and theories ranging from biologically
plausible practices and products and practices with some evidence, to
practices and theories that are directly contradicted by basic science
or clear evidence, and products that have been conclusively proven to be
ineffective or even toxic and harmful.
The terms
alternative medicine,
complementary medicine,
integrative medicine, holistic medicine,
natural medicine,
unorthodox medicine,
fringe medicine,
unconventional medicine, and
new age medicine are used interchangeably as having the same meaning and are almost synonymous in some contexts,
[16][17][18][19] but may have different meanings in some rare cases.
Marcia Angell: "There cannot be two kinds of medicine – conventional and alternative".
The meaning of the term "alternative" in the expression "alternative medicine", is not that it is an effective alternative to
medical science, although some alternative medicine promoters may use the loose terminology to give the appearance of effectiveness.
[4][20]
Loose terminology may also be used to suggest meaning that a dichotomy
exists when it does not, e.g., the use of the expressions "western
medicine" and "eastern medicine" to suggest that the difference is a
cultural difference between the Asiatic east and the European west,
rather than that the difference is between
evidence-based medicine and treatments that don't work.
[4]
Complementary or integrative medicine
Complementary medicine (
CM) or
integrative medicine (
IM) is when alternative medicine is used together with functional medical treatment, in a
belief that it improves the effect of treatments. However, significant
drug interactions caused by alternative therapies may instead negatively influence treatment, making treatments less effective, notably
cancer therapy.
[25][26] Both terms refer to use of alternative medical treatments alongside conventional medicine,
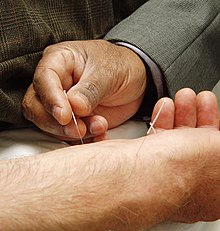
[27][28][29] an example of which is use of
acupuncture
(sticking needles in the body to influence the flow of a supernatural
energy), along with using science-based medicine, in the belief that the
acupuncture increases the effectiveness or "complements" the
science-based medicine.
[29]
Allopathic medicine
Allopathic medicine or
allopathy is an expression commonly used by
homeopaths and proponents of other forms of alternative medicine to refer to
mainstream medicine. It was used to describe the traditional European practice of
heroic medicine,
which was based on balance of the four "humours" (blood, phlegm, yellow
bile, and black bile) where disease was caused by an excess of one
humour, and would thus be treated with its opposite.
[30] This description continued to be used to describe anything that was not homeopathy.
[30] Apart from in
India, the term is not used outside alternative medicine and not accepted by the medical field.
Allopathy refers to the use of pharmacologically active
agents or
physical interventions to treat or suppress
symptoms or
pathophysiologic processes of diseases or conditions.
[31] The German version of the word,
allopathisch, was coined in 1810 by the creator of
homeopathy,
Samuel Hahnemann (1755–1843).
[32] The word was coined from
allo- (different) and
-pathic (relating to a disease or to a method of treatment).
[33]
In alternative medicine circles the expression "allopathic medicine" is
still used to refer to "the broad category of medical practice that is
sometimes called Western medicine,
biomedicine,
evidence-based medicine, or modern medicine" (see the article on
scientific medicine).
[34]
Use of the term remains common among homeopaths and has spread to
other alternative medicine practices. The meaning implied by the label
has never been accepted by conventional medicine and is considered
pejorative.
[35] More recently, some sources have used the term "allopathic", particularly American sources wishing to distinguish between
Doctors of Medicine (MD) and Doctors of Osteopathic Medicine (DO) in the United States.
[32][36] William Jarvis, an expert on alternative medicine and public health,
[37]
states that "although many modern therapies can be construed to conform
to an allopathic rationale (e.g., using a laxative to relieve
constipation), standard medicine has never paid allegiance to an
allopathic principle" and that the label "allopath" was from the start
"considered highly derisive by regular medicine".
[38]
Many conventional medical treatments clearly do not fit the nominal definition of
allopathy, as they seek to prevent illness, or remove its cause.
[39][40]
CAM
CAM is an abbreviation of complementary and alternative medicine.
[41][42] It has also been called sCAM or SCAM with the addition of "so-called" or "supplements".
[43][44]
The words balance and holism are often used, claiming to take into
account a "whole" person, in contrast to the supposed reductionism of
medicine. Due to its many names the field has been criticized for
intense
rebranding of what are essentially the same practices: as soon as one name is declared synonymous with
quackery, a new name is chosen.
[16]
Traditional medicine
Traditional medicine refers to the pre-scientific practices of
a certain culture, contrary to what is typically practiced in other
cultures where medical science dominates.
"
Eastern medicine" typically refers to the traditional medicines of Asia where conventional bio-medicine penetrated much later.
Problems with definition
Prominent members of the science
[45][46] and biomedical science community
[3]
say that it is not meaningful to define an alternative medicine that is
separate from a conventional medicine, that the expressions
"conventional medicine", "alternative medicine", "complementary
medicine", "integrative medicine", and "holistic medicine" do not refer
to any medicine at all.
Others in both the biomedical and CAM communities say that CAM
cannot
be precisely defined because of the diversity of theories and practices
it includes, and because the boundaries between CAM and biomedicine
overlap, are porous, and change.
The expression "complementary and alternative medicine" (CAM) resists
easy definition because the health systems and practices it refers to
are diffuse, and its boundaries poorly defined.
[14][n 8] Healthcare practices categorized as alternative may differ in their historical origin, theoretical basis,
diagnostic technique,
therapeutic practice and in their relationship to the medical mainstream. Some alternative therapies, including
traditional Chinese medicine (TCM) and
Ayurveda, have antique origins in East or South Asia and are entirely alternative medical systems;
[52]
others, such as homeopathy and chiropractic, have origins in Europe or
the United States and emerged in the eighteenth and nineteenth
centuries. Some, such as
osteopathy and chiropractic, employ manipulative physical methods of treatment; others, such as
meditation and
prayer, are based on
mind-body interventions. Treatments considered alternative in one location may be considered conventional in another.
[55] Thus, chiropractic is not considered alternative in Denmark and likewise
osteopathic medicine is no longer thought of as an alternative therapy in the United States.
[55]
Critics say the expression is deceptive because it implies there is
an effective alternative to science-based medicine, and that
complementary
is deceptive because it implies that the treatment increases the
effectiveness of (complements) science-based medicine, while alternative
medicines that have been tested nearly always have no measurable
positive effect compared to a
placebo.
[4][56][57][58]
Different types of definitions
One common feature of all definitions of alternative medicine is its designation as "other than" conventional medicine. For example, the widely referenced descriptive definition of complementary and alternative medicine devised by the
US National Center for Complementary and Integrative Health (NCCIH) of the
National Institutes of Health (NIH),
states that it is "a group of diverse medical and health care systems,
practices, and products that are not generally considered part of
conventional medicine".
