From Wikipedia, the free encyclopedia
Brain
control of 3D prosthetic arm movement (hitting targets). This movie was
recorded when the participant controlled the 3D movement of a
prosthetic arm to hit physical targets in a research lab.
In
medicine, a
prosthesis (plural: prostheses; from
Ancient Greek prosthesis, "addition, application, attachment")
is an artificial device that replaces a missing body part, which may be
lost through trauma, disease, or congenital conditions. Prosthetics are
intended to restore the normal functions of the missing body part. Prosthetic
amputee
rehabilitation is primarily coordinated by a prosthetist and an
inter-disciplinary team of health care professionals including
psychiatrists, surgeons, physical therapists, and occupational
therapists. Prosthetics are commonly created with CAD (Computer-Aided
Design), a software interface that helps creators visualize the creation
in a 3D form. But they can also be designed by hand.
Types
A person's
prosthesis should be designed and assembled according to the person's
appearance and functional needs. For instance, a person may need a
transradial prosthesis, but need to choose between an aesthetic
functional device, a myoelectric device, a body-powered device, or an
activity specific device. The person's future goals and economical
capabilities may help them choose between one or more devices.
Craniofacial prostheses
include intra-oral and extra-oral prostheses. Extra-oral prostheses are
further divided into hemifacial, auricular (ear), nasal,
orbital and
ocular. Intra-oral prostheses include
dental prostheses such as
dentures,
obturators, and
dental implants.
Prostheses of the neck include
larynx substitutes,
trachea and upper
esophageal replacements,
Somato prostheses of the torso include
breast prostheses which may be either single or bilateral, full breast devices or
nipple prostheses.
Penile prostheses are used to treat erectile dysfunction.
Limb prostheses
Limb prostheses include both upper- and lower-extremity prostheses.
Upper-extremity prostheses are used at varying levels of
amputation: forequarter, shoulder disarticulation, transhumeral
prosthesis, elbow disarticulation, transradial prosthesis, wrist
disarticulation, full hand, partial hand, finger, partial finger. A
transradial prosthesis is an artificial limb that replaces an arm
missing below the elbow.
Upper limb prostheses can be categorized in three main
categories: Passive devices, Body Powered devices, Externally Powered
(myoelectric) devices. Passive devices can either be passive hands,
mainly used for cosmetic purpose, or passive tools, mainly used for
specific activities (e.g. leisure or vocational). An extensive overview
and classification of passive devices can be found in a literature
review by Maat
et.al.
A passive device can be static, meaning the device has no movable
parts, or it can be adjustable, meaning its configuration can be
adjusted (e.g. adjustable hand opening). Despite the absence of active
grasping, passive devices are very useful in bimanual tasks that require
fixation or support of an object, or for gesticulation in social
interaction. According to scientific data a third of the upper limb
amputees worldwide use a passive prosthetic hand.
Body Powered or cable operated limbs work by attaching a harness and
cable around the opposite shoulder of the damaged arm. The third
category of prosthetic devices available are
myoelectric arms. These work by sensing, via
electrodes, when the muscles in the
upper arm
move, causing an artificial hand to open or close. In the prosthetics
industry, a trans-radial prosthetic arm is often referred to as a "BE"
or below elbow prosthesis.
Lower-extremity prostheses provide replacements at varying
levels of amputation. These include hip disarticulation, transfemoral
prosthesis, knee disarticulation, transtibial prosthesis, Syme's
amputation, foot, partial foot, and toe. The two main subcategories of
lower extremity prosthetic devices are trans-tibial (any amputation
transecting the tibia bone or a congenital anomaly resulting in a tibial
deficiency) and trans-femoral (any amputation transecting the femur
bone or a congenital anomaly resulting in a femoral deficiency).
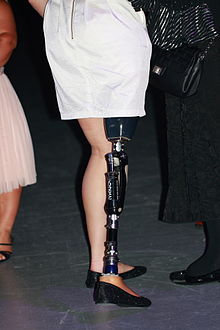
A transfemoral prosthesis is an artificial limb that replaces a
leg missing above the knee. Transfemoral amputees can have a very
difficult time regaining normal movement. In general, a transfemoral
amputee must use approximately 80% more energy to walk than a person
with two whole legs.
This is due to the complexities in movement associated with the knee.
In newer and more improved designs, hydraulics, carbon fiber, mechanical
linkages, motors, computer microprocessors, and innovative combinations
of these technologies are employed to give more control to the user. In
the prosthetics industry a trans-femoral prosthetic leg is often
referred to as an "AK" or above the knee prosthesis.
A transtibial prosthesis is an artificial limb that replaces a
leg missing below the knee. A transtibial amputee is usually able to
regain normal movement more readily than someone with a transfemoral
amputation, due in large part to retaining the knee, which allows for
easier movement. Lower extremity prosthetics describes artificially
replaced limbs located at the hip level or lower. In the prosthetics
industry a trans-tibial prosthetic leg is often referred to as a "BK" or
below the knee prosthesis.
Physical therapists are trained to teach a person to walk with a
leg prosthesis. To do so, the physical therapist may provide verbal
instructions and may also help guide the person using touch, or tactile
cues. This may be done in a clinic or home. There is some research
suggesting that such training in the home may be more successful if the
treatment includes the use of a treadmill.
Using a treadmill, along with the physical therapy treatment, helps the
person to experience many of the challenges of walking with a
prosthesis.
In the United Kingdom, 75% of lower limb amputations are performed due to inadequate
circulation (dysvascularity). This condition is often associated with many other medical conditions (
co-morbidities) including
diabetes and
heart disease that may make it a challenge to recover and use a prosthetic limb to regain mobility and independence.
For people who have inadequate circulation and have lost a lower limb,
there is insufficient evidence due to a lack of research, to inform them
regarding their choice of prosthetic rehabilitation approaches.
