| Mental disorder | |
|---|---|
| Synonyms | Psychiatric disorder, psychological disorder, mental illness, mental disease, mental breakdown, nervous breakdown |
 | |
| Specialty | Psychiatry, clinical psychology |
| Symptoms | Agitation, anxiety, depression, mania, paranoia, psychosis |
| Complications | Cognitive impairment, social problems, suicide |
| Types | Anxiety disorders, eating disorders, mood disorders, neurodevelopmental disorders, personality disorders, psychotic disorders, substance use disorders |
| Causes | Genetic and environmental factors |
| Treatment | Psychotherapy, medications |
| Medication | Antidepressants, antipsychotics, anxiolytics, mood stabilizers, stimulants |
| Frequency | 18% per year (United States) |
A mental disorder, also called a mental illness or psychiatric disorder, is a behavioral or mental pattern that causes significant distress or impairment of personal functioning. Such features may be persistent, relapsing and remitting, or occur as a single episode. Many disorders have been described, with signs and symptoms that vary widely between specific disorders. Such disorders may be diagnosed by a mental health professional.
The causes of mental disorders are often unclear. Theories may incorporate findings from a range of fields. Mental disorders are usually defined by a combination of how a person behaves, feels, perceives, or thinks. This may be associated with particular regions or functions of the brain, often in a social context. A mental disorder is one aspect of mental health. Cultural and religious beliefs, as well as social norms, should be taken into account when making a diagnosis.
Services are based in psychiatric hospitals or in the community, and assessments are carried out by mental health professionals such as psychiatrists, psychologists, and clinical social workers, using various methods such as psychometric tests but often relying on observation and questioning. Treatments are provided by various mental health professionals. Psychotherapy and psychiatric medication are two major treatment options. Other treatments include social interventions, peer support, and self-help. In a minority of cases there might be involuntary detention or treatment. Prevention programs have been shown to reduce depression.
Common mental disorders include depression, which affects about 400 million, dementia which affects about 35 million, and schizophrenia, which affects about 21 million people globally. Stigma and discrimination can add to the suffering and disability associated with mental disorders, leading to various social movements attempting to increase understanding and challenge social exclusion.
Definition
The definition and classification of mental disorders are key issues for researchers as well as service providers and those who may be diagnosed. For a mental state to classify as a disorder, it generally needs to cause dysfunction. Most international clinical documents use the term mental "disorder", while "illness" is also common. It has been noted that using the term "mental" (i.e., of the mind) is not necessarily meant to imply separateness from brain or body.According to DSM-IV, a mental disorder is a psychological syndrome or pattern which is associated with distress (e.g. via a painful symptom), disability (impairment in one or more important areas of functioning), increased risk of death, or causes a significant loss of autonomy; however it excludes normal responses such as grief from loss of a loved one, and also excludes deviant behavior for political, religious, or societal reasons not arising from a dysfunction in the individual.
DSM-IV precedes the definition with caveats, stating that, as in the case with many medical terms, mental disorder "lacks a consistent operational definition that covers all situations", noting that different levels of abstraction can be used for medical definitions, including pathology, symptomology, deviance from a normal range, or etiology, and that the same is true for mental disorders, so that sometimes one type of definition is appropriate, and sometimes another, depending on the situation.
In 2013, the American Psychiatric Association (APA) redefined mental disorders in the DSM-5 as "a syndrome characterized by clinically significant disturbance in an individual's cognition, emotion regulation, or behavior that reflects a dysfunction in the psychological, biological, or developmental processes underlying mental functioning.” The final draft of ICD-11 contains a very similar definition.
The terms "mental breakdown" or "nervous breakdown" may be used by the general population to mean a mental disorder. The terms "nervous breakdown" and "mental breakdown" have not been formally defined through a medical diagnostic system such as the DSM-5 or ICD-10, and are nearly absent from scientific literature regarding mental illness. Although "nervous breakdown" is not rigorously defined, surveys of laypersons suggest that the term refers to a specific acute time-limited reactive disorder, involving symptoms such as anxiety or depression, usually precipitated by external stressors. Many health experts today refer to a nervous breakdown as a "modern mental health crisis".
Concept of nervous illness
Additionally to the concept of mental disorder, some people have argued for a return to the old-fashioned concept of nervous illness In How Everyone Became Depressed: The Rise and Fall of the Nervous Breakdown (2013), Edward Shorter, a professor of psychiatry and the history of medicine, says:About half of them are depressed. Or at least that is the diagnosis that they got when they were put on antidepressants. ... They go to work but they are unhappy and uncomfortable; they are somewhat anxious; they are tired; they have various physical pains—and they tend to obsess about the whole business. There is a term for what they have, and it is a good old-fashioned term that has gone out of use. They have nerves or a nervous illness. It is an illness not just of mind or brain, but a disorder of the entire body. ... We have a package here of five symptoms—mild depression, some anxiety, fatigue, somatic pains, and obsessive thinking. ... We have had nervous illness for centuries. When you are too nervous to function ... it is a nervous breakdown. But that term has vanished from medicine, although not from the way we speak. ... The nervous patients of yesteryear are the depressives of today. That is the bad news. ... There is a deeper illness that drives depression and the symptoms of mood. We can call this deeper illness something else, or invent a neologism, but we need to get the discussion off depression and onto this deeper disorder in the brain and body. That is the point.
— Edward Shorter, Faculty of Medicine, University of Toronto.
In eliminating the nervous breakdown, psychiatry has come close to having its own nervous breakdown.
— David Healy, MD, FRCPsych, Professor of Psychiatry, University of Cardiff, Wales.
"Nerves stand at the core of common mental illness, no matter how much we try to forget them.
— Peter J. Tyrer, FMedSci, Professor of Community Psychiatry, Imperial College, London
"Nervous breakdown" is a pseudo-medical term to describe a wealth of stress-related feelings and they are often made worse by the belief that there is a real phenomenon called "nervous breakdown".
— Richard E. Vatz, co-author of explication of views of Thomas Szasz in /Thomas Szasz : "Primary Values and Major Contentions"
Classifications
There are currently two widely established systems that classify mental disorders:- ICD-10 Chapter V: Mental and behavioural disorders, since 1949 part of the International Classification of Diseases produced by the WHO,
- the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) produced by the American Psychiatric Association (APA) since 1952.
Unlike the DSM and ICD, some approaches are not based on identifying distinct categories of disorder using dichotomous symptom profiles intended to separate the abnormal from the normal. There is significant scientific debate about the relative merits of categorical versus such non-categorical (or hybrid) schemes, also known as continuum or dimensional models. A spectrum approach may incorporate elements of both.