[61]
For conventional medical practitioners, it does not necessarily follow
that either it or its practitioners would no longer be considered
alternative.
[n 9]
Some definitions seek to specify alternative medicine in terms of its social and political marginality to mainstream healthcare.
[64]
This can refer to the lack of support that alternative therapies
receive from the medical establishment and related bodies regarding
access to
research funding, sympathetic coverage in the
medical press, or inclusion in the standard
medical curriculum.
[64] In 1993, the
British Medical Association (BMA), one among many professional organizations who have attempted to define alternative medicine, stated that it
[n 10]
referred to "...those forms of treatment which are not widely used by
the conventional healthcare professions, and the skills of which are not
taught as part of the undergraduate curriculum of conventional medical
and paramedical healthcare courses".
[65] In a US context, an influential definition coined in 1993 by the Harvard-based physician,
[66] David M. Eisenberg,
[67]
characterized alternative medicine "as interventions neither taught
widely in medical schools nor generally available in US hospitals".
[68]
These descriptive definitions are inadequate in the present-day when
some conventional doctors offer alternative medical treatments and CAM
introductory courses or modules can be offered as part of standard
undergraduate medical training;
[69] alternative medicine is taught in more than 50 per cent of
US medical schools and increasingly
US health insurers are willing to provide reimbursement for CAM therapies. In 1999, 7.7% of US hospitals reported using some form of CAM therapy; this proportion had risen to 37.7% by 2008.
[71]
An expert panel at a conference hosted in 1995 by the US Office for Alternative Medicine (OAM),
[72][n 11] devised a
theoretical definition[72]
of alternative medicine as "a broad domain of healing resources ...
other than those intrinsic to the politically dominant health system of a
particular society or culture in a given historical period".
[74] This definition has been widely adopted by CAM researchers,
[72] cited by official government bodies such as the UK Department of Health,
[75] attributed as the definition used by the
Cochrane Collaboration,
[76] and, with some modification,
[dubious – discuss] was preferred in the 2005 consensus report of the
US Institute of Medicine,
Complementary and Alternative Medicine in the United States.
[n 2]
The 1995 OAM conference definition, an expansion of Eisenberg's 1993
formulation, is silent regarding questions of the medical effectiveness
of alternative therapies.
[77] Its proponents hold that it thus avoids
relativism
about differing forms of medical knowledge and, while it is an
essentially political definition, this should not imply that the
dominance of mainstream
biomedicine is solely due to political forces.
[77] According to this definition, alternative and
mainstream medicine
can only be differentiated with reference to what is "intrinsic to the
politically dominant health system of a particular society of culture".
[78] However, there is neither a reliable method to distinguish between cultures and
subcultures, nor to attribute them as dominant or subordinate, nor any accepted criteria to determine the dominance of a cultural entity.
[78]
If the culture of a politically dominant healthcare system is held to
be equivalent to the perspectives of those charged with the medical
management of leading healthcare institutions and programs, the
definition fails to recognize the potential for division either within
such an elite or between a healthcare elite and the wider population.
[78]
Normative
definitions distinguish alternative medicine from the biomedical
mainstream in its provision of therapies that are unproven, unvalidated,
or ineffective and support of theories with no recognized scientific
basis. These definitions characterize practices as constituting alternative medicine when, used independently or in place of
evidence-based medicine, they are put forward as having the healing effects of medicine, but are not based on
evidence gathered with the
scientific method.
[1][3][27][28][61][80] Exemplifying this perspective, a 1998 editorial co-authored by
Marcia Angell, a former editor of
The New England Journal of Medicine, argued that:
It is time for the scientific community to stop giving alternative
medicine a free ride. There cannot be two kinds of medicine –
conventional and alternative. There is only medicine that has been
adequately tested and medicine that has not, medicine that works and
medicine that may or may not work. Once a treatment has been tested
rigorously, it no longer matters whether it was considered alternative
at the outset. If it is found to be reasonably safe and effective, it
will be accepted. But assertions, speculation, and testimonials do not
substitute for evidence. Alternative treatments should be subjected to
scientific testing no less rigorous than that required for conventional
treatments.[3]
This line of division has been subject to criticism, however, as not
all forms of standard medical practice have adequately demonstrated
evidence of benefit,
[n 4][81]
and it is also unlikely in most instances that conventional therapies,
if proven to be ineffective, would ever be classified as CAM.
[72]
Similarly, the public information website maintained by the
National Health and Medical Research Council
(NHMRC) of the Commonwealth of Australia uses the acronym "CAM" for a
wide range of health care practices, therapies, procedures and devices
not within the domain of conventional medicine. In the Australian
context this is stated to include acupuncture; aromatherapy;
chiropractic; homeopathy; massage; meditation and relaxation therapies;
naturopathy; osteopathy; reflexology, traditional Chinese medicine; and
the use of vitamin supplements.
[83]
The
Danish National Board of Health's
"Council for Alternative Medicine" (Sundhedsstyrelsens Råd for
Alternativ Behandling (SRAB)), an independent institution under the
National Board of Health (Danish:
Sundhedsstyrelsen), uses the term "alternative medicine" for:
- Treatments performed by therapists that are not authorized healthcare professionals.
- Treatments performed by authorized healthcare professionals, but
those based on methods otherwise used mainly outside the healthcare
system. People without a healthcare authorisation are [also] allowed to
perform the treatments.[84]
Proponents of an
evidence-base for medicine[n 12][86][87][88][89] such as the Cochrane Collaboration (founded in 1993 and from 2011 providing input for WHO resolutions) take a position that
all
systematic reviews of treatments, whether "mainstream" or
"alternative", ought to be held to the current standards of scientific
method.
[90] In a study titled
Development
and classification of an operational definition of complementary and
alternative medicine for the Cochrane Collaboration (2011) it was proposed that indicators that a therapy is accepted include government licensing of practitioners, coverage by
health insurance,
statements of approval by government agencies, and recommendation as
part of a practice guideline; and that if something is currently a
standard, accepted therapy, then it is not likely to be widely
considered as CAM.
[72]
Types
Alternative medicine consists of a wide range of health care
practices, products, and therapies. The shared feature is a claim to
heal that is not based on the scientific method. Alternative medicine
practices are diverse in their foundations and methodologies.
[61]
Alternative medicine practices may be classified by their cultural
origins or by the types of beliefs upon which they are based. Methods may incorporate or be based on traditional medicinal practices of a particular culture, folk knowledge, superstition, spiritual beliefs, belief in
supernatural energies (
antiscience),
pseudoscience,
errors in reasoning,
propaganda, fraud, new or different concepts of health and disease, and
any bases other than being proven by scientific methods.