Lower extremity prostheses are often categorized by the level of amputation or after the name of a surgeon:
- Transfemoral (Above-knee)
- Transtibial (Below-knee)
- Ankle disarticulation (e.g.: Syme amputation)
- Knee disarticulation
- Hemi-pelvictomy (Hip disarticulation)
- Partial foot amputations (Pirogoff, Talo-Navicular and
Calcaneo-cuboid (Chopart), Tarso-metatarsal (Lisfranc),
Trans-metatarsal, Metatarsal-phalangeal, Ray amputations, toe
amputations).
- Van Nes rotationplasty
Prosthetic raw materials
Prosthetic are made lightweight for better convenience for the amputee. Some of these materials include:
- Plastics:
- Polyethylene
- Polypropylene
- Acrylics
- Polyurethane
- Wood (early prosthetics)
- Rubber (early prosthetics)
- Lightweight metals:
- Composites:
Wheeled prostheses have also been used extensively in the
rehabilitation of injured domestic animals, including dogs, cats, pigs,
rabbits, and turtles.
History
Prosthetic toe from ancient Egypt
"Illustration of mechanical hand", c. 1564.
Iron prosthetic hand believed to have been owned by Götz von Berlichingen (1480–1562)
Artificial iron hand believed to date from 1560–1600
Prosthetics have been mentioned throughout history. The earliest recorded mention is the warrior queen
Vishpala in the
Rigveda. The Egyptians were early pioneers of the idea, as shown by the wooden toe found on a body from the
New Kingdom. Roman bronze
crowns have also been found, but their use could have been more aesthetic than medical.
An early mention of a prosthetic comes from the Greek historian
Herodotus, who tells the story of
Hegesistratus, a Greek
diviner who cut off his own foot to escape his
Spartan captors and replaced it with a wooden one.
Wood and metal hands
Pliny the Elder also recorded the tale of a Roman general,
Marcus Sergius, whose right hand was cut off while campaigning and had an
iron hand made to hold his shield so that he could return to battle. A famous and quite refined historical prosthetic arm was that of
Götz von Berlichingen,
made at the beginning of the 16th century. The first confirmed use of a
prosthetic device, however, is from 950–710 BC. In 2000, research
pathologists discovered a mummy from this period buried in the Egyptian
necropolis near ancient Thebes that possessed an artificial big toe.
This toe, consisting of wood and leather, exhibited evidence of use.
When reproduced by bio-mechanical engineers in 2011, researchers
discovered that this ancient prosthetic enabled its wearer to walk both
barefoot and in Egyptian style sandals. Previously, the earliest
discovered prosthetic was an artificial
leg from Capua.
An artificial limbs factory in 1941
Around the same time,
François de la Noue is also reported to have had an iron hand, as is, in the 17th Century,
René-Robert Cavalier de la Salle.
Henri de Tonti
had a prosthetic hook for a hand. During the Middle Ages, prosthetic
remained quite basic in form. Debilitated knights would be fitted with
prosthetics so they could hold up a shield, grasp a lance or a sword, or
stabilize a mounted warrior. Only the wealthy could afford anything that would assist in daily life.
[citation needed]
One notable prosthesis was that belonging to an Italian man, who
scientists estimate replaced his amputated right hand with a knife. Scientists investigating the skeleton, which was found in a
Longobard cemetery in
Povegliano Veronese, estimated that the man had lived sometime between the 6th and 8th centuries AD.
Materials found near the man's body suggest that the knife prosthesis
was attached with a leather strap, which he repeatedly tightened with
his teeth.
During the Renaissance, prosthetics developed with the use of
iron, steel, copper, and wood. Functional prosthetics began to make an
appearance in the 1500s.
Technology progress before the 20th century
An
Italian surgeon recorded the existence of an amputee who had an arm
that allowed him to remove his hat, open his purse, and sign his name. Improvement in amputation surgery and prosthetic design came at the hands of
Ambroise Paré. Among his inventions was an above-knee device that was a kneeling
peg leg
and foot prosthesis with a fixed position, adjustable harness, and knee
lock control. The functionality of his advancements showed how future
prosthetics could develop.
Other major improvements before the modern era:
- Pieter Verduyn – First non-locking below-knee (BK) prosthesis.
- James Potts –
Prosthesis made of a wooden shank and socket, a steel knee joint and an
articulated foot that was controlled by catgut tendons from the knee to
the ankle. Came to be known as “Anglesey Leg” or “Selpho Leg”.
- Sir James Syme – A new method of ankle amputation that did not involve amputating at the thigh.
- Benjamin Palmer – Improved upon the Selpho leg. Added an anterior spring and concealed tendons to simulate natural-looking movement.
- Dubois Parmlee – Created prosthetic with a suction socket, polycentric knee, and multi-articulated foot.
- Marcel Desoutter & Charles Desoutter – First aluminium prosthesis
- Henry Heather Bigg, and his son Henry Robert Heather Bigg, won the
Queen's command to provide "surgical appliances" to wounded soldiers
after Crimea War. They developed arms that allowed a double arm amputee
to crochet, and a hand that felt natural to others based on ivory, felt,
and leather.
At the end of World War II, the NAS (National Academy of Sciences)
began to advocate better research and development of prosthetics.
Through government funding, a research and development program was
developed within the Army, Navy, Air Force, and the Veterans
Administration.
Lower extremity modern history
Socket
technology for lower extremity limbs saw a revolution during the 1980s
when John Sabolich C.P.O., invented the Contoured Adducted
Trochanteric-Controlled Alignment Method (CATCAM) socket, later to
evolve into the Sabolich Socket. He followed the direction of Ivan Long
and Ossur Christensen as they developed alternatives to the
quadrilateral socket, which in turn followed the open ended plug socket,
created from wood.
