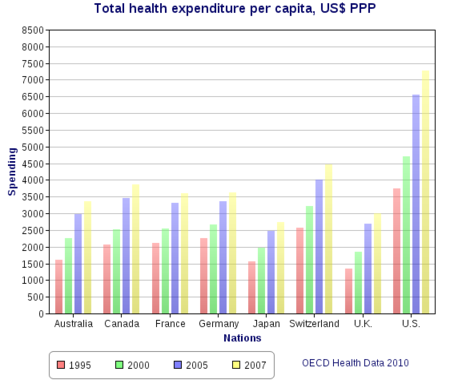
Health spending per capita, in $US PPP-adjusted , with the US and Canada compared amongst other first world nations.
Comparison of the healthcare systems in Canada and the United States is often made by government, public health and public policy analysts. The two countries had similar healthcare systems
before Canada changed its system in the 1960s and 1970s. The United
States spends much more money on healthcare than Canada, on both a
per-capita basis and as a percentage of GDP.
In 2006, per-capita spending for health care in Canada was US$3,678; in
the U.S., US$6,714. The U.S. spent 15.3% of GDP on healthcare in that
year; Canada spent 10.0%.
In 2006, 70% of healthcare spending in Canada was financed by
government, versus 46% in the United States. Total government spending
per capita in the U.S. on healthcare was 23% higher than Canadian
government spending, and U.S. government expenditure on healthcare was
just under 83% of total Canadian spending (public and private) though
these statistics don't take into account population differences.
Studies have come to different conclusions about the result of
this disparity in spending. A 2007 review of all studies comparing
health outcomes in Canada and the US in a Canadian peer-reviewed medical
journal found that "health outcomes may be superior in patients cared
for in Canada versus the United States, but differences are not
consistent."
Some of the noted differences were a higher life expectancy in Canada,
as well as a lower infant mortality rate than the United States.
One commonly cited comparison, the 2000 World Health
Organization's ratings of "overall health service performance", which
used a "composite measure of achievement in the level of health, the
distribution of health, the level of responsiveness and fairness of
financial contribution", ranked Canada 30th and the US 37th among 191
member nations. This study rated the US "responsiveness", or quality of
service for individuals receiving treatment, as 1st, compared with 7th
for Canada. However, the average life expectancy for Canadians was
80.34 years compared with 78.6 years for residents of the US.
The WHO's study methods were criticized by some analyses.
While life-expectancy and infant mortality are commonly used in
comparing nationwide health care, they are in fact affected by many
factors other than the quality of a nation's health care system,
including individual behavior and population makeup. A 2007 report by the Congressional Research Service carefully summarizes some recent data and noted the "difficult research issues" facing international comparisons.
Government involvement
In
2004, government funding of healthcare in Canada was equivalent to
$1,893 per person. In the US, government spending per person was
$2,728.
The Canadian healthcare system is composed of at least 10 mostly
autonomous provincial healthcare systems that report to their provincial
governments, and a federal system which covers the military and First Nations. This causes a significant degree of variation in funding and coverage within the country.
History
Canada and the US had similar healthcare systems in the early 1960s, but now have a different mix of funding mechanisms. Canada's universal single-payer healthcare system covers about 70% of expenditures, and the Canada Health Act
requires that all insured persons be fully insured, without co-payments
or user fees, for all medically necessary hospital and physician care. About 91% of hospital expenditures and 99% of total physician services are financed by the public sector.
In the United States, with its mixed public-private system, 16% or 45
million American residents are uninsured at any one time. The U.S. is one of two OECD
countries not to have some form of universal health coverage, the other
being Turkey. Mexico established a universal healthcare program by
November 2008.
Health insurance
The governments of both nations are closely involved in healthcare. The central structural difference between the two is in health insurance.
In Canada, the federal government is committed to providing funding
support to its provincial governments for healthcare expenditures as
long as the province in question abides by accessibility guarantees as
set out in the Canada Health Act, which explicitly prohibits billing end users for procedures that are covered by Medicare.
While some label Canada's system as "socialized medicine", health
economists do not use that term. Unlike systems with public delivery,
such as the UK, the Canadian system provides public coverage for a
combination of public and private delivery. Princeton University health
economist Uwe E. Reinhardt says that single-payer systems are not
"socialized medicine" but "social insurance" systems, since providers
(such as doctors) are largely in the private sector.
Similarly, Canadian hospitals are controlled by private boards or
regional health authorities, rather than being part of government.
In the US, direct government funding of health care is limited to Medicare, Medicaid, and the State Children's Health Insurance Program
(SCHIP), which cover eligible senior citizens, the very poor, disabled
persons, and children. The federal government also runs the Veterans Administration,
which provides care directly to retired or disabled veterans, their
families, and survivors through medical centers and clinics.
The U.S. government also runs the Military Health System.
In fiscal year 2007, the MHS had a total budget of $39.4 billion and
served approximately 9.1 million beneficiaries, including active-duty
personnel and their families, and retirees and their families. The MHS
includes 133,000 personnel, 86,000 military and 47,000 civilian, working
at more than 1,000 locations worldwide, including 70 inpatient
facilities and 1,085 medical, dental, and veterans' clinics.
One study estimates that about 25 percent of the uninsured in the
U.S. are eligible for these programs but remain unenrolled; however,
extending coverage to all who are eligible remains a fiscal and
political challenge.
For everyone else, health insurance must be paid for privately.