In the scientific and academic literature on the definition or classification of mental disorder, one extreme argues that it is entirely a matter of value judgements (including of what is normal) while another proposes that it is or could be entirely objective and scientific (including by reference to statistical norms). Common hybrid views argue that the concept of mental disorder is objective even if only a "fuzzy prototype" that can never be precisely defined, or conversely that the concept always involves a mixture of scientific facts and subjective value judgments. Although the diagnostic categories are referred to as 'disorders', they are presented as medical diseases, but are not validated in the same way as most medical diagnoses. Some neurologists argue that classification will only be reliable and valid when based on neurobiological features rather than clinical interview, while others suggest that the differing ideological and practical perspectives need to be better integrated.
The DSM and ICD approach remains under attack both because of the implied causality model and because some researchers believe it better to aim at underlying brain differences which can precede symptoms by many years.
Dimensional models
The high degree of comorbidity between disorders in categorical models such as the DSM and ICD have led some to propose dimensional models. Studying comorbidity between disorders have demonstrated two latent (unobserved) factors or dimensions in the structure of mental disorders that are thought to possibly reflect etiological processes. These two dimensions reflect a distinction between internalizing disorders, such as mood or anxiety symptoms, and externalizing disorders such as behavioral or substance abuse symptoms. A single general factor of psychopathology, similar to the g factor for intelligence, has been empirically supported. The p factor model supports the internalizing-externalizing distinction, but also supports the formation of a third dimension of thought disorders such as schizophrenia. Biological evidence also supports the validity of the internalizing-externalizing structure of mental disorders, with twin and adoption studies supporting heritable factors for externalizing and internalizing disorders.Disorders
There are many different categories of mental disorder, and many different facets of human behavior and personality that can become disordered.Anxiety or fear that interferes with normal functioning may be classified as an anxiety disorder. Commonly recognized categories include specific phobias, generalized anxiety disorder, social anxiety disorder, panic disorder, agoraphobia, obsessive-compulsive disorder and post-traumatic stress disorder.
Other affective (emotion/mood) processes can also become disordered. Mood disorder involving unusually intense and sustained sadness, melancholia, or despair is known as major depression (also known as unipolar or clinical depression). Milder but still prolonged depression can be diagnosed as dysthymia. Bipolar disorder (also known as manic depression) involves abnormally "high" or pressured mood states, known as mania or hypomania, alternating with normal or depressed moods. The extent to which unipolar and bipolar mood phenomena represent distinct categories of disorder, or mix and merge along a dimension or spectrum of mood, is subject to some scientific debate.
Patterns of belief, language use and perception of reality can become disordered (e.g., delusions, thought disorder, hallucinations). Psychotic disorders in this domain include schizophrenia, and delusional disorder. Schizoaffective disorder is a category used for individuals showing aspects of both schizophrenia and affective disorders. Schizotypy is a category used for individuals showing some of the characteristics associated with schizophrenia but without meeting cutoff criteria.
Personality—the fundamental characteristics of a person that influence thoughts and behaviors across situations and time—may be considered disordered if judged to be abnormally rigid and maladaptive. Although treated separately by some, the commonly used categorical schemes include them as mental disorders, albeit on a separate "axis II" in the case of the DSM-IV. A number of different personality disorders are listed, including those sometimes classed as "eccentric", such as paranoid, schizoid and schizotypal personality disorders; types that have described as "dramatic" or "emotional", such as antisocial, borderline, histrionic or narcissistic personality disorders; and those sometimes classed as fear-related, such as anxious-avoidant, dependent, or obsessive-compulsive personality disorders. The personality disorders, in general, are defined as emerging in childhood, or at least by adolescence or early adulthood. The ICD also has a category for enduring personality change after a catastrophic experience or psychiatric illness. If an inability to sufficiently adjust to life circumstances begins within three months of a particular event or situation, and ends within six months after the stressor stops or is eliminated, it may instead be classed as an adjustment disorder. There is an emerging consensus that so-called "personality disorders", like personality traits in general, actually incorporate a mixture of acute dysfunctional behaviors that may resolve in short periods, and maladaptive temperamental traits that are more enduring. Furthermore, there are also non-categorical schemes that rate all individuals via a profile of different dimensions of personality without a symptom-based cutoff from normal personality variation, for example through schemes based on dimensional models.
Eating disorders involve disproportionate concern in matters of food and weight. Categories of disorder in this area include anorexia nervosa, bulimia nervosa, exercise bulimia or binge eating disorder.
Sleep disorders such as insomnia involve disruption to normal sleep patterns, or a feeling of tiredness despite sleep appearing normal.
Sexual disorders and gender dysphoria may be diagnosed, including dyspareunia and ego-dystonic homosexuality. Various kinds of paraphilia are considered mental disorders (sexual arousal to objects, situations, or individuals that are considered abnormal or harmful to the person or others).
People who are abnormally unable to resist certain urges or impulses that could be harmful to themselves or others, may be classed as having an impulse control disorder, and disorders such as kleptomania (stealing) or pyromania (fire-setting). Various behavioral addictions, such as gambling addiction, may be classed as a disorder. Obsessive-compulsive disorder can sometimes involve an inability to resist certain acts but is classed separately as being primarily an anxiety disorder.
The use of drugs (legal or illegal, including alcohol), when it persists despite significant problems related to its use, may be defined as a mental disorder. The DSM incorporates such conditions under the umbrella category of substance use disorders, which includes substance dependence and substance abuse. The DSM does not currently use the common term drug addiction, and the ICD simply refers to "harmful use". Disordered substance use may be due to a pattern of compulsive and repetitive use of the drug that results in tolerance to its effects and withdrawal symptoms when use is reduced or stopped.
People who suffer severe disturbances of their self-identity, memory and general awareness of themselves and their surroundings may be classed as having a dissociative identity disorder, such as depersonalization disorder or Dissociative Identity Disorder itself (which has also been called multiple personality disorder, or "split personality"). Other memory or cognitive disorders include amnesia or various kinds of old age dementia.
A range of developmental disorders that initially occur in childhood may be diagnosed, for example autism spectrum disorders, oppositional defiant disorder and conduct disorder, and attention deficit hyperactivity disorder (ADHD), which may continue into adulthood.
Conduct disorder, if continuing into adulthood, may be diagnosed as antisocial personality disorder (dissocial personality disorder in the ICD). Popularist labels such as psychopath (or sociopath) do not appear in the DSM or ICD but are linked by some to these diagnoses.