The advancement was due to the difference in the socket to patient
contact model. Prior to this, sockets were made in the shape of a square
shape with no specialized containment for muscular tissue. New designs
thus help to lock in the bony anatomy, locking it into place and
distributing the weight evenly over the existing limb as well as the
musculature of the patient. Ischial containment is well known and used
today by many prosthetist to help in patient care. Variations of the
ischial containment socket thus exists and each socket is tailored to
the specific needs of the patient. Others who contributed to socket
development and changes over the years include Tim Staats, Chris Hoyt,
and Frank Gottschalk. Gottschalk disputed the efficacy of the CAT-CAM
socket- insisting the surgical procedure done by the amputation surgeon
was most important to prepare the amputee for good use of a prosthesis
of any type socket design.
The first microprocessor-controlled prosthetic knees became
available in the early 1990s. The Intelligent Prosthesis was the first
commercially available microprocessor controlled prosthetic knee. It was
released by Chas. A. Blatchford and Sons, Ltd., of Great Britain, in
1993 and made walking with the prosthesis feel and look more natural.
An improved version was released in 1995 by the name Intelligent
Prosthesis Plus. Blatchford released another prosthesis, the Adaptive
Prosthesis, in 1998. The Adaptive Prosthesis utilized hydraulic
controls, pneumatic controls, and a microprocessor to provide the
amputee with a gait that was more responsive to changes in walking
speed. Cost analysis reveals that a sophisticated above-knee prosthesis
will be about $1 million in 45 years, given only annual cost of living
adjustments.
Upper extremity modern history
In 2005,
DARPA started the
Revolutionizing Prosthetics program.
Patient procedure
A
prosthesis is a functional replacement for an amputated or congenitally
malformed or missing limb. Prosthetists are responsible for the
prescription, design and management of a prosthetic device.
In most cases, the prosthetist begins by taking a plaster cast of
the patient's affected limb. Lightweight, high-strength thermoplastics
are custom-formed to this model of the patient. Cutting-edge materials
such as carbon fiber, titanium and Kevlar provide strength and
durability while making the new prosthesis lighter. More sophisticated
prostheses are equipped with advanced electronics, providing additional
stability and control.
Current technology and manufacturing
Over the years, there have been advancements in artificial limbs. New plastics and other materials, such as
carbon fiber,
have allowed artificial limbs to be stronger and lighter, limiting the
amount of extra energy necessary to operate the limb. This is especially
important for trans-femoral amputees. Additional materials have allowed
artificial limbs to look much more realistic, which is important to
trans-radial and transhumeral amputees because they are more likely to
have the artificial limb exposed.
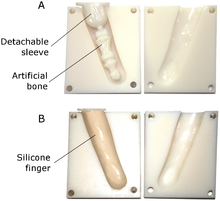
Manufacturing a prosthetic finger
In addition to new materials, the use of electronics has become very
common in artificial limbs. Myoelectric limbs, which control the limbs
by converting muscle movements to electrical signals, have become much
more common than cable operated limbs. Myoelectric signals are picked up
by electrodes, the signal gets integrated and once it exceeds a certain
threshold, the prosthetic limb control signal is triggered which is why
inherently, all myoelectric controls lag. Conversely, cable control is
immediate and physical, and through that offers a certain degree of
direct force feedback that myoelectric control does not. Computers are
also used extensively in the manufacturing of limbs.
Computer Aided Design and Computer Aided Manufacturing are often used to assist in the design and manufacture of artificial limbs.
Most modern artificial limbs are attached to the residual limb (stump) of the amputee by belts and cuffs or by
suction.
The residual limb either directly fits into a socket on the prosthetic,
or—more commonly today—a liner is used that then is fixed to the socket
either by vacuum (suction sockets) or a pin lock. Liners are soft and
by that, they can create a far better suction fit than hard sockets. Silicone liners can be obtained in standard sizes, mostly with a
circular (round) cross section, but for any other residual limb shape,
custom liners can be made. The socket is custom made to fit the residual
limb and to distribute the forces of the artificial limb across the
area of the residual limb (rather than just one small spot), which helps
reduce wear on the residual limb. The custom socket is created by
taking a plaster cast of the residual limb or, more commonly today, of
the liner worn over the residual limb, and then making a mold from the
plaster cast. Newer methods include laser-guided measuring which can be
input directly to a computer allowing for a more sophisticated design.
One problem with the residual limb and socket attachment is that a
bad fit will reduce the area of contact between the residual limb and
socket or liner, and increase pockets between residual limb skin and
socket or liner. Pressure then is higher, which can be painful. Air
pockets can allow sweat to accumulate that can soften the skin.
Ultimately, this is a frequent cause for itchy skin rashes. Over time,
this can lead to breakdown of the skin.
Artificial limbs are typically manufactured using the following steps:
- Measurement of the residual limb
- Measurement of the body to determine the size required for the artificial limb
- Fitting of a silicone liner
- Creation of a model of the liner worn over the residual limb
- Formation of thermoplastic sheet around the model – This is then used to test the fit of the prosthetic
- Formation of permanent socket
- Formation of plastic parts of the artificial limb – Different methods are used, including vacuum forming and injection molding
- Creation of metal parts of the artificial limb using die casting
- Assembly of entire limb
Body-powered arms
Current technology allows body powered arms to weigh around one-half to one-third of what a myoelectric arm does.
Sockets
Current
body-powered arms contain sockets that are built from hard epoxy or
carbon fiber. These sockets or "interfaces" can be made more comfortable
by lining them with a softer, compressible foam material that provides
padding for the bone prominences. A self-suspending or supra-condylar
socket design is useful for those with short to mid-range below elbow
absence. Longer limbs may require the use of a locking roll-on type
inner liner or more complex harnessing to help augment suspension.
Wrists
Wrist
units are either screw-on connectors featuring the UNF 1/2-20 thread
(USA) or quick-release connector, of which there are different models.
Voluntary opening and voluntary closing
Two
types of body-powered systems exist, voluntary opening "pull to open"
and voluntary closing "pull to close". Virtually all "split hook"
prostheses operate with a voluntary opening type system.