Different cultures may have their own unique traditional or belief
based practices developed recently or over thousands of years, and
specific practices or entire systems of practices.
Unscientific belief systems
Alternative medicine, such as using
naturopathy or
homeopathy in place of
conventional medicine, is based on belief systems not grounded in science.
[61]
|
Proposed mechanism |
Issues |
| Naturopathy |
Naturopathic medicine is based on a belief that the body heals itself using a supernatural vital energy that guides bodily processes.[92] |
In conflict with the paradigm of evidence-based medicine.[93] Many naturopaths have opposed vaccination,[94] and "scientific evidence does not support claims that naturopathic medicine can cure cancer or any other disease".[95] |
| Homeopathy |
A belief that a substance that causes the symptoms of a disease in healthy people cures similar symptoms in sick people.[n 13] |
Developed before knowledge of atoms and molecules,
or of basic chemistry, which shows that repeated dilution as practiced
in homeopathy produces only water, and that homeopathy is not
scientifically valid.[97][98][99][100] |
Supplements
"
They told me if I took 1000 pills at night I should be quite another thing in the morning", an early 19th-century satire on
Morison's Vegetable Pills, an alternative medicine supplement.
Traditional ethnic systems
Alternative medical systems may be based on
traditional medicine practices, such as
traditional Chinese medicine (TCM),
Ayurveda in India, or practices of other cultures around the world.
[61] Some useful applications of traditional medicines have been researched
and accepted within ordinary medicine, however the underlying belief
systems are seldom scientific and are not accepted.
Traditional medicine is considered alternative when it is used
outside its home region; or when it is used together with or instead of
known functional treatment; or when it can be reasonably expected that
the patient or practitioner knows or should know that it will not work –
such as knowing that the practice is based on superstition.
Since ancient times, in many parts of the world a number of herbs reputed to possess abortifacient properties have been used in
folk medicine. Among these are:
tansy,
pennyroyal,
black cohosh, and the now-extinct
silphium.
[101]:44–47, 62–63, 154–55, 230–31 Historian of science
Ann Hibner Koblitz has written of the probable
protoscientific
origins of this folk knowledge in observation of farm animals. Women
who knew that grazing on certain plants would cause an animal to abort
(with negative economic consequences for the farm) would be likely to
try out those plants on themselves in order to avoid an unwanted
pregnancy.
[102]:120
However, modern users of these plants often lack knowledge of the proper preparation and dosage. The historian of medicine
John Riddle has spoken of the "broken chain of knowledge" caused by urbanization and modernization,
[101]:167–205
and Koblitz has written that "folk knowledge about effective
contraception techniques often disappears over time or becomes
inextricably mixed with useless or harmful practices."
[102]:vii The ill-informed or indiscriminant use of herbs as abortifacients can cause serious and even lethal side-effects.
|
Claims |
Issues |
| Traditional Chinese medicine |
Traditional practices and beliefs from China, together with
modifications made by the Communist party make up TCM. Common practices
include herbal medicine, acupuncture (insertion of needles in the body at specified points), massage (Tui na), exercise (qigong), and dietary therapy. |
The practices are based on belief in a supernatural energy called qi, considerations of Chinese Astrology and Chinese numerology,
traditional use of herbs and other substances found in China – a belief
that the tongue contains a map of the body that reflects changes in the
body, and an incorrect model of the anatomy and physiology of internal
organs.[4][105][106][107][108][109] |
| Ayurveda |
Traditional medicine of India. Ayurveda believes in the existence of three elemental substances, the doshas
(called Vata, Pitta and Kapha), and states that a balance of the doshas
results in health, while imbalance results in disease. Such
disease-inducing imbalances can be adjusted and balanced using
traditional herbs, minerals and heavy metals. Ayurveda stresses the use
of plant-based medicines and treatments, with some animal products, and
added minerals, including sulfur, arsenic, lead and copper sulfate[clarification needed]. |
Safety concerns have been raised about Ayurveda, with two U.S.
studies finding about 20 percent of Ayurvedic Indian-manufactured patent medicines contained toxic levels of heavy metals such as lead, mercury and arsenic.
A 2015 study of users in the United States also found elevated blood
lead levels in 40 percent of those tested. Other concerns include the
use of herbs containing toxic compounds and the lack of quality control
in Ayurvedic facilities. Incidents of heavy metal poisoning have been attributed to the use of these compounds in the United States.[15][112][113][114][115][116] |
Supernatural energies
Bases
of belief may include belief in existence of supernatural energies
undetected by the science of physics, as in biofields, or in belief in
properties of the energies of physics that are inconsistent with the
laws of physics, as in energy medicine.
|
Claims |
Issues |
| Biofield therapy |
Intended to influence energy fields that, it is purported, surround and penetrate the body.[61] |
Writers such as noted astrophysicist and advocate of skeptical thinking (Scientific skepticism) Carl Sagan
(1934–1996) have described the lack of empirical evidence to support
the existence of the putative energy fields on which these therapies are
predicated. |
| Bioelectromagnetic therapy |
Use verifiable electromagnetic fields, such as pulsed fields,
alternating-current, or direct-current fields in an unconventional
manner.[61] |
Asserts that magnets can be used to defy the laws of physics to influence health and disease. |
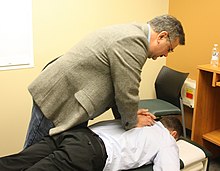
| Chiropractic |
Spinal manipulation aims to treat "vertebral subluxations" which are claimed to put pressure on nerves. |
Chiropractic was developed in the belief that manipulating the spine affects the flow of a supernatural vital energy and thereby affects health and disease. Vertebral subluxation is a pseudoscientific concept and has not been proven to exist. |
| Reiki |
Practitioners place their palms on the patient near Chakras
that they believe are centers of supernatural energies in the belief
that these supernatural energies can transfer from the practitioner's
palms to heal the patient. |
Lacks credible scientific evidence.[118] |
Holistic therapy
|
Claims |
Issues |
| Mind-body medicine |
The mind can affect "bodily functions and symptoms" and there is an interconnection between the mind, body, and spirit. |
|
Herbal remedies and other substances used
Substance based practices use substances found in nature such as
herbs, foods, non-vitamin supplements and megavitamins, animal and
fungal products, and minerals, including use of these products in
traditional medical practices that may also incorporate other methods.
Examples include healing claims for nonvitamin supplements,
fish oil,
Omega-3 fatty acid,
glucosamine,
echinacea,
flaxseed oil, and
ginseng.
[121] Herbal medicine, or
phytotherapy, includes not just the use of plant products, but may also include the use of animal and mineral products.