Somatoform disorders may be diagnosed when there are problems that appear to originate in the body that are thought to be manifestations of a mental disorder. This includes somatization disorder and conversion disorder. There are also disorders of how a person perceives their body, such as body dysmorphic disorder. Neurasthenia is an old diagnosis involving somatic complaints as well as fatigue and low spirits/depression, which is officially recognized by the ICD-10 but no longer by the DSM-IV.
Factitious disorders, such as Munchausen syndrome, are diagnosed where symptoms are thought to be experienced (deliberately produced) and/or reported (feigned) for personal gain.
There are attempts to introduce a category of relational disorder, where the diagnosis is of a relationship rather than on any one individual in that relationship. The relationship may be between children and their parents, between couples, or others. There already exists, under the category of psychosis, a diagnosis of shared psychotic disorder where two or more individuals share a particular delusion because of their close relationship with each other.
There are a number of uncommon psychiatric syndromes, which are often named after the person who first described them, such as Capgras syndrome, De Clerambault syndrome, Othello syndrome, Ganser syndrome, Cotard delusion, and Ekbom syndrome, and additional disorders such as the Couvade syndrome and Geschwind syndrome.
Various new types of mental disorder diagnosis are occasionally proposed. Among those controversially considered by the official committees of the diagnostic manuals include self-defeating personality disorder, sadistic personality disorder, passive-aggressive personality disorder and premenstrual dysphoric disorder.
Two recent unique unofficial proposals are solastalgia by Glenn Albrecht and hubris syndrome by David Owen. The application of the concept of mental illness to the phenomena described by these authors has in turn been critiqued by Seamus Mac Suibhne.
Signs and symptoms
Course
The likely course and outcome of mental disorders varies and is dependent on numerous factors related to the disorder itself, the individual as a whole, and the social environment. Some disorders are transient, while others may be more chronic in nature.Even those disorders often considered the most serious and intractable have varied courses i.e. schizophrenia, psychotic disorders, and personality disorders. Long-term international studies of schizophrenia have found that over a half of individuals recover in terms of symptoms, and around a fifth to a third in terms of symptoms and functioning, with many requiring no medication. While some have serious difficulties and support needs for many years, "late" recovery is still plausible. The World Health Organization concluded that the long-term studies' findings converged with others in "relieving patients, carers and clinicians of the chronicity paradigm which dominated thinking throughout much of the 20th century."
Around half of people initially diagnosed with bipolar disorder achieve syndromal recovery (no longer meeting criteria for the diagnosis) within six weeks, and nearly all achieve it within two years, with nearly half regaining their prior occupational and residential status in that period. Less than half go on to experience a new episode of mania or major depression within the next two years. Functioning has been found to vary, being poor during periods of major depression or mania but otherwise fair to good, and possibly superior during periods of hypomania in Bipolar II.
Disability
Some disorders may be very limited in their functional effects, while others may involve substantial disability and support needs. The degree of ability or disability may vary over time and across different life domains. Furthermore, continued disability has been linked to institutionalization, discrimination and social exclusion as well as to the inherent effects of disorders. Alternatively, functioning may be affected by the stress of having to hide a condition in work or school etc., by adverse effects of medications or other substances, or by mismatches between illness-related variations and demands for regularity.It is also the case that, while often being characterized in purely negative terms, some mental traits or states labeled as disorders can also involve above-average creativity, non-conformity, goal-striving, meticulousness, or empathy. In addition, the public perception of the level of disability associated with mental disorders can change.
Nevertheless, internationally, people report equal or greater disability from commonly occurring mental conditions than from commonly occurring physical conditions, particularly in their social roles and personal relationships. The proportion with access to professional help for mental disorders is far lower, however, even among those assessed as having a severely disabling condition. Disability in this context may or may not involve such things as:
- Basic activities of daily living. Including looking after the self (health care, grooming, dressing, shopping, cooking etc.) or looking after accommodation (chores, DIY tasks, etc.)
- Interpersonal relationships. Including communication skills, ability to form relationships and sustain them, ability to leave the home or mix in crowds or particular settings
- Occupational functioning. Ability to acquire a employment and hold it, cognitive and social skills required for the job, dealing with workplace culture, or studying as a student.
The first ever systematic description of global disability arising in youth, published in 2011, found that among 10- to 24-year-olds nearly half of all disability (current and as estimated to continue) was due to mental and neurological conditions, including substance use disorders and conditions involving self-harm. Second to this were accidental injuries (mainly traffic collisions) accounting for 12 percent of disability, followed by communicable diseases at 10 percent. The disorders associated with most disability in high income countries were unipolar major depression (20%) and alcohol use disorder (11%). In the eastern Mediterranean region it was unipolar major depression (12%) and schizophrenia (7%), and in Africa it was unipolar major depression (7%) and bipolar disorder (5%).
Suicide, which is often attributed to some underlying mental disorder, is a leading cause of death among teenagers and adults under 35. There are an estimated 10 to 20 million non-fatal attempted suicides every year worldwide.
Risk factors
The predominant view as of 2018 is that biological, psychological, and environmental factors all contribute to the development or progression of mental disorders.Drugs
Mental disorders are associated with drug use including: cannabis, alcohol, and caffeine, use of which appears to promote anxiety. For psychosis and schizophrenia, usage of a number of drugs has been associated with development of the disorder, including cannabis, cocaine, and amphetamines. There has been debate regarding the relationship between usage of cannabis and bipolar disorder. Cannabis has also been associated with depression.Personality traits
Risk factors for mental illness include a propensity for high neuroticism or "emotional instability". In anxiety, risk factors may include temperament and attitudes (e.g. pessimism).Genetics
Twin studies have revealed a very high heritability for many mental disorders (especially autism and schizophrenia). But although researchers have been looking for decades for clear linkages between genetics and mental disorders, that work has yielded no genetic biomarkers yet that might lead to better diagnosis and better treatments.A number of disorders are linked to a family history including depression, narcissistic personality disorder and anxiety.
Environmental
In schizophrenia and psychosis, risk factors include migration and discrimination, childhood trauma, bereavement or separation in families, abuse of drugs, and urbanicity.In anxiety, risk factors may include parenting factors including parental rejection, lack of parental warmth, high hostility, harsh discipline, high maternal negative affect, anxious childrearing, modelling of dysfunctional and drug-abusing behavior, and child abuse (emotional, physical and sexual).