More modern "prehensors" called GRIPS utilize voluntary closing
systems. The differences are significant. Users of voluntary opening
systems rely on elastic bands or springs for gripping force, while users
of voluntary closing systems rely on their own body power and energy to
create gripping force.
Voluntary closing users can generate prehension forces equivalent
to the normal hand, upwards to or exceeding one hundred pounds.
Voluntary closing GRIPS require constant tension to grip, like a human
hand, and in that property, they do come closer to matching human hand
performance. Voluntary opening split hook users are limited to forces
their rubber or springs can generate which usually is below 20 pounds.
Feedback
An
additional difference exists in the biofeedback created that allows the
user to "feel" what is being held. Voluntary opening systems once
engaged provide the holding force so that they operate like a passive
vice at the end of the arm. No gripping feedback is provided once the
hook has closed around the object being held. Voluntary closing systems
provide directly
proportional control and biofeedback so that the user can feel how much force that they are applying.
A recent study showed that by stimulating the median and ulnar
nerves, according to the information provided by the artificial sensors
from a hand prosthesis, physiologically appropriate (near-natural)
sensory information could be provided to an amputee. This feedback
enabled the participant to effectively modulate the grasping force of
the prosthesis with no visual or auditory feedback.
Researchers from École Polytechnique Fédérale De Lausanne in
Switzerland and the Scuola Superiore Sant'Anna in Italy, implanted the
electrodes into the amputee's arm in February 2013. The study, published
Wednesday in
Science Translational Medicine, details the first time sensory feedback has been restored allowing an amputee to control an artificial limb in real-time.
With wires linked to nerves in his upper arm, the Danish patient was
able to handle objects and instantly receive a sense of touch through
the special artificial hand that was created by Silvestro Micera and
researchers both in Switzerland and Italy.
Terminal devices
Terminal devices contain a range of hooks, prehensors, hands or other devices.
Hooks
Voluntary opening split hook systems are simple, convenient, light, robust, versatile and relatively affordable.
A hook does not match a normal human hand for appearance or
overall versatility, but its material tolerances can exceed and surpass
the normal human hand for mechanical stress (one can even use a hook to
slice open boxes or as a hammer whereas the same is not possible with a
normal hand), for thermal stability (one can use a hook to grip items
from boiling water, to turn meat on a grill, to hold a match until it
has burned down completely) and for chemical hazards (as a metal hook
withstands acids or lye, and does not react to solvents like a
prosthetic glove or human skin).
Hands
Actor
Owen Wilson gripping the myoelectric prosthetic arm of a United States Marine
Prosthetic hands are available in both voluntary opening and
voluntary closing versions and because of their more complex mechanics
and cosmetic glove covering require a relatively large activation force,
which, depending on the type of harness used, may be uncomfortable.
A recent study by the Delft University of Technology, The Netherlands,
showed that the development of mechanical prosthetic hands has been
neglected during the past decades. The study showed that the pinch force
level of most current mechanical hands is too low for practical use.
The best tested hand was a prosthetic hand developed around 1945. In
2017 however, a research has been started with bionic hands by
Laura Hruby of the
Medical University of Vienna. A few open-hardware 3-d printable bionic hands have also become available. Some companies are also producing robotic hands with integrated forearm, for fitting unto a patient's upper arm.
Commercial providers and materials
Hosmer and
Otto Bock
are major commercial hook providers. Mechanical hands are sold by
Hosmer and Otto Bock as well; the Becker Hand is still manufactured by
the Becker family. Prosthetic hands may be fitted with standard stock or
custom-made cosmetic looking silicone gloves. But regular work gloves
may be worn as well. Other terminal devices include the V2P Prehensor, a
versatile robust gripper that allows customers to modify aspects of it,
Texas Assist Devices (with a whole assortment of tools) and TRS that
offers a range of terminal devices for sports. Cable harnesses can be
built using aircraft steel cables, ball hinges, and self-lubricating
cable sheaths. Some prosthetics have been designed specifically for use
in salt water.
Lower-extremity prosthetics
Lower-extremity prosthetics describes artificially replaced limbs
located at the hip level or lower. Concerning all ages Ephraim et al.
(2003) found a worldwide estimate of all-cause lower-extremity
amputations of 2.0–5.9 per 10,000 inhabitants. For birth prevalence
rates of congenital limb deficiency they found an estimate between
3.5–7.1 cases per 10,000 births.
The two main subcategories of lower extremity prosthetic devices
are trans-tibial (any amputation transecting the tibia bone or a
congenital anomaly resulting in a tibial deficiency), and trans-femoral
(any amputation transecting the femur bone or a congenital anomaly
resulting in a femoral deficiency). In the prosthetic industry, a
trans-tibial prosthetic leg is often referred to as a "BK" or below the
knee prosthesis while the trans-femoral prosthetic leg is often referred
to as an "AK" or above the knee prosthesis.
Other, less prevalent lower extremity cases include the following:
- Hip disarticulations – This usually refers to when an amputee or
congenitally challenged patient has either an amputation or anomaly at
or in close proximity to the hip joint.
- Knee disarticulations – This usually refers to an amputation through the knee disarticulating the femur from the tibia.
- Symes – This is an ankle disarticulation while preserving the heel pad.
Socket
The
socket serves as an interface between the residuum and the prosthesis,
ideally allowing comfortable weight-bearing, movement control and
proprioception. Socket issues, such as discomfort and skin breakdown, are rated among the most important issues faced by lower-limb amputees.
Shank and connectors
This
part creates distance and support between the knee-joint and the foot
(in case of an upper-leg prosthesis) or between the socket and the foot.
The type of connectors that are used between the shank and the
knee/foot determines whether the prosthesis is modular or not. Modular
means that the angle and the displacement of the foot in respect to the
socket can be changed after fitting. In developing countries prosthesis
mostly are non-modular, in order to reduce cost. When considering
children modularity of angle and height is important because of their
average growth of 1.9 cm annually.