[119]
It is among the most commercially successful branches of alternative
medicine, and includes the tablets, powders and elixirs that are sold as
"nutritional supplements".
[119]
Only a very small percentage of these have been shown to have any
efficacy, and there is little regulation as to standards and safety of
their contents.
[119] This may include use of known toxic substances, such as use of the poison
lead in traditional Chinese medicine.
[121]
Religion, faith healing, and prayer
|
Claims |
Issues |
| Christian faith healing |
There is a divine or spiritual intervention in healing. |
Lack of evidence for effectiveness.[122]
Unwanted outcomes, such as death and disability, "have occurred when
faith healing was elected instead of medical care for serious injuries
or illnesses".[123]
A 2001 double-blind study of 799 discharged coronary surgery patients
found that "intercessory prayer had no significant effect on medical
outcomes after hospitalization in a coronary care unit."[124] |
| Shamanism |
A practitioner can reach an altered states of consciousness in order to encounter and interact with the spirit world or channel supernatural energies in the belief that they can heal. |
|
NCCIH classification
A US agency, National Center on Complementary and Integrative Health (
NCCIH),
has created a classification system for branches of complementary and
alternative medicine that divides them into five major groups. These
groups have some overlap, and distinguish two types of
energy medicine:
veritable which involves scientifically observable energy (including
magnet therapy,
colorpuncture and
light therapy) and
putative, which invokes physically undetectable or unverifiable energy.
[125] None of these energies have any evidence to support that they effect the body in any positive or health promoting way.
[30]
- Whole medical systems: Cut across more than one of the other groups;
examples include traditional Chinese medicine, naturopathy, homeopathy,
and ayurveda.
- Mind-body interventions: Explore the interconnection between the
mind, body, and spirit, under the premise that they affect "bodily
functions and symptoms". A connection between mind and body is
conventional medical fact, and this classification does not include
therapies with proven function such as cognitive behavioral therapy.
- "Biology"-based practices: Use substances found in nature such as
herbs, foods, vitamins, and other natural substances. (Note that as used
here, "biology" does not refer to the science of biology,
but is a usage newly coined by NCCIH in the primary source used for
this article. "Biology-based" as coined by NCCIH may refer to chemicals
from a nonbiological source, such as use of the poison lead in traditional Chinese medicine, and to other nonbiological substances.)
- Manipulative and body-based practices: feature manipulation or
movement of body parts, such as is done in bodywork, chiropractic, and
osteopathic manipulation.
- Energy medicine: is a domain that deals with putative and verifiable energy fields:
- Biofield
therapies are intended to influence energy fields that are purported to
surround and penetrate the body. The existence of such energy fields
have been disproven.
- Bioelectromagnetic-based
therapies use verifiable electromagnetic fields, such as pulsed fields,
alternating-current, or direct-current fields in an non-scientific
manner.
History
The history of alternative medicine may refer to the history of a
group of diverse medical practices that were collectively promoted as
"alternative medicine" beginning in the 1970s, to the collection of
individual histories of members of that group, or to the history of
western medical practices that were labeled "irregular practices" by the
western medical establishment.
[4][126][127][128][129] It includes the histories of
complementary medicine and of
integrative medicine.
Before the 1970s, western practitioners that were not part of the
increasingly science-based medical establishment were referred to
"irregular practitioners", and were dismissed by the medical
establishment as unscientific and as practicing
quackery.
[126][127] Until the 1970s, irregular practice became increasingly marginalized as
quackery
and fraud, as western medicine increasingly incorporated scientific
methods and discoveries, and had a corresponding increase in success of
its treatments.
[128]
In the 1970s, irregular practices were grouped with traditional
practices of nonwestern cultures and with other unproven or disproven
practices that were not part of biomedicine, with the entire group
collectively marketed and promoted under the single expression
"alternative medicine".
Use of alternative medicine in the west began to rise following the
counterculture movement of the 1960s, as part of the rising
new age movement of the 1970s.
[4][131][132] This was due to misleading
mass marketing of "alternative medicine" being an effective "alternative" to biomedicine, changing social attitudes about not using
chemicals and challenging
the establishment and
authority of any kind, sensitivity to giving equal measure to beliefs and practices of other cultures (
cultural relativism), and growing frustration and desperation by patients about limitations and
side effects of
science-based medicine.
[4][127][128][129][130][132][133] At the same time, in 1975, the
American Medical Association,
which played the central role in fighting quackery in the United
States, abolished its quackery committee and closed down its Department
of Investigation.
[126]:xxi[133]
By the early to mid 1970s the expression "alternative medicine" came
into widespread use, and the expression became mass marketed as a
collection of "natural" and effective treatment "alternatives" to
science-based biomedicine.
[4][133][134][135] By 1983, mass marketing of "alternative medicine" was so pervasive that the
British Medical Journal
(BMJ) pointed to "an apparently endless stream of books, articles, and
radio and television programmes urge on the public the virtues of
(alternative medicine) treatments ranging from meditation to drilling a
hole in the skull to let in more oxygen".
[133]
Medical education
Mainly as a result of reforms following the Flexner Report of 1910
[136] medical education in established
medical schools in the US has generally not included alternative medicine as a teaching topic.
[n 14]
Typically, their teaching is based on current practice and scientific
knowledge about: anatomy, physiology, histology, embryology,
neuroanatomy, pathology, pharmacology, microbiology and immunology.
[138] Medical schools' teaching includes such topics as doctor-patient communication, ethics, the art of medicine,
[139] and engaging in complex clinical reasoning (medical decision-making).
[140]
Writing in 2002, Snyderman and Weil remarked that by the early
twentieth century the Flexner model had helped to create the
20th-century academic health center, in which education, research, and
practice were inseparable. While this had much improved medical practice
by defining with increasing certainty the
pathophysiological
basis of disease, a single-minded focus on the pathophysiological had
diverted much of mainstream American medicine from clinical conditions
that were not well understood in mechanistic terms, and were not
effectively treated by conventional therapies.
[141]
By 2001 some form of CAM training was being offered by at least 75 out of 125 medical schools in the US.
[142] Exceptionally, the School of Medicine of the
University of Maryland, Baltimore includes a research institute for integrative medicine (a member entity of the Cochrane Collaboration). Medical schools are responsible for conferring medical degrees, but a
physician typically may not legally practice medicine until licensed by
the local government authority. Licensed
physicians in the US who have attended one of the established medical schools there have usually graduated Doctor of Medicine (MD).
[144] All states require that applicants for MD licensure be graduates of an approved medical school and complete the
United States Medical Licensing Exam (USMLE).
[144]
Efficacy
There is a general scientific consensus that alternative therapies lack the requisite
scientific validation, and their
effectiveness is either
unproved or
disproved.