For bipolar disorder, stress (such as childhood adversity) is not a specific cause, but does place genetically and biologically vulnerable individuals at risk for a more severe course of illness.
Social influences have also been found to be important, including abuse, neglect, bullying, social stress, traumatic events, and other negative or overwhelming life experiences. Aspects of the wider community have also been implicated, including employment problems, socioeconomic inequality, lack of social cohesion, problems linked to migration, and features of particular societies and cultures. The specific risks and pathways to particular disorders are less clear, however.
Models
Mental disorders can arise from multiple sources, and in many cases there is no single accepted or consistent cause currently established. An eclectic or pluralistic mix of models may be used to explain particular disorders. The primary paradigm of contemporary mainstream Western psychiatry is said to be the biopsychosocial model which incorporates biological, psychological and social factors, although this may not always be applied in practice.Biological psychiatry follows a biomedical model where many mental disorders are conceptualized as disorders of brain circuits likely caused by developmental processes shaped by a complex interplay of genetics and experience. A common assumption is that disorders may have resulted from genetic and developmental vulnerabilities, exposed by stress in life (for example in a diathesis–stress model), although there are various views on what causes differences between individuals. Some types of mental disorders may be viewed as primarily neurodevelopmental disorders.
Evolutionary psychology may be used as an overall explanatory theory, while attachment theory is another kind of evolutionary-psychological approach sometimes applied in the context of mental disorders. Psychoanalytic theories have continued to evolve alongside and cognitive-behavioral and systemic-family approaches. A distinction is sometimes made between a "medical model" or a "social model" of disorder and disability.
Diagnosis
Psychiatrists seek to provide a medical diagnosis of individuals by an assessment of symptoms, signs and impairment associated with particular types of mental disorder. Other mental health professionals, such as clinical psychologists, may or may not apply the same diagnostic categories to their clinical formulation of a client's difficulties and circumstances. The majority of mental health problems are, at least initially, assessed and treated by family physicians (in the UK general practitioners) during consultations, who may refer a patient on for more specialist diagnosis in acute or chronic cases.Routine diagnostic practice in mental health services typically involves an interview known as a mental status examination, where evaluations are made of appearance and behavior, self-reported symptoms, mental health history, and current life circumstances. The views of other professionals, relatives or other third parties may be taken into account. A physical examination to check for ill health or the effects of medications or other drugs may be conducted. Psychological testing is sometimes used via paper-and-pen or computerized questionnaires, which may include algorithms based on ticking off standardized diagnostic criteria, and in rare specialist cases neuroimaging tests may be requested, but such methods are more commonly found in research studies than routine clinical practice.
Time and budgetary constraints often limit practicing psychiatrists from conducting more thorough diagnostic evaluations. It has been found that most clinicians evaluate patients using an unstructured, open-ended approach, with limited training in evidence-based assessment methods, and that inaccurate diagnosis may be common in routine practice. In addition, comorbidity is very common in psychiatric diagnosis, where the same person meets the criteria for more than one disorder. On the other hand, a person may have several different difficulties only some of which meet the criteria for being diagnosed. There may be specific problems with accurate diagnosis in developing countries.
More structured approaches are being increasingly used to measure levels of mental illness.
HoNOS is the most widely used measure in English mental health services, being used by at least 61 trusts. In HoNOS a score of 0–4 is given for each of 12 factors, based on functional living capacity. Research has been supportive of HoNOS, although some questions have been asked about whether it provides adequate coverage of the range and complexity of mental illness problems, and whether the fact that often only 3 of the 12 scales vary over time gives enough subtlety to accurately measure outcomes of treatment.
Criticism
Since the 1980s, Paula Caplan has been concerned about the subjectivity of psychiatric diagnosis, and people being arbitrarily “slapped with a psychiatric label.” Caplan says because psychiatric diagnosis is unregulated, doctors are not required to spend much time interviewing patients or to seek a second opinion. The Diagnostic and Statistical Manual of Mental Disorders can lead a psychiatrist to focus on narrow checklists of symptoms, with little consideration of what is actually causing the patient’s problems. So, according to Caplan, getting a psychiatric diagnosis and label often stands in the way of recovery.In 2013, psychiatrist Allen Frances wrote a paper entitled "The New Crisis of Confidence in Psychiatric Diagnosis", which said that "psychiatric diagnosis… still relies exclusively on fallible subjective judgments rather than objective biological tests." Frances was also concerned about "unpredictable over diagnosis." For many years, marginalized psychiatrists (such as Peter Breggin, Thomas Szasz) and outside critics (such as Stuart A. Kirk) have "been accusing psychiatry of engaging in the systematic medicalization of normality." More recently these concerns have come from insiders who have worked for and promoted the American Psychiatric Association (e.g., Robert Spitzer, Allen Frances). A 2002 editorial in the British Medical Journal warned of inappropriate medicalization leading to disease mongering, where the boundaries of the definition of illnesses are expanded to include personal problems as medical problems or risks of diseases are emphasized to broaden the market for medications.
Prevention
The 2004 WHO report "Prevention of Mental Disorders" stated that "Prevention of these disorders is obviously one of the most effective ways to reduce the [disease] burden." The 2011 European Psychiatric Association (EPA) guidance on prevention of mental disorders states "There is considerable evidence that various psychiatric conditions can be prevented through the implementation of effective evidence-based interventions." A 2011 UK Department of Health report on the economic case for mental health promotion and mental illness prevention found that "many interventions are outstandingly good value for money, low in cost and often become self-financing over time, saving public expenditure". In 2016, the National Institute of Mental Health re-affirmed prevention as a research priority area.Parenting may affect the child's mental health, and evidence suggests that helping parents to be more effective with their children can address mental health needs.
Universal prevention (aimed at a population that has no increased risk for developing a mental disorder, such as school programs or mass media campaigns) need very high numbers of people to show effect (sometimes known as the "power" problem). Approaches to overcome this are (1) focus on high-incidence groups (e.g. by targeting groups with high risk factors), (2) use multiple interventions to achieve greater, and thus more statistically valid, effects, (3) use cumulative meta-analyses of many trials, and (4) run very large trials.
Management
"Haus
Tornow am See" (former manor house), Germany from 1912 is today
separated into a special education school and a hotel with integrated
work/job- and rehabilitation-training for people with mental disorders
Treatment and support for mental disorders is provided in psychiatric hospitals, clinics or any of a diverse range of community mental health services. A number of professions have developed that specialize in the treatment of mental disorders. This includes the medical specialty of psychiatry (including psychiatric nursing), the field of psychology known as clinical psychology, and the practical application of sociology known as social work. There is also a wide range of psychotherapists (including family therapy), counselors, and public health professionals. In addition, there are peer support roles where personal experience of similar issues is the primary source of expertise.