Providing contact to the ground, the foot provides shock absorption and stability during stance. Additionally it influences gait biomechanics by its shape and
stiffness. This is because the trajectory of the center of pressure
(COP) and the angle of the ground reaction forces is determined by the
shape and stiffness of the foot and needs to match the subject's build
in order to produce a normal gait pattern.
Andrysek (2010) found 16 different types of feet, with greatly varying
results concerning durability and biomechanics. The main problem found
in current feet is durability, endurance ranging from 16–32 months
These results are for adults and will probably be worse for children
due to higher activity levels and scale effects. Evidence comparing
different types of feet and ankle prosthetic devices is not strong
enough to determine if one mechanism of ankle/foot is superior to
another. When deciding on a device, the cost of the device, a person's
functional need, and the availability of a particular device should be
considered.
Knee joint
In
case of a trans-femoral amputation, there also is a need for a complex
connector providing articulation, allowing flexion during swing-phase
but not during stance.
Microprocessor control
To
mimic the knee's functionality during gait, microprocessor-controlled
knee joints have been developed that control the flexion of the knee.
Some examples are
Otto Bock’s C-leg, introduced in 1997, Ossur's Rheo Knee, released in 2005, the Power Knee by
Ossur, introduced in 2006, the Plié Knee from Freedom Innovations and DAW Industries’ Self Learning Knee (SLK).
The idea was originally developed by Kelly James, a Canadian engineer, at the
University of Alberta.
A microprocessor is used to interpret and analyze signals from
knee-angle sensors and moment sensors. The microprocessor receives
signals from its sensors to determine the type of motion being employed
by the amputee. Most microprocessor controlled knee-joints are powered
by a battery housed inside the prosthesis.
The sensory signals computed by the microprocessor are used to control the resistance generated by
hydraulic cylinders in the knee-joint. Small valves control the amount of
hydraulic fluid
that can pass into and out of the cylinder, thus regulating the
extension and compression of a piston connected to the upper section of
the knee.
The main advantage of a microprocessor-controlled prosthesis is a
closer approximation to an amputee's natural gait. Some allow amputees
to walk near walking speed or run. Variations in speed are also possible
and are taken into account by sensors and communicated to the
microprocessor, which adjusts to these changes accordingly. It also
enables the amputees to walk downstairs with a step-over-step approach,
rather than the one step at a time approach used with mechanical knees. There is some research suggesting that people with
microprocessor-controlled prostheses report greater satisfaction and
improvement in functionality, residual limb health, and safety. People may be able to perform everyday activities at greater speeds, even while multitasking, and reduce their risk of falls.
However, some have some significant drawbacks that impair its
use. They can be susceptible to water damage and thus great care must be
taken to ensure that the prosthesis remains dry.
[citation needed]
Myoelectric
A
myoelectric prosthesis
uses the electrical tension generated every time a muscle contracts, as
information. This tension can be captured from voluntarily contracted
muscles by electrodes applied on the skin to control the movements of
the prosthesis, such as elbow flexion/extension, wrist
supination/pronation (rotation) or opening/closing of the fingers. A
prosthesis of this type utilizes the residual neuromuscular system of
the human body to control the functions of an electric powered
prosthetic hand, wrist, elbow or foot.
This is different from an electric switch prosthesis, which requires
straps and/or cables actuated by body movements to actuate or operate
switches that control the movements of the prosthesis. There is no clear
evidence concluding that myoelectric upper extremity prostheses
function better than body-powered prostheses.
Advantages to using a myoelectric upper extremity prosthesis include
the potential for improvement in cosmetic appeal (this type of
prosthesis may have a more natural look), may be better for light
everyday activities, and may be beneficial for people experiencing
phantom limb pain.
When compared to a body-powered prosthesis, a myoelectric prosthesis
may not be as durable, may have a longer training time, may require more
adjustments, may need more maintenance, and does not provide feedback
to the user.
The USSR was the first to develop a myoelectric arm in 1958, while the first myoelectric arm became commercial in 1964 by the
Central Prosthetic Research Institute of the
USSR, and distributed by the
Hangar Limb Factory of the
UK.
Researchers at the
Rehabilitation Institute of Chicago
announced in September 2013 that they have developed a robotic leg that
translates neural impulses from the user's thigh muscles into movement,
which is the first prosthetic leg to do so. It is currently in testing.
Robotic prostheses
Robots can be used to generate objective measures of patient's
impairment and therapy outcome, assist in diagnosis, customize therapies
based on patient's motor abilities, and assure compliance with
treatment regimens and maintain patient's records. It is shown in many
studies that there is a significant improvement in upper limb motor
function after stroke using robotics for upper limb rehabilitation.
In order for a robotic prosthetic limb to work, it must have several components to integrate it into the body's function:
Biosensors detect signals from the user's nervous or muscular systems. It then relays this information to a
controller
located inside the device, and processes feedback from the limb and
actuator, e.g., position or force, and sends it to the controller.
Examples include surface electrodes that detect electrical activity on
the skin, needle electrodes implanted in muscle, or solid-state
electrode arrays with nerves growing through them. One type of these
biosensors are employed in
myoelectric prostheses.
A device known as the
controller
is connected to the user's nerve and muscular systems and the device
itself. It sends intention commands from the user to the actuators of
the device and interprets feedback from the mechanical and biosensors to
the user. The controller is also responsible for the monitoring and
control of the movements of the device.
An
actuator
mimics the actions of a muscle in producing force and movement.
Examples include a motor that aids or replaces original muscle tissue.
Targeted muscle reinnervation (TMR) is a technique in which
motor nerves, which previously controlled
muscles on an amputated limb, are
surgically rerouted such that they reinnervate a small region of a large, intact muscle, such as the
pectoralis major.
As a result, when a patient thinks about moving the thumb of his
missing hand, a small area of muscle on his chest will contract instead.
By placing sensors over the reinnervated muscle, these contractions can
be made to control the movement of an appropriate part of the robotic
prosthesis.