[1][4][145][146]
Many of the claims regarding the efficacy of alternative medicines are
controversial, since research on them is frequently of low quality and
methodologically flawed.
Selective publication bias,
marked differences in product quality and standardisation, and some
companies making unsubstantiated claims call into question the claims of
efficacy of isolated examples where there is evidence for alternative
therapies.
[148]
The Scientific Review of Alternative Medicine points to
confusions in the general population – a person may attribute
symptomatic relief to an otherwise-ineffective therapy just because they
are taking something (the placebo effect); the natural recovery from or
the cyclical nature of an illness (the
regression fallacy)
gets misattributed to an alternative medicine being taken; a person not
diagnosed with science-based medicine may never originally have had a
true illness diagnosed as an alternative disease category.
[149]
Edzard Ernst characterized the evidence for many alternative techniques as weak, nonexistent, or negative
[150]
and in 2011 published his estimate that about 7.4% were based on "sound
evidence", although he believes that may be an overestimate.
[151]
Ernst has concluded that 95% of the alternative treatments he and his
team studied, including acupuncture, herbal medicine, homeopathy, and
reflexology, are "statistically indistinguishable from placebo
treatments", but he also believes there is something that conventional
doctors can usefully learn from the chiropractors and homeopath: this is
the therapeutic value of the placebo effect, one of the strangest
phenomena in medicine.
[152][153]
In 2003, a project funded by the CDC identified 208 condition-treatment pairs, of which 58% had been studied by at least one
randomized controlled trial (RCT), and 23% had been assessed with a
meta-analysis.
[154] According to a 2005 book by a US
Institute of Medicine panel, the number of RCTs focused on CAM has risen dramatically.
As of 2005, the
Cochrane Library
had 145 CAM-related Cochrane systematic reviews and 340 non-Cochrane
systematic reviews. An analysis of the conclusions of only the 145
Cochrane reviews was done by two readers. In 83% of the cases, the
readers agreed. In the 17% in which they disagreed, a third reader
agreed with one of the initial readers to set a rating. These studies
found that, for CAM, 38.4% concluded positive effect or possibly
positive (12.4%), 4.8% concluded no effect, 0.7% concluded harmful
effect, and 56.6% concluded insufficient evidence. An assessment of
conventional treatments found that 41.3% concluded positive or possibly
positive effect, 20% concluded no effect, 8.1% concluded net harmful
effects, and 21.3% concluded insufficient evidence. However, the CAM
review used the more developed 2004 Cochrane database, while the
conventional review used the initial 1998 Cochrane database.
In the same way as for conventional therapies, drugs, and
interventions, it can be difficult to test the efficacy of alternative
medicine in
clinical trials. In instances where an established, effective, treatment for a condition is already available, the
Helsinki Declaration
states that withholding such treatment is unethical in most
circumstances. Use of standard-of-care treatment in addition to an
alternative technique being tested may produce confounded or
difficult-to-interpret results.
[156]
Cancer researcher
Andrew J. Vickers has stated:
Contrary to much popular and scientific writing, many alternative cancer treatments
have been investigated in good-quality clinical trials, and they have
been shown to be ineffective. The label "unproven" is inappropriate for
such therapies; it is time to assert that many alternative cancer
therapies have been "disproven".[157]
Mechanism of action
Placebo effect
A research methods expert and author of
Snake Oil Science,
R. Barker Bausell, has stated that "it's become politically correct to investigate nonsense."
[158]
There are concerns that just having NIH support is being used to give
unfounded "legitimacy to treatments that are not legitimate."
Use of placebos to achieve a
placebo effect
in integrative medicine has been criticized as, "...diverting research
time, money, and other resources from more fruitful lines of
investigation in order to pursue a theory that has no basis in biology."
[57][58]
Another critic has argued that academic proponents of
integrative medicine sometimes recommend misleading patients by using known placebo treatments to achieve a placebo effect.
[n 15]
However, a 2010 survey of family physicians found that 56% of
respondents said they had used a placebo in clinical practice as well.
Eighty-five percent of respondents believed placebos can have both
psychological and physical benefits.
[161]
Integrative medicine has been criticized in that its practitioners, trained in science-based medicine, deliberately mislead patients by pretending
placebos are not. "
quackademic medicine" is a pejorative term used for
integrative medicine, which medical professionals consider an infiltration of quackery into academic
science-based medicine.
[58]
An analysis of trends in the criticism of complementary and
alternative medicine (CAM) in five prestigious American medical journals
during the period of reorganization within medicine (1965–1999) was
reported as showing that the medical profession had responded to the
growth of CAM in three phases, and that in each phase, changes in the
medical marketplace had influenced the type of response in the journals.
[162]
Changes included relaxed medical licensing, the development of managed
care, rising consumerism, and the establishment of the USA Office of
Alternative Medicine (later
National Center for Complementary and Alternative Medicine, currently
National Center for Complementary and Integrative Health).
[n 16]
In the "condemnation" phase, from the late 1960s to the early 1970s,
authors had ridiculed, exaggerated the risks, and petitioned the state
to contain CAM; in the "reassessment" phase (mid-1970s through early
1990s), when increased consumer utilization of CAM was prompting
concern, authors had pondered whether patient dissatisfaction and
shortcomings in conventional care contributed to the trend; in the
"integration" phase of the 1990s physicians began learning to work
around or administer CAM, and the subjugation of CAM to scientific
scrutiny had become the primary means of control.
[citation needed]
Use and regulation
Appeal
Alternative therapies often make bombastic claims, and frequently
include anecdotes from healthy-looking individuals claiming successful
treatment.
Practitioners of complementary medicine usually discuss and advise
patients as to available alternative therapies. Patients often express
interest in mind-body complementary therapies because they offer a
non-drug approach to treating some health conditions.
[164]
In addition to the social-cultural underpinnings of the popularity of
alternative medicine, there are several psychological issues that are
critical to its growth. One of the most critical is the placebo effect –
a well-established observation in medicine.
[165] Related to it are similar psychological effects, such as the will to believe,
[166] cognitive biases that help maintain self-esteem and promote harmonious social functioning,
[166] and the
post hoc, ergo propter hoc fallacy.
[166]
Marketing
Edzard Ernst,
a leading authority on scientific study of alternative treatments and
diagnoses, and the first university professor of Complementary and
Alternative Medicine. Here in 2012, promoting his book
Trick or Treatment co-written with
Simon Singh.
The popularity of complementary & alternative medicine (CAM) may be related to other factors that
Edzard Ernst mentioned in an interview in
The Independent:
Why is it so popular, then? Ernst blames the providers, customers and
the doctors whose neglect, he says, has created the opening into which
alternative therapists have stepped. "People are told lies. There are 40
million websites and 39.9 million tell lies, sometimes outrageous lies.