The different clinical and scientific perspectives draw on diverse
fields of research and theory, and different disciplines may favor
differing models, explanations and goals.
In some countries services are increasingly based on a recovery approach,
intended to support each individual's personal journey to gain the kind
of life they want, although there may also be 'therapeutic pessimism'
in some areas.
There are a range of different types of treatment and what is
most suitable depends on the disorder and on the individual. Many things
have been found to help at least some people, and a placebo
effect may play a role in any intervention or medication. In a minority
of cases, individuals may be treated against their will, which can
cause particular difficulties depending on how it is carried out and
perceived.
Compulsory treatment while in the community versus non-compulsory
treatment does not appear to make much of a difference except by maybe
decreasing victimization.
Psychotherapy
A major option for many mental disorders is psychotherapy. There are several main types. Cognitive behavioral therapy (CBT) is widely used and is based on modifying the patterns of thought and behavior associated with a particular disorder. Psychoanalysis, addressing underlying psychic conflicts and defenses, has been a dominant school of psychotherapy and is still in use. Systemic therapy or family therapy is sometimes used, addressing a network of significant others as well as an individual.
Some psychotherapies are based on a humanistic
approach. There are a number of specific therapies used for particular
disorders, which may be offshoots or hybrids of the above types. Mental
health professionals often employ an eclectic or integrative approach. Much may depend on the therapeutic relationship, and there may be problems with trust, confidentiality and engagement.
Medication
A major option for many mental disorders is psychiatric medication and there are several main groups. Antidepressants are used for the treatment of clinical depression, as well as often for anxiety and a range of other disorders. Anxiolytics (including sedatives) are used for anxiety disorders and related problems such as insomnia. Mood stabilizers are used primarily in bipolar disorder. Antipsychotics are used for psychotic disorders, notably for positive symptoms in schizophrenia, and also increasingly for a range of other disorders. Stimulants are commonly used, notably for ADHD.
Despite the different conventional names of the drug groups,
there may be considerable overlap in the disorders for which they are
actually indicated, and there may also be off-label use of medications. There can be problems with adverse effects of medication and adherence to them, and there is also criticism of pharmaceutical marketing and professional conflicts of interest.
Other
Electroconvulsive therapy (ECT) is sometimes used in severe cases when other interventions for severe intractable depression have failed. Psychosurgery is considered experimental but is advocated by some neurologists in certain rare cases.
Counseling (professional) and co-counseling (between peers) may be used. Psychoeducation
programs may provide people with the information to understand and
manage their problems. Creative therapies are sometimes used, including music therapy, art therapy or drama therapy. Lifestyle adjustments and supportive measures are often used, including peer support, self-help groups for mental health and supported housing or supported employment (including social firms). Some advocate dietary supplements.
Reasonable accommodations
(adjustments and supports) might be put in place to help an individual
cope and succeed in environments despite potential disability related to
mental health problems. This could include an emotional support animal or specifically trained psychiatric service dog.
Epidemiology
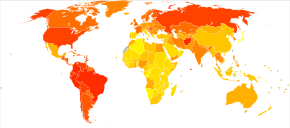
Deaths from mental and behavioral disorders per million persons in 2012
0–6
7–9
10–15
16–24
25–31
32–39
40–53
54–70
71–99
100–356
Disability-adjusted life year for neuropsychiatric conditions per 100,000 inhabitants in 2004.
<2200 span="">
2200–2400
2400–2600
2600–2800
2800–3000
3000–3200
3200–3400
3400–3600
3600–3800
3800–4000
4000–4200
>4200
Mental disorders are common. Worldwide, more than one in three people
in most countries report sufficient criteria for at least one at some
point in their life. In the United States, 46% qualify for a mental illness at some point.
An ongoing survey indicates that anxiety disorders are the most common
in all but one country, followed by mood disorders in all but two
countries, while substance disorders and impulse-control disorders were
consistently less prevalent. Rates varied by region.
A review of anxiety disorder surveys in different countries found
average lifetime prevalence estimates of 16.6%, with women having
higher rates on average.
A review of mood disorder surveys in different countries found lifetime
rates of 6.7% for major depressive disorder (higher in some studies,
and in women) and 0.8% for Bipolar I disorder.
In the United States the frequency of disorder is: anxiety
disorder (28.8%), mood disorder (20.8%), impulse-control disorder
(24.8%) or substance use disorder (14.6%).
A 2004 cross-Europe study found that approximately one in four
people reported meeting criteria at some point in their life for at
least one of the DSM-IV disorders assessed, which included mood
disorders (13.9%), anxiety disorders (13.6%) or alcohol disorder (5.2%).
Approximately one in ten met criteria within a 12-month period. Women
and younger people of either gender showed more cases of disorder.
A 2005 review of surveys in 16 European countries found that 27% of
adult Europeans are affected by at least one mental disorder in a
12-month period.
An international review of studies on the prevalence of
schizophrenia found an average (median) figure of 0.4% for lifetime
prevalence; it was consistently lower in poorer countries.
Studies of the prevalence of personality disorders (PDs) have
been fewer and smaller-scale, but one broad Norwegian survey found a
five-year prevalence of almost 1 in 7 (13.4%). Rates for specific
disorders ranged from 0.8% to 2.8%, differing across countries, and by
gender, educational level and other factors. A US survey that incidentally screened for personality disorder found a rate of 14.79%.
Approximately 7% of a preschool pediatric sample were given a
psychiatric diagnosis in one clinical study, and approximately 10% of 1-
and 2-year-olds receiving developmental screening have been assessed as
having significant emotional/behavioral problems based on parent and
pediatrician reports.
While rates of psychological disorders are often the same for men
and women, women tend to have a higher rate of depression. Each year 73
million women are affected by major depression, and suicide is ranked
7th as the cause of death for women between the ages of 20–59.
Depressive disorders account for close to 41.9% of the disability from
neuropsychiatric disorders among women compared to 29.3% among men.