A variant of this technique is called targeted sensory reinnervation (TSR). This procedure is similar to TMR, except that
sensory nerves are surgically rerouted to
skin
on the chest, rather than motor nerves rerouted to muscle. Recently,
robotic limbs have improved in their ability to take signals from
the human brain and translate those signals into motion in the artificial limb.
DARPA,
the Pentagon's research division, is working to make even more
advancements in this area. Their desire is to create an artificial limb
that ties directly into the
nervous system.
Robotic arms
Advancements
in the processors used in myoelectric arms have allowed developers to
make gains in fine-tuned control of the prosthetic. The
Boston Digital Arm
is a recent artificial limb that has taken advantage of these more
advanced processors. The arm allows movement in five axes and allows the
arm to be programmed for a more customized feel. Recently the
i-Limb hand, invented in Edinburgh, Scotland, by
David Gow
has become the first commercially available hand prosthesis with five
individually powered digits. The hand also possesses a manually
rotatable thumb which is operated passively by the user and allows the
hand to grip in precision, power, and key grip modes.
Another neural prosthetic is
Johns Hopkins University Applied Physics Laboratory Proto 1. Besides the Proto 1, the university also finished the
Proto 2 in 2010.
Early in 2013, Max Ortiz Catalan and Rickard Brånemark of the Chalmers
University of Technology, and Sahlgrenska University Hospital in Sweden,
succeeded in making the first robotic arm which is mind-controlled and
can be permanently attached to the body (using
osseointegration).
An approach that is very useful is called arm rotation which is
common for unilateral amputees which is an amputation that affects only
one side of the body; and also essential for bilateral amputees, a
person who is missing or has had amputated either both arms or legs, to
carry out activities of daily living. This involves inserting a small
permanent magnet into the distal end of the residual bone of subjects
with upper limb amputations. When a subject rotates the residual arm,
the magnet will rotate with the residual bone, causing a change in
magnetic field distribution.
EEG (electroencephalogram) signals, detected using small flat metal
discs attached to the scalp, essentially decoding human brain activity
used for physical movement, is used to control the robotic limbs. This
allows the user to control the part directly.
Robotic legs
Prosthesis design
The
main goal of a robotic prosthesis is to provide active actuation during
gait to improve the biomechanics of gait, including, among other
things, stability, symmetry, or energy expenditure for amputees. There
are several powered prosthetic legs currently on the market, including
fully powered legs, in which actuators directly drive the joints, and
semi-active legs, which use small amounts of energy and a small actuator
to change the mechanical properties of the leg but do not inject net
positive energy into gait. Specific examples include The emPOWER from
BionX, the Proprio Foot from Ossur, and the Elan Foot from Endolite. Various research groups have also experimented with robotic legs over the last decade.
Central issues being researched include designing the behavior of the
device during stance and swing phases, recognizing the current
ambulation task, and various mechanical design problems such as
robustness, weight, battery-life/efficiency, and noise-level. However,
scientists from
Stanford University and
Seoul National University has developed artificial nerves system that will help prosthetic limbs feel. This synthetic nerve system enables prosthetic limbs sense
braille, feel the sense of touch and respond to the environment.
Attachment to the body
Most
prostheses can be attached to the exterior of the body, in a
non-permanent way. Some others however can be attached in a permanent
way. One such example are exoprostheses (see below).
Direct bone attachment and osseointegration
Osseointegration is a method of attaching the artificial limb to the body. This method is also sometimes referred to as
exoprosthesis (attaching an artificial limb to the bone), or endo-exoprosthesis.
The stump and socket method can cause significant pain in the
amputee, which is why the direct bone attachment has been explored
extensively. The method works by inserting a titanium bolt into the bone
at the end of the stump. After several months the
bone attaches itself
to the titanium bolt and an abutment is attached to the titanium bolt.
The abutment extends out of the stump and the (removable) artificial
limb is then attached to the abutment. Some of the benefits of this
method include the following:
- Better muscle control of the prosthetic.
- The ability to wear the prosthetic for an extended period of time; with the stump and socket method this is not possible.
- The ability for transfemoral amputees to drive a car.
The main disadvantage of this method is that amputees with the direct
bone attachment cannot have large impacts on the limb, such as those
experienced during jogging, because of the potential for the bone to
break.
Cosmesis
Cosmetic prosthesis has long been used to disguise injuries and disfigurements. With advances in modern technology,
cosmesis, the creation of lifelike limbs made from
silicone or
PVC
has been made possible. Such prosthetics, including artificial hands,
can now be designed to simulate the appearance of real hands, complete
with freckles, veins, hair, fingerprints and even tattoos.
Custom-made cosmeses are generally more expensive (costing thousands of
U.S. dollars, depending on the level of detail), while standard cosmeses
come premade in a variety of sizes, although they are often not as
realistic as their custom-made counterparts. Another option is the
custom-made silicone cover, which can be made to match a person's skin
tone but not details such as freckles or wrinkles. Cosmeses are attached
to the body in any number of ways, using an adhesive, suction,
form-fitting, stretchable skin, or a skin sleeve.
Cognition
Unlike neuromotor prostheses, neurocognitive prostheses would sense
or modulate neural function in order to physically reconstitute or
augment cognitive processes such as
executive function,
attention,
language, and memory. No neurocognitive prostheses are currently
available but the development of implantable neurocognitive
brain-computer interfaces has been proposed to help treat conditions
such as
stroke,
traumatic brain injury,
cerebral palsy,
autism, and
Alzheimer's disease.
The recent field of
Assistive Technology for Cognition concerns the development of technologies to augment human cognition. Scheduling devices such as
Neuropage
remind users with memory impairments when to perform certain
activities, such as visiting the doctor. Micro-prompting devices such as
PEAT,
AbleLink and
Guide have been used to aid users with memory and executive function problems perform
activities of daily living.
Prosthetic enhancement
Sgt.