They mislead cancer patients, who are encouraged not only to pay their
last penny but to be treated with something that shortens their lives.
"At the same time, people are gullible. It needs gullibility for the
industry to succeed. It doesn't make me popular with the public, but
it's the truth.[167]
Paul Offit
proposed that "alternative medicine becomes quackery" in four ways: by
recommending against conventional therapies that are helpful, promoting
potentially harmful therapies without adequate warning, draining
patients' bank accounts, or by promoting "magical thinking."
[45]
Friendly and colorful images of herbal treatments may look less
threatening or dangerous when compared to conventional medicine. This is
an intentional marketing strategy.
Social factors
Authors
have speculated on the socio-cultural and psychological reasons for the
appeal of alternative medicines among the minority using them
in lieu
of conventional medicine. There are several socio-cultural reasons for
the interest in these treatments centered on the low level of
scientific literacy among the public at large and a concomitant increase in
antiscientific attitudes and
new age mysticism.
[166] Related to this are vigorous
marketing[168] of extravagant claims by the alternative medical community combined with inadequate media scrutiny and attacks on critics.
[166][169]
There is also an increase in
conspiracy theories
toward conventional medicine and pharmaceutical companies, mistrust of
traditional authority figures, such as the physician, and a dislike of
the current delivery methods of scientific biomedicine, all of which
have led patients to seek out alternative medicine to treat a variety of
ailments.
[169] Many patients lack access to contemporary medicine, due to a lack of private or public
health insurance, which leads them to seek out lower-cost alternative medicine.
[170] Medical doctors are also aggressively marketing alternative medicine to profit from this market.
[168]
Patients can be averse to the painful, unpleasant, and sometimes-dangerous
side effects of biomedical treatments. Treatments for severe diseases such as
cancer and
HIV infection have well-known, significant side-effects. Even low-risk medications such as
antibiotics can have potential to cause life-threatening
anaphylactic
reactions in a very few individuals. Many medications may cause minor
but bothersome symptoms such as cough or upset stomach. In all of these
cases, patients may be seeking out alternative treatments to avoid the
adverse effects of conventional treatments.
[166][169]
Prevalence of use
Complementary and alternative medicine
(CAM) has been described as a broad domain of healing resources that
encompasses all health systems, modalities, and practices and their
accompanying theories and beliefs, other than those intrinsic to the
politically dominant health system of a particular society or culture in
a given historical period. CAM includes all such practices and ideas
self-defined by their users as preventing or treating illness or
promoting health and well-being. Boundaries within CAM and between the
CAM domain and that of the dominant system are not always sharp or
fixed.
According to recent research, the increasing popularity of the CAM
needs to be explained by moral convictions or lifestyle choices rather
than by economic reasoning.
[171]
In
developing nations, access to essential medicines is severely restricted by lack of resources and
poverty.
Traditional remedies,
often closely resembling or forming the basis for alternative remedies,
may comprise primary healthcare or be integrated into the healthcare
system. In Africa, traditional medicine is used for 80% of primary
healthcare, and in developing nations as a whole over one-third of the
population lack access to essential medicines.
[172]
Some have proposed adopting a
prize system to reward medical research.
[173]
However, public funding for research exists. Increasing the funding for
research on alternative medicine techniques is the purpose of the
US National Center for Complementary and Alternative Medicine.
NCCIH and its predecessor, the Office of Alternative Medicine, have
spent more than US$2.5 billion on such research since 1992; this
research has largely not demonstrated the efficacy of alternative
treatments.
That alternative medicine has been on the rise "in countries where
Western science and scientific method generally are accepted as the
major foundations for healthcare, and 'evidence-based' practice is the
dominant paradigm" was described as an "enigma" in the Medical Journal
of Australia.
[177]
In the US
In the United States, the 1974
Child Abuse Prevention and Treatment Act (CAPTA) required that for states to receive federal money, they had to grant religious exemptions to
child neglect and
abuse laws regarding religion-based healing practices.
[178] Thirty-one states have child-abuse religious exemptions.
[179]
The use of alternative medicine in the US has increased,
[1][180]
with a 50 percent increase in expenditures and a 25 percent increase in
the use of alternative therapies between 1990 and 1997 in America.
[180] Americans spend many billions on the therapies annually.
[180]
Most Americans used CAM to treat and/or prevent musculoskeletal
conditions or other conditions associated with chronic or recurring
pain.
[170] In America, women were more likely than men to use CAM, with the biggest difference in use of
mind-body therapies including prayer specifically for health reasons".
[170] In 2008, more than 37% of American hospitals offered alternative therapies, up from 27 percent in 2005, and 25% in 2004.
[181][182] More than 70% of the hospitals offering CAM were in urban areas.
[182]
A survey of Americans found that 88 percent thought that "there are
some good ways of treating sickness that medical science does not
recognize".
[1] Use of magnets was the most common tool in
energy medicine in America, and among users of it, 58 percent described it as at least "sort of
scientific", when it is not at all scientific.
[1] In 2002, at least 60 percent of US medical schools have at least some class time spent teaching alternative therapies.
[1]
"Therapeutic touch", was taught at more than 100 colleges and
universities in 75 countries before the practice was debunked by a
nine-year-old child for a school science project.
[1][118]
Prevalence of use of specific therapies
The most common CAM therapies used in the US in 2002 were prayer (45%),
herbalism (19%),
breathing meditation (12%),
meditation (8%),
chiropractic medicine (8%),
yoga (5–6%),
body work (5%),
diet-based therapy (4%),
progressive relaxation (3%),
mega-vitamin therapy (3%) and
Visualization (2%)
[170][183]
In Britain, the most often used alternative therapies were
Alexander technique,
Aromatherapy, Bach and other flower remedies, Body work therapies including massage, Counseling stress therapies,
hypnotherapy,
Meditation,
Reflexology,
Shiatsu,
Ayurvedic medicine, Nutritional medicine, and
Yoga.
[184] Ayurvedic medicine remedies are mainly plant based with some use of animal materials. Safety concerns include the use of herbs containing toxic compounds and the lack of quality control in Ayurvedic facilities.
[112][114]
According to the
National Health Service (England),
the most commonly used complementary and alternative medicines (CAM)
supported by the NHS in the UK are: acupuncture, aromatherapy,
chiropractic, homeopathy, massage, osteopathy and clinical hypnotherapy.
[186]
In palliative care
Complementary therapies are often used in
palliative care
or by practitioners attempting to manage chronic pain in patients.