History
Ancient civilizations
Ancient civilizations described and treated a number of mental disorders. Mental illnesses were well known in ancient Mesopotamia, where diseases and mental disorders were believed to be caused by specific deities. Because hands symbolized control over a person, mental illnesses were known as "hands" of certain deities. One psychological illness was known as Qāt Ištar, meaning "Hand of Ishtar". Others were known as "Hand of Shamash", "Hand of the Ghost", and "Hand of the God". Descriptions of these illnesses, however, are so vague that it is
usually impossible to determine which illnesses they correspond to in
modern terminology. Mesopotamian doctors kept detailed record of their patients' hallucinations and assigned spiritual meanings to them. The royal family of Elam was notorious for its members frequently suffering from insanity. The Greeks coined terms for melancholy, hysteria and phobia and developed the humorism theory. Mental disorders were described, and treatments developed, in Persia, Arabia and in the medieval Islamic world.
Europe
Middle Ages
Conceptions of madness in the Middle Ages in Christian Europe were a
mixture of the divine, diabolical, magical and humoral and
transcendental.
In the early modern period, some people with mental disorders may have
been victims of the witch-hunts. While not every witch and sorcerer
accused were mentally ill, all mentally ill were considered to be
witches or sorcerers.
At the turn of the 16th and 17th centuries, the mentally ill were
increasingly admitted to local workhouses, jails and private madhouses
by social justice advocates such as Dorothea Dix. Many terms for mental disorder that found their way into everyday use first became popular in the 16th and 17th centuries.
Eighteenth century
Eight patients representing mental diagnoses as of the 19th century at the Salpêtrière, Paris.
By the end of the 17th century and into the Enlightenment,
madness was increasingly seen as an organic physical phenomenon with no
connection to the soul or moral responsibility. Asylum care was often
harsh and treated people like wild animals, but towards the end of the
18th century a moral treatment movement gradually developed. Clear descriptions of some syndromes may be rare prior to the 19th century.
Nineteenth century
Industrialization
and population growth led to a massive expansion of the number and size
of insane asylums in every Western country in the 19th century.
Numerous different classification schemes and diagnostic terms were
developed by different authorities, and the term psychiatry was coined (1808), though medical superintendents were still known as alienists.
Twentieth century
A patient in a strait-jacket and barrel contraption, 1908
The turn of the 20th century saw the development of psychoanalysis, which would later come to the fore, along with Kraepelin's classification scheme. Asylum "inmates" were increasingly referred to as "patients", and asylums renamed as hospitals.
Europe and the United States
Insulin shock procedure, 1950s
Early in the 20th century in the United States, a mental hygiene movement developed, aiming to prevent mental disorders. Clinical psychology and social work developed as professions. World War I saw a massive increase of conditions that came to be termed "shell shock".
World War II
saw the development in the U.S. of a new psychiatric manual for
categorizing mental disorders, which along with existing systems for
collecting census and hospital statistics led to the first Diagnostic and Statistical Manual of Mental Disorders (DSM). The International Classification of Diseases (ICD) also developed a section on mental disorders. The term stress, having emerged from endocrinology work in the 1930s, was increasingly applied to mental disorders.
Electroconvulsive therapy, insulin shock therapy, lobotomies and the "neuroleptic" chlorpromazine came to be used by mid-century. In the 1960s there were many challenges to the concept of mental illness
itself. These challenges came from psychiatrists like Thomas Szasz who
argued that mental illness was a myth used to disguise moral conflicts;
from sociologists such as Erving Goffman
who said that mental illness was merely another example of how society
labels and controls non-conformists; from behavioral psychologists who
challenged psychiatry's fundamental reliance on unobservable phenomena;
and from gay rights activists who criticized the APA's listing of
homosexuality as a mental disorder. A study published in Science by Rosenhan received much publicity and was viewed as an attack on the efficacy of psychiatric diagnosis.
Deinstitutionalization gradually occurred in the West, with isolated psychiatric hospitals being closed down in favor of community mental health services. A consumer/survivor movement gained momentum. Other kinds of psychiatric medication gradually came into use, such as "psychic energizers" (later antidepressants) and lithium. Benzodiazepines gained widespread use in the 1970s for anxiety and depression, until dependency problems curtailed their popularity.
Advances in neuroscience, genetics and psychology led to new research agendas. Cognitive behavioral therapy
and other psychotherapies developed. The DSM and then ICD adopted new
criteria-based classifications, and the number of "official" diagnoses
saw a large expansion. Through the 1990s, new SSRI-type antidepressants became some of the most widely prescribed drugs in the world, as later did antipsychotics. Also during the 1990s, a recovery approach developed.
Society and culture
Different societies or cultures, even different individuals in a subculture,
can disagree as to what constitutes optimal versus pathological
biological and psychological functioning. Research has demonstrated that
cultures vary in the relative importance placed on, for example,
happiness, autonomy, or social relationships for pleasure. Likewise, the
fact that a behavior pattern is valued, accepted, encouraged, or even
statistically normative in a culture does not necessarily mean that it
is conducive to optimal psychological functioning.
People in all cultures find some behaviors bizarre or even
incomprehensible. But just what they feel is bizarre or incomprehensible
is ambiguous and subjective.
These differences in determination can become highly contentious. The
process by which conditions and difficulties come to be defined and
treated as medical conditions and problems, and thus come under the
authority of doctors and other health professionals, is known as medicalization or pathologization.
Religion
Religious, spiritual, or transpersonal experiences and beliefs meet many criteria of delusional or psychotic disorders.
A belief or experience can sometimes be shown to produce distress or
disability—the ordinary standard for judging mental disorders. There is a link between religion and schizophrenia,
a complex mental disorder characterized by a difficulty in recognizing
reality, regulating emotional responses, and thinking in a clear and
logical manner. Those with schizophrenia commonly report some type of
religious delusion, and religion itself may be a trigger for schizophrenia.
Movements
Giorgio Antonucci
Thomas Szasz
Controversy has often surrounded psychiatry, and the term anti-psychiatry was coined by psychiatrist David Cooper in 1967. The anti-psychiatry message is that psychiatric treatments
are ultimately more damaging than helpful to patients, and psychiatry's
history involves what may now be seen as dangerous treatments. Electroconvulsive therapy was one of these, which was used widely between the 1930s and 1960s. Lobotomy was another practice that was ultimately seen as too invasive and brutal. Diazepam and other sedatives
were sometimes over-prescribed, which led to an epidemic of dependence.
There was also concern about the large increase in prescribing
psychiatric drugs for children. Some charismatic psychiatrists came to
personify the movement against psychiatry. The most influential of these
was R.D. Laing who wrote a series of best-selling books, including The Divided Self. Thomas Szasz wrote The Myth of Mental Illness. Some ex-patient groups have become militantly anti-psychiatric, often referring to themselves as "survivors". Giorgio Antonucci has questioned the basis of psychiatry through his work on the dismantling of two psychiatric hospitals (in the city of Imola), carried out from 1973 to 1996.