Jerrod Fields, a U.S. Army World Class Athlete Program Paralympic
sprinter hopeful, works out at the U.S. Olympic Training Center in Chula
Vista, Calif. A below-the-knee amputee, Fields won a gold medal in the
100 meters with a time of 12.15 seconds at the Endeavor Games in Edmond,
Okla., on June 13, 2009
In addition to the standard artificial limb for everyday use, many amputees or
congenital patients have special limbs and devices to aid in the participation of sports and recreational activities.
Within science fiction, and, more recently, within the
scientific community,
there has been consideration given to using advanced prostheses to
replace healthy body parts with artificial mechanisms and systems to
improve function. The morality and desirability of such technologies are
being debated by
transhumanists, other ethicists, and others in general. Body parts such as legs, arms, hands, feet, and others can be replaced.
The first experiment with a healthy individual appears to have been that by the British scientist
Kevin Warwick. In 2002, an implant was interfaced directly into Warwick's nervous system. The
electrode array, which contained around a hundred
electrodes, was placed in the
median nerve. The signals produced were detailed enough that a
robot arm was able to mimic the actions of Warwick's own arm and provide a form of touch feedback again via the implant.
The
DEKA company of
Dean Kamen developed the "Luke arm", an advanced
nerve-controlled prosthetic. Clinical trials began in 2008,
with FDA approval in 2014 and commercial manufacturing by Universal
Instruments Corporation expected in 2017. The price offered at retail by
Mobius Bionics is expected to be around $100,000.
Oscar Pistorius
In early 2008,
Oscar Pistorius, the "Blade Runner" of South Africa, was briefly ruled ineligible to compete in the
2008 Summer Olympics
because his transtibial prosthesis limbs were said to give him an
unfair advantage over runners who had ankles. One researcher found that
his limbs used twenty-five percent less energy than those of an
able-bodied runner moving at the same speed. This ruling was overturned
on appeal, with the appellate court stating that the overall set of
advantages and disadvantages of Pistorius' limbs had not been
considered.
Pistorius did not qualify for the South African team for the Olympics, but went on to sweep the
2008 Summer Paralympics, and has been ruled eligible to qualify for any future Olympics.
He qualified for the 2011 World Championship in South Korea and reached
the semifinal where he ended last timewise, he was 14th in the first
round, his personal best at 400m would have given him 5th place in the
finals. At the
2012 Summer Olympics in London, Pistorius became the first amputee runner to compete at an Olympic Games. He ran in the
400 metres race semifinals, and the
4 × 400 metres relay race finals. He also competed in 5 events in the
2012 Summer Paralympics in London.
Design considerations
There
are multiple factors to consider when designing a transtibial
prosthesis. Manufacturers must make choices about their priorities
regarding these factors.
Performance
Nonetheless,
there are certain elements of socket and foot mechanics that are
invaluable for the athlete, and these are the focus of today's high-tech
prosthetics companies:
- Fit – athletic/active amputees, or those with bony residua, may
require a carefully detailed socket fit; less-active patients may be
comfortable with a 'total contact' fit and gel liner
- Energy storage and return – storage of energy acquired through
ground contact and utilization of that stored energy for propulsion
- Energy absorption – minimizing the effect of high impact on the musculoskeletal system
- Ground compliance – stability independent of terrain type and angle
- Rotation – ease of changing direction
- Weight – maximizing comfort, balance and speed
- Suspension – how the socket will join and fit to the limb
Other
The buyer is also concerned with numerous other factors:
- Cosmetics
- Cost
- Ease of use
- Size availability
Cost and source freedom
High-cost
In
the USA a typical prosthetic limb costs anywhere between $15,000 and
$90,000, depending on the type of limb desired by the patient. With
medical insurance, a patient will typically pay 10%–50% of the total
cost of a prosthetic limb, while the insurance company will cover the
rest of the cost. The percent that the patient pays varies on the type
of insurance plan, as well as the limb requested by the patient.
In the United Kingdom, much of Europe, Australia and New Zealand the
entire cost of prosthetic limbs is met by state funding or statutory
insurance. For example, in Australia prostheses are fully funded by
state schemes in the case of amputation due to disease, and by workers
compensation or traffic injury insurance in the case of most traumatic
amputations. The
National Disability Insurance Scheme, which is being rolled out nationally between 2017 and 2020 also pays for prostheses.
Transradial (below the elbow amputation) and transtibial prostheses (below the knee amputation) typically cost between US
$6,000
and $8,000, while transfemoral (above the knee amputation) and
transhumeral prosthetics (above the elbow amputation) cost approximately
twice as much with a range of $10,000 to $15,000 and can sometimes
reach costs of $35,000. The cost of an artificial limb often recurs,
while a limb typically needs to be replaced every 3–4 years due to
wear and tear
of everyday use. In addition, if the socket has fit issues, the socket
must be replaced within several months from the onset of pain. If
height is an issue, components such as pylons can be changed.
Not only does the patient need to pay for their multiple
prosthetic limbs, but they also need to pay for physical and
occupational therapy that come along with adapting to living with an
artificial limb. Unlike the reoccurring cost of the prosthetic limbs,
the patient will typically only pay the $2000 to $5000 for therapy
during the first year or two of living as an amputee. Once the patient
is strong and comfortable with their new limb, they will not be required
to go to therapy anymore. Throughout one's life, it is projected that a
typical amputee will go through $1.4 million worth of treatment,
including surgeries, prosthetics, as well as therapies.
Low-cost
Low-cost above-knee prostheses often provide only basic structural
support with limited function. This function is often achieved with
crude, non-articulating, unstable, or manually locking knee joints. A
limited number of organizations, such as the International Committee of
the Red Cross (ICRC), create devices for developing countries. Their
device which is manufactured by CR Equipments is a single-axis, manually
operated locking polymer prosthetic knee joint.