Integrative medicine is considered more acceptable in the
interdisciplinary approach used in palliative care than in other areas
of medicine. "From its early experiences of care for the dying,
palliative care took for granted the necessity of placing patient values
and lifestyle habits at the core of any design and delivery of quality
care at the end of life. If the patient desired complementary therapies,
and as long as such treatments provided additional support and did not
endanger the patient, they were considered acceptable."
[187] The non-pharmacologic interventions of complementary medicine can employ
mind-body interventions designed to "reduce pain and concomitant mood disturbance and increase quality of life."
[188]
Regulation
In Austria and Germany complementary and alternative medicine is mainly in the hands of doctors with
MDs,
[41] and half or more of the American alternative practitioners are licensed MDs.
[189] In Germany herbs are tightly regulated: half are prescribed by doctors and covered by health insurance.
[190]
Some professions of complementary/traditional/alternative medicine, such as
chiropractic, have achieved full regulation in North America and other parts of the world
and are regulated in a manner similar to that governing science-based
medicine. In contrast, other approaches may be partially recognized and
others have no regulation at all. Regulation and licensing of
alternative medicine ranges widely from country to country, and state to
state.
Government bodies in the US and elsewhere have published information or guidance about alternative medicine. The
U.S. Food and Drug Administration (FDA), has issued online warnings for consumers about medication health fraud.
[192] This includes a section on Alternative Medicine Fraud,
[193] such as a warning that Ayurvedic products generally have not been approved by the FDA before marketing.
[194]
Risks and problems
Adequacy of regulation and CAM safety
Many
of the claims regarding the safety and efficacy of alternative medicine
are controversial. Some alternative treatments have been associated
with unexpected side effects, which can be fatal.
[195]
A commonly voiced concerns about complementary alternative medicine
(CAM) is the way it's regulated. There have been significant
developments in how CAMs should be assessed prior to re-sale in the
United Kingdom and the European Union (EU) in the last 2 years. Despite
this, it has been suggested that current regulatory bodies have been
ineffective in preventing deception of patients as many companies have
re-labelled their drugs to avoid the new laws.
[196]
There is no general consensus about how to balance consumer protection
(from false claims, toxicity, and advertising) with freedom to choose
remedies.
Advocates of CAM suggest that regulation of the industry will
adversely affect patients looking for alternative ways to manage their
symptoms, even if many of the benefits may represent the placebo affect.
[197]
Some contend that alternative medicines should not require any more
regulation than over-the-counter medicines that can also be toxic in
overdose (such as paracetamol).
[198]
Interactions with conventional pharmaceuticals
Forms
of alternative medicine that are biologically active can be dangerous
even when used in conjunction with conventional medicine. Examples
include immuno-augmentation therapy, shark cartilage, bioresonance
therapy, oxygen and ozone therapies, and insulin potentiation therapy.
Some herbal remedies can cause dangerous interactions with chemotherapy
drugs, radiation therapy, or anesthetics during surgery, among other
problems.
[42]
An anecdotal example of these dangers was reported by Associate
Professor Alastair MacLennan of Adelaide University, Australia regarding
a patient who almost bled to death on the operating table after
neglecting to mention that she had been taking "natural" potions to
"build up her strength" before the operation, including a powerful
anticoagulant that nearly caused her death.
[199]
To
ABC Online, MacLennan also gives another possible mechanism:
And lastly [sic]
there's the cynicism and disappointment and depression that some
patients get from going on from one alternative medicine to the next,
and they find after three months the placebo effect wears off, and
they're disappointed and they move on to the next one, and they're
disappointed and disillusioned, and that can create depression and make
the eventual treatment of the patient with anything effective difficult,
because you may not get compliance, because they've seen the failure so
often in the past.[200]
Side-effects
Conventional treatments are subjected to testing for undesired
side-effects,
whereas alternative treatments, in general, are not subjected to such
testing at all. Any treatment – whether conventional or alternative –
that has a biological or psychological effect on a patient may also have
potential to possess dangerous biological or psychological
side-effects. Attempts to refute this fact with regard to alternative
treatments sometimes use the
appeal to nature
fallacy, i.e., "That which is natural cannot be harmful." Specific
groups of patients such as patients with impaired hepatic or renal
function are more susceptible to side effects of alternative remedies.
[201][202]
An exception to the normal thinking regarding side-effects is
Homeopathy. Since 1938, the
U.S. Food and Drug Administration (FDA) has regulated homeopathic products in "several significantly different ways from other drugs."
[203]
Homeopathic preparations, termed "remedies", are extremely dilute,
often far beyond the point where a single molecule of the original
active (and possibly toxic) ingredient is likely to remain. They are,
thus, considered safe on that count, but "their products are exempt from
good manufacturing practice requirements related to expiration dating
and from finished product testing for identity and strength", and their
alcohol concentration may be much higher than allowed in conventional
drugs.
[203]
Treatment delay
Those
having experienced or perceived success with one alternative therapy
for a minor ailment may be convinced of its efficacy and persuaded to
extrapolate that success to some other alternative therapy for a more
serious, possibly life-threatening illness.
[204]
For this reason, critics argue that therapies that rely on the placebo
effect to define success are very dangerous. According to mental health
journalist Scott Lilienfeld in 2002, "unvalidated or scientifically
unsupported mental health practices can lead individuals to forgo
effective treatments" and refers to this as "
opportunity cost". Individuals who spend large amounts of time and money on ineffective
treatments may be left with precious little of either, and may forfeit
the opportunity to obtain treatments that could be more helpful. In
short, even innocuous treatments can indirectly produce negative
outcomes.
[205]
Between 2001 and 2003, four children died in Australia because their
parents chose ineffective naturopathic, homeopathic, or other
alternative medicines and diets rather than conventional therapies.
[206]
Unconventional cancer "cures"
There
have always been "many therapies offered outside of conventional cancer
treatment centers and based on theories not found in
biomedicine.
These alternative cancer cures have often been described as 'unproven,'
suggesting that appropriate clinical trials have not been conducted and
that the therapeutic value of the treatment is unknown." However, "many
alternative cancer treatments have been investigated in good-quality
clinical trials, and they have been shown to be ineffective....The label
'unproven' is inappropriate for such therapies; it is time to assert
that many alternative cancer therapies have been 'disproven'."
[157]
Edzard Ernst has stated:
...any alternative cancer cure is bogus by definition. There will
never be an alternative cancer cure. Why? Because if something looked
halfway promising, then mainstream oncology would scrutinize it, and if
there is anything to it, it would become mainstream almost automatically
and very quickly. All curative "alternative cancer cures" are based on
false claims, are bogus, and, I would say, even criminal.[207]
Rejection of science
| “ |
There is no alternative medicine. There is
only scientifically proven, evidence-based medicine supported by solid
data or unproven medicine, for which scientific evidence is lacking. |
” |
| — P.B. Fontanarosa, Journal of the American Medical Association (1998)[47] |
"CAM", meaning "complementary and alternative medicine", is not as
well researched as conventional medicine, which undergoes intense
research before release to the public.