The consumer/survivor movement
(also known as user/survivor movement) is made up of individuals (and
organizations representing them) who are clients of mental health
services or who consider themselves survivors of psychiatric
interventions. Activists campaign for improved mental health services
and for more involvement and empowerment within mental health services,
policies and wider society. Patient advocacy organizations have expanded with increasing deinstitutionalization in developed countries, working to challenge the stereotypes, stigma and exclusion associated with psychiatric conditions. There is also a carers rights movement
of people who help and support people with mental health conditions,
who may be relatives, and who often work in difficult and time-consuming
circumstances with little acknowledgement and without pay. An anti-psychiatry
movement fundamentally challenges mainstream psychiatric theory and
practice, including in some cases asserting that psychiatric concepts
and diagnoses of 'mental illness' are neither real nor useful.
Alternatively, a movement for global mental health
has emerged, defined as 'the area of study, research and practice that
places a priority on improving mental health and achieving equity in
mental health for all people worldwide'.
Cultural bias
Current diagnostic guidelines, namely the DSM and to some extent the
ICD, have been criticized as having a fundamentally Euro-American
outlook. Opponents argue that even when diagnostic criteria are used
across different cultures, it does not mean that the underlying
constructs have validity within those cultures, as even reliable
application can prove only consistency, not legitimacy. Advocating a more culturally sensitive approach, critics such as Carl Bell and Marcello Maviglia contend that the cultural and ethnic diversity of individuals is often discounted by researchers and service providers.
Cross-cultural psychiatrist Arthur Kleinman contends that the Western bias is ironically illustrated in the introduction of cultural factors to the DSM-IV.
Disorders or concepts from non-Western or non-mainstream cultures are
described as "culture-bound", whereas standard psychiatric diagnoses are
given no cultural qualification whatsoever, revealing to Kleinman an
underlying assumption that Western cultural phenomena are universal. Kleinman's negative view towards the culture-bound syndrome
is largely shared by other cross-cultural critics. Common responses
included both disappointment over the large number of documented
non-Western mental disorders still left out and frustration that even
those included are often misinterpreted or misrepresented.
Many mainstream psychiatrists are dissatisfied with the new culture-bound diagnoses, although for partly different reasons. Robert Spitzer, a lead architect of the DSM-III,
has argued that adding cultural formulations was an attempt to appease
cultural critics, and has stated that they lack any scientific rationale
or support. Spitzer also posits that the new culture-bound diagnoses
are rarely used, maintaining that the standard diagnoses apply
regardless of the culture involved. In general, mainstream psychiatric
opinion remains that if a diagnostic category is valid, cross-cultural
factors are either irrelevant or are significant only to specific
symptom presentations.
Clinical conceptions of mental illness also overlap with personal and cultural values in the domain of morality,
so much so that it is sometimes argued that separating the two is
impossible without fundamentally redefining the essence of being a
particular person in a society.
In clinical psychiatry, persistent distress and disability indicate an
internal disorder requiring treatment; but in another context, that same
distress and disability can be seen as an indicator of emotional
struggle and the need to address social and structural problems. This dichotomy has led some academics and clinicians to advocate a postmodernist conceptualization of mental distress and well-being.
Such approaches, along with cross-cultural and "heretical" psychologies centered on alternative cultural and ethnic and race-based
identities and experiences, stand in contrast to the mainstream
psychiatric community's alleged avoidance of any explicit involvement
with either morality or culture. In many countries there are attempts to challenge perceived prejudice against minority groups, including alleged institutional racism within psychiatric services. There are also ongoing attempts to improve professional cross cultural sensitivity.
Laws and policies
Three quarters of countries around the world have mental health
legislation. Compulsory admission to mental health facilities (also
known as involuntary commitment)
is a controversial topic. It can impinge on personal liberty and the
right to choose, and carry the risk of abuse for political, social and
other reasons; yet it can potentially prevent harm to self and others,
and assist some people in attaining their right to healthcare when they
may be unable to decide in their own interests.
All human rights
oriented mental health laws require proof of the presence of a mental
disorder as defined by internationally accepted standards, but the type
and severity of disorder that counts can vary in different
jurisdictions. The two most often utilized grounds for involuntary
admission are said to be serious likelihood of immediate or imminent
danger to self or others, and the need for treatment. Applications for
someone to be involuntarily admitted usually come from a mental health
practitioner, a family member, a close relative, or a guardian.
Human-rights-oriented laws usually stipulate that independent medical
practitioners or other accredited mental health practitioners must
examine the patient separately and that there should be regular,
time-bound review by an independent review body. The individual should also have personal access to independent advocacy.
In order for involuntary treatment to be administered (by force if necessary), it should be shown that an individual lacks the mental capacity for informed consent
(i.e. to understand treatment information and its implications, and
therefore be able to make an informed choice to either accept or
refuse). Legal challenges in some areas have resulted in supreme court decisions that a person does not
have to agree with a psychiatrist's characterization of the issues as
constituting an "illness", nor agree with a psychiatrist's conviction in
medication, but only recognize the issues and the information about
treatment options.
Proxy consent (also known as surrogate or substituted decision-making)
may be transferred to a personal representative, a family member or a
legally appointed guardian. Moreover, patients may be able to make, when
they are considered well, an advance directive stipulating how they wish to be treated should they be deemed to lack mental capacity in future. The right to supported decision-making,
where a person is helped to understand and choose treatment options
before they can be declared to lack capacity, may also be included in
legislation. There should at the very least be shared decision-making as far as possible. Involuntary treatment laws are increasingly extended to those living in the community, for example outpatient commitment laws (known by different names) are used in New Zealand, Australia, the United Kingdom and most of the United States.
The World Health Organization reports that in many instances
national mental health legislation takes away the rights of persons with
mental disorders rather than protecting rights, and is often outdated. In 1991, the United Nations adopted the Principles for the Protection of Persons with Mental Illness and the Improvement of Mental Health Care, which established minimum human rights standards of practice in the mental health field. In 2006, the UN formally agreed the Convention on the Rights of Persons with Disabilities to protect and enhance the rights and opportunities of disabled people, including those with psychosocial disabilities.
The term insanity, sometimes used colloquially as a synonym for mental illness, is often used technically as a legal term. The insanity defense may be used in a legal trial (known as the mental disorder defense in some countries).