List of knee joint technologies based on the literature review.
| Name of technology (country of origin) |
Brief description |
Highest level of
evidence
|
| ICRC knee (Switzerland) |
Single-axis with manual lock |
Independent field
|
| ATLAS knee (UK) |
Weight-activated friction |
Independent field
|
| POF/OTRC knee (US) |
Single-axis with ext. assist |
Field
|
| DAV/Seattle knee (US) |
Compliant polycentric |
Field
|
| LIMBS International M1 knee (US) |
Four-bar |
Field
|
| JaipurKnee (India) |
Four-bar |
Field
|
| LCKnee (Canada) |
Single-axis with automatic lock |
Field
|
| None provided (Nepal) |
Single-axis |
Field
|
| None provided (New Zealand) |
Roto-molded single-axis |
Field
|
| None provided (India) |
Six-bar with squatting |
Technical development
|
| Friction knee (US) |
Weight-activated friction |
Technical development
|
| Wedgelock knee (Australia) |
Weight-activated friction |
Technical development
|
| SATHI friction knee (India) |
Weight-activated friction |
Limited data available
|
Low-cost above-knee prosthetic limbs: ICRC Knee (left) and LC Knee (right)
A plan for a low-cost artificial leg, designed by Sébastien Dubois,
was featured at the 2007 International Design Exhibition and award show
in Copenhagen, Denmark, where it won the
Index: Award. It would be able to create an energy-return prosthetic leg for US
$8.00, composed primarily of
fiberglass.
Prior to the 1980s, foot prostheses merely restored basic walking
capabilities. These early devices can be characterized by a simple
artificial attachment connecting one's residual limb to the ground.
The introduction of the
Seattle Foot (
Seattle Limb Systems) in 1981 revolutionized the field, bringing the concept of an
Energy Storing Prosthetic Foot
(ESPF) to the fore. Other companies soon followed suit, and before
long, there were multiple models of energy storing prostheses on the
market. Each model utilized some variation of a compressible heel. The
heel is compressed during initial ground contact, storing energy which
is then returned during the latter phase of ground contact to help
propel the body forward.
Since then, the foot prosthetics industry has been dominated by
steady, small improvements in performance, comfort, and marketability.
With
3D printers, it is possible to manufacture a single product without having to have metal
molds, so the costs can be drastically reduced.
Jaipur Foot, an artificial limb from
Jaipur,
India, costs about US$40.
Open-source robotic prothesis
There is currently an
open-design Prosthetics forum known as the "
Open Prosthetics Project".
The group employs collaborators and volunteers to advance Prosthetics
technology while attempting to lower the costs of these necessary
devices.
Open Bionics
is a company that is developing open-source robotic prosthetic hands.
It uses 3D printing to manufacture the devices and low-cost 3D scanners
to fit them, with the aim of lowering the cost of fabricating custom
prosthetics. A review study on a wide range of printed prosthetic hands,
found that although 3D printing technology holds a promise for
individualised prosthesis design, it is not necessarily cheaper when all
costs are included. The same study also found that evidence on the
functionality, durability and user acceptance of 3D printed hand
prostheses is still lacking.
Low-cost prosthetics for children
In the USA an estimate was found of 32,500 children ( < 21 years)
that suffer from major paediatric amputation, with 5,525 new cases each
year, of which 3,315 congenital.
Carr et al. (1998) investigated amputations caused by landmines for
Afghanistan, Bosnia and Herzegovina, Cambodia and Mozambique among
children ( < 14 years), showing estimates of respectively 4.7, 0.19,
1.11 and 0.67 per 1000 children.
Mohan (1986) indicated in India a total of 424,000 amputees (23,500
annually), of which 10.3% had an onset of disability below the age of
14, amounting to a total of about 43,700 limb deficient children in
India alone.
Few low-cost solutions have been created specially for children. Underneath some of them can be found.
Artificial limbs for a juvenile
thalidomide survivor 1961–1965
Pole and crutch
This
hand-held pole with leather support band or platform for the limb is
one of the simplest and cheapest solutions found. It serves well as a
short-term solution, but is prone to rapid contracture formation if the
limb is not stretched daily through a series of range-of motion (RoM)
sets.
Bamboo, PVC or plaster limbs
This
also fairly simple solution comprises a plaster socket with a bamboo or
PVC pipe at the bottom, optionally attached to a prosthetic foot. This
solution prevents contractures because the knee is moved through its
full RoM. The David Werner Collection, an online database for the
assistance of disabled village children, displays manuals of production
of these solutions.
Adjustable bicycle limb
This
solution is built using a bicycle seat post up side down as foot,
generating flexibility and (length) adjustability. It is a very cheap
solution, using locally available materials.
Sathi Limb
It
is an endoskeletal modular lower limb from India, which uses
thermoplastic parts. Its main advantages are the small weight and
adaptability.
Monolimb
Monolimbs
are non-modular prostheses and thus require more experienced
prosthetist for correct fitting, because alignment can barely be changed
after production. However, their durability on average is better than
low-cost modular solutions.
Cultural and social theory perspectives
A number of theorists have explored the meaning and implications of prosthetic extension of the body.
Elizabeth Grosz
writes, "Creatures use tools, ornaments, and appliances to augment
their bodily capacities. Are their bodies lacking something, which they
need to replace with artificial or substitute organs?...Or conversely,
should prostheses be understood, in terms of aesthetic reorganization
and proliferation, as the consequence of an inventiveness that functions
beyond and perhaps in defiance of pragmatic need?"
Elaine Scarry
argues that every artifact recreates and extends the body. Chairs
supplement the skeleton, tools append the hands, clothing augments the
skin.
In Scarry's thinking, "furniture and houses are neither more nor less
interior to the human body than the food it absorbs, nor are they
fundamentally different from such sophisticated prosthetics as
artificial lungs, eyes and kidneys. The consumption of manufactured
things turns the body inside out, opening it up
to and
as the culture of objects."
Mark Wigley,
a professor of architecture, continues this line of thinking about how
architecture supplements our natural capabilities, and argues that "a
blurring of identity is produced by all prostheses." Some of this work relies on
Freud's earlier characterization of man's relation to objects as one of extension.