[208] Funding for research is also sparse making it difficult to do further research for effectiveness of CAM.
[209] Most funding for CAM is funded by government agencies.
[208] Proposed research for CAM are rejected by most private funding agencies because the results of research are not reliable.
[208]
The research for CAM has to meet certain standards from research ethics
committees, which most CAM researchers find almost impossible to meet.
[208] Even with the little research done on it, CAM has not been proven to be effective.
[210]
Steven Novella,
a neurologist at Yale School of Medicine, wrote that government funded
studies of integrating alternative medicine techniques into the
mainstream are "used to lend an appearance of legitimacy to treatments
that are not legitimate."
[159] Marcia Angell considered that critics felt that healthcare practices should be classified based solely on
scientific evidence,
and if a treatment had been rigorously tested and found safe and
effective, science-based medicine will adopt it regardless of whether it
was considered "alternative" to begin with.
[3]
It is possible for a method to change categories (proven vs. unproven),
based on increased knowledge of its effectiveness or lack thereof. A
prominent supporter of this position is
George D. Lundberg, former editor of the
Journal of the American Medical Association (JAMA).
[47]
Writing in 1999 in
CA: A Cancer Journal for Clinicians Barrie R. Cassileth mentioned a 1997 letter to the
US Senate
Subcommittee on Public Health and Safety, which had deplored the lack
of critical thinking and scientific rigor in OAM-supported research, had
been signed by four Nobel Laureates and other prominent scientists.
(This was supported by the
National Institutes of Health (NIH).)
[211]
In March 2009 a staff writer for
the Washington Post
reported that the impending national discussion about broadening access
to health care, improving medical practice and saving money was giving a
group of scientists an opening to propose shutting down the
National Center for Complementary and Alternative Medicine. They quoted one of these scientists,
Steven Salzberg,
a genome researcher and computational biologist at the University of
Maryland, as saying "One of our concerns is that NIH is funding
pseudoscience." They noted that the vast majority of studies were based
on fundamental misunderstandings of
physiology and
disease, and had shown little or no effect.
[159]
Writers such as
Carl Sagan, a noted astrophysicist, advocate of
scientific skepticism and the author of
The Demon-Haunted World: Science as a Candle in the Dark
(1996), have lambasted the lack of empirical evidence to support the
existence of the putative energy fields on which these therapies are
predicated.
Sampson has also pointed out that CAM tolerated
contradiction without thorough reason and experiment.
[212]
Barrett has pointed out that there is a policy at the NIH of never
saying something doesn't work only that a different version or dose
might give different results.
[158]
Barrett also expressed concern that, just because some "alternatives"
have merit, there is the impression that the rest deserve equal
consideration and respect even though most are worthless, since they are
all classified under the one heading of alternative medicine.
[213]
Some critics of alternative medicine are focused upon health fraud,
misinformation, and quackery as public health problems, notably
Wallace Sampson and
Paul Kurtz founders of
Scientific Review of Alternative Medicine and
Stephen Barrett, co-founder of
The National Council Against Health Fraud and webmaster of
Quackwatch.
[214] Grounds for opposing alternative medicine include that:
- It is usually based on religion, tradition, superstition, belief in supernatural energies, pseudoscience, errors in reasoning, propaganda, or fraud.[169][1][4][215]
- Alternative therapies typically lack any scientific validation, and their effectiveness is either unproved or disproved.[4][145][146][dubious – discuss]
- Treatments are not part of the conventional, science-based healthcare system.[12][61][217]
- Research on alternative medicine is frequently of low quality and methodologically flawed.[61]
- Where alternative treatments have replaced conventional
science-based medicine, even with the safest alternative medicines,
failure to use or delay in using conventional science-based medicine has
caused deaths.[205][206]
- Methods may incorporate or base themselves on traditional medicine, folk knowledge,
spiritual beliefs, ignorance or misunderstanding of scientific
principles, errors in reasoning, or newly conceived approaches claiming
to heal.[169][4][219]
Many alternative medical treatments are not
patentable,
[citation needed]
which may lead to less research funding from the private sector. In
addition, in most countries, alternative treatments (in contrast to
pharmaceuticals) can be marketed without any proof of efficacy – also a
disincentive for manufacturers to fund scientific research.
[220]
English evolutionary biologist
Richard Dawkins, in his 2003 book
A Devil's Chaplain, defined alternative medicine as a "set of practices that cannot be tested, refuse to be tested, or consistently fail tests."
[221]
Dawkins argued that if a technique is demonstrated effective in
properly performed trials then it ceases to be alternative and simply
becomes medicine.
[222]
CAM is also often less regulated than conventional medicine.
[208] There are ethical concerns about whether people who perform CAM have the proper knowledge to treat patients.
[208] CAM is often done by non-physicians who do not operate with the same medical licensing laws which govern conventional medicine,
[208] and it is often described as an issue of
non-maleficence.
[223]
According to two writers, Wallace Sampson and K. Butler, marketing is
part of the training required in alternative medicine, and propaganda
methods in alternative medicine have been traced back to those used by
Hitler and
Goebels in their promotion of pseudoscience in medicine.
[4][224]
In November 2011
Edzard Ernst
stated that the "level of misinformation about alternative medicine has
now reached the point where it has become dangerous and unethical. So
far, alternative medicine has remained an ethics-free zone. It is time
to change this."
[225]
Conflicts of interest
Some commentators have said that special consideration must be given to the issue of
conflicts of interest in alternative medicine.
Edzard Ernst
has said that most researchers into alternative medicine are at risk of
"unidirectional bias" because of a generally uncritical belief in their
chosen subject.
[226] Ernst cites as evidence the phenomenon whereby 100% of a sample of
acupuncture trials originating in China had positive conclusions.
[226] David Gorski contrasts
evidence-based medicine,
in which researchers try to disprove hyphotheses, with what he says is
the frequent practice in pseudoscience-based research, of striving to
confirm pre-existing notions.
[227] Harriet Hall
writes that there is a contrast between the circumstances of
alternative medicine practitioners and disinterested scientists: in the
case of acupuncture, for example, an acupuncturist would have "a great
deal to lose" if acupuncture were rejected by research; but the
disinterested skeptic would not lose anything if its effects were
confirmed; rather their change of mind would enhance their skeptical
credentials.
[228]
Gallery
-
-
Indian
Ayurvedic medicine includes a belief that the spiritual balance of mind influences disease.
-
Medicinal herbs in a traditional Spanish market
-
-
Assorted dried plant and animal parts used in traditional Chinese medicine
-
-