Perception and discrimination
Stigma
The social stigma
associated with mental disorders is a widespread problem. The US
Surgeon General stated in 1999 that: "Powerful and pervasive, stigma
prevents people from acknowledging their own mental health problems,
much less disclosing them to others." In the United States, racial and ethnic minorities are more likely to experience mental health disorders often due to low socioeconomic status, and discrimination.
Employment discrimination is reported to play a significant part in the high rate of unemployment among those with a diagnosis of mental illness. An Australian study found that having a mental illness is a bigger barrier to employment than a physical disability. The mentally ill are stigmatized in Chinese society and can not legally marry.
Efforts are being undertaken worldwide to eliminate the stigma of mental illness, although the methods and outcomes used have sometimes been criticized.
Media and general public
Media coverage of mental illness comprises predominantly negative and pejorative
depictions, for example, of incompetence, violence or criminality, with
far less coverage of positive issues such as accomplishments or human rights issues.
Such negative depictions, including in children's cartoons, are thought
to contribute to stigma and negative attitudes in the public and in
those with mental health problems themselves, although more sensitive or
serious cinematic portrayals have increased in prevalence.
In the United States, the Carter Center has created fellowships for journalists in South Africa, the U.S., and Romania, to enable reporters to research and write stories on mental health topics. Former US First Lady Rosalynn Carter
began the fellowships not only to train reporters in how to sensitively
and accurately discuss mental health and mental illness, but also to
increase the number of stories on these topics in the news media. There is also a World Mental Health Day, which in the US and Canada falls within a Mental Illness Awareness Week.
The general public have been found to hold a strong stereotype of dangerousness and desire for social distance from individuals described as mentally ill.
A US national survey found that a higher percentage of people rate
individuals described as displaying the characteristics of a mental
disorder as "likely to do something violent to others", compared to the
percentage of people who are rating individuals described as being
"troubled".
Recent depictions in media have included leading characters
successfully living with and managing a mental illness, including in
bipolar disorder in Homeland (2011) and posttraumatic stress disorder in Iron Man 3 (2013).
Violence
Despite public or media opinion, national studies have indicated that
severe mental illness does not independently predict future violent
behavior, on average, and is not a leading cause of violence in society.
There is a statistical association with various factors that do relate
to violence (in anyone), such as substance abuse and various personal,
social and economic factors. A 2015 review found that in the United States, about 4% of violence is attributable to people diagnosed with mental illness,
and a 2014 study found that 7.5% of crimes committed by mentally ill
people were directly related to the symptoms of their mental illness. The majority of people with serious mental illness are never violent.
In fact, findings consistently indicate that it is many times
more likely that people diagnosed with a serious mental illness living
in the community will be the victims rather than the perpetrators of
violence.
In a study of individuals diagnosed with "severe mental illness" living
in a US inner-city area, a quarter were found to have been victims
of at least one violent crime over the course of a year, a proportion
eleven times higher than the inner-city average, and higher in every
category of crime including violent assaults and theft.
People with a diagnosis may find it more difficult to secure
prosecutions, however, due in part to prejudice and being seen as less
credible.
However, there are some specific diagnoses, such as childhood conduct disorder or adult antisocial personality disorder or psychopathy,
which are defined by, or are inherently associated with, conduct
problems and violence. There are conflicting findings about the extent
to which certain specific symptoms, notably some kinds of psychosis
(hallucinations or delusions) that can occur in disorders such as
schizophrenia, delusional disorder or mood disorder, are linked to an
increased risk of serious violence on average. The mediating
factors of violent acts, however, are most consistently found to be
mainly socio-demographic and socio-economic factors such as being young,
male, of lower socioeconomic status and, in particular, substance abuse (including alcoholism) to which some people may be particularly vulnerable.
High-profile cases have led to fears that serious crimes, such as
homicide, have increased due to deinstitutionalization, but the
evidence does not support this conclusion.
Violence that does occur in relation to mental disorder (against the
mentally ill or by the mentally ill) typically occurs in the context of
complex social interactions, often in a family setting rather than
between strangers. It is also an issue in health care settings and the wider community.
Mental health
The recognition and understanding of mental health conditions have changed over time and across cultures and there are still variations in definition, assessment and classification, although standard guideline criteria are widely used. In many cases, there appears to be a continuum between mental health and mental illness, making diagnosis complex. According to the World Health Organization
(WHO), over a third of people in most countries report problems at some
time in their life which meet criteria for diagnosis of one or more of
the common types of mental disorder. Mental health can be defined as an absence of mental disorder.
Other animals
Psychopathology in non-human primates
has been studied since the mid-20th century. Over 20 behavioral
patterns in captive chimpanzees have been documented as (statistically)
abnormal for frequency, severity or oddness—some of which have also been
observed in the wild. Captive great apes show gross behavioral abnormalities such as stereotypy of movements, self-mutilation,
disturbed emotional reactions (mainly fear or aggression) towards
companions, lack of species-typical communications, and generalized learned helplessness.
In some cases such behaviors are hypothesized to be equivalent to
symptoms associated with psychiatric disorders in humans such as
depression, anxiety disorders, eating disorders and post-traumatic
stress disorder. Concepts of antisocial, borderline and schizoid
personality disorders have also been applied to non-human great apes.
The risk of anthropomorphism
is often raised with regard to such comparisons, and assessment of
non-human animals cannot incorporate evidence from linguistic
communication. However, available evidence may range from nonverbal
behaviors—including physiological responses and homologous facial
displays and acoustic utterances—to neurochemical studies. It is pointed
out that human psychiatric classification is often based on statistical
description and judgment of behaviors (especially when speech or
language is impaired) and that the use of verbal self-report is itself
problematic and unreliable.
Psychopathology has generally been traced, at least in captivity,
to adverse rearing conditions such as early separation of infants from
mothers; early sensory deprivation; and extended periods of social
isolation. Studies have also indicated individual variation in
temperament, such as sociability or impulsiveness. Particular causes of
problems in captivity have included integration of strangers into
existing groups and a lack of individual space, in which context some
pathological behaviors have also been seen as coping mechanisms.
Remedial interventions have included careful individually tailored
re-socialization programs, behavior therapy,
environment enrichment, and on rare occasions psychiatric drugs.
Socialization has been found to work 90% of the time in disturbed
chimpanzees, although restoration of functional sexuality and
care-giving is often not achieved.
Laboratory researchers sometimes try to develop animal models
of human mental disorders, including by inducing or treating symptoms
in animals through genetic, neurological, chemical or behavioral
manipulation, but this has been criticized on empirical grounds and opposed on animal rights grounds.