Some 59% of U.S. residents have access to health care insurance through
employers, although this figure is decreasing, and coverages as well as
workers' expected contributions vary widely.
Those whose employers do not offer health insurance, as well as those
who are self-employed or unemployed, must purchase it on their own.
Nearly 27 million of the 45 million uninsured U.S. residents worked at
least part-time in 2007, and more than a third were in households that
earned $50,000 or more per year.
Funding
Despite
the greater role of private business in the US, federal and state
agencies are increasingly involved, paying about 45% of the $2.2
trillion the nation spent on medical care in 2004. The U.S. government spends more on healthcare than on Social Security and national defense combined, according to the Brookings Institution.
Beyond its direct spending, the US government is also highly
involved in healthcare through regulation and legislation. For example,
the Health Maintenance Organization Act of 1973 provided grants and loans to subsidize Health Maintenance Organizations
and contained provisions to stimulate their popularity. HMOs had been
declining before the law; by 2002 there were 500 such plans enrolling 76
million people.
The Canadian system has been 69–75% publicly funded,
though most services are delivered by private providers, including
physicians (although they may derive their revenue primarily from
government billings). Although some doctors work on a purely
fee-for-service basis (usually family physicians), some family
physicians and most specialists are paid through a combination of
fee-for-service and fixed contracts with hospitals or health service
management organizations.
Canada's universal health plans do not cover certain services. Non-cosmetic dental care
is covered for children up to age 14 in some provinces. Outpatient
prescription drugs are not required to be covered, but some provinces
have drug cost programs that cover most drug costs for certain
populations. In every province, seniors receiving the Guaranteed Income Supplement have significant additional coverage; some provinces expand forms of drug coverage to all seniors, low-income families, those on social assistance, or those with certain medical conditions. Some provinces cover all drug prescriptions over a certain portion of a family's income. Drug prices are also regulated, so brand-name prescription drugs are often significantly cheaper than in the U.S. Optometry is only covered in some provinces and is sometimes only covered for children under a certain age.
Visits to non-physician specialists may require an additional fee.
Also, some procedures are only covered under certain circumstances. For
example, circumcision is not covered, and a fee is usually charged when a parent requests the procedure; however, if an infection or medical necessity arises, the procedure would be covered.
According to Dr. Albert Schumacher, former president of the
Canadian Medical Association, an estimated 75 percent of Canadian
healthcare services are delivered privately, but funded publicly.
Frontline practitioners whether they're GPs or specialists by and large are not salaried. They're small hardware stores. Same thing with labs and radiology clinics ... The situation we are seeing now are more services around not being funded publicly but people having to pay for them, or their insurance companies. We have sort of a passive privatization.
Coverage and access
In
both Canada and the United States, access can be a problem. Studies
suggest that 40% of U.S. citizens do not have adequate health insurance,
if any at all. In Canada, 5% of Canadian citizens have not been able to
find a regular doctor, with a further 9% having never looked for one.
Yet, even if some cannot find a family doctor, every Canadian citizen is
covered by the national health care system. The U.S. data is evidenced
in a 2007 Consumer Reports study on the U.S. health care system which
showed that the underinsured account for 24% of the U.S. population and
live with skeletal health insurance that barely covers their medical
needs and leaves them unprepared to pay for major medical expenses.
When added to the population of uninsured (approximately 16% of the U.S.
population), a total of 40% of Americans ages 18–64 have inadequate
access to healthcare, according to the Consumer Reports study. The Canadian data comes from the 2003 Canadian Community Health Survey.
In the U.S., the federal government does not guarantee universal healthcare to all its citizens, but publicly funded healthcare programs help to provide for the elderly, disabled, the poor, and children. The Emergency Medical Treatment and Active Labor Act or EMTALA also ensures public access to emergency services.
The EMTALA law forces emergency healthcare providers to stabilize an
emergency health crisis and cannot withhold treatment for lack of
evidence of insurance coverage or other evidence of the ability to pay.
EMTALA does not absolve the person receiving emergency care of the
obligation to meet the cost of emergency healthcare not paid for at the
time and it is still within the right of the hospital to pursue any
debtor for the cost of emergency care provided. In Canada, emergency
room treatment for legal Canadian residents is not charged to the
patient at time of service but is met by the government.
According to the United States Census Bureau, 59.3% of U.S. citizens have health insurance
related to employment, 27.8% have government-provided health-insurance;
nearly 9% purchase health insurance directly (there is some overlap in
these figures), and 15.3% (45.7 million) were uninsured in 2007. An estimated 25 percent of the uninsured are eligible for government programs but unenrolled. About a third of the uninsured are in households earning more than $50,000 annually.
A 2003 report by the Congressional Budget Office found that many
people lack health insurance only temporarily, such as after leaving one
employer and before a new job. The number of chronically uninsured
(uninsured all year) was estimated at between 21 and 31 million in 1998.
Another study, by the Kaiser Commission on Medicaid and the Uninsured,
estimated that 59 percent of uninsured adults have been uninsured for at
least two years. One indicator of the consequences of Americans' inconsistent health care coverage is a study in Health Affairs that concluded that half of personal bankruptcies involved medical bills. Although other sources dispute this, it is possible that medical debt is the principal cause of bankruptcy in the United States.
A number of clinics
provide free or low-cost non-emergency care to poor, uninsured
patients. The National Association of Free Clinics claims that its
member clinics provide $3 billion in services to some 3.5 million
patients annually.
A peer-reviewed comparison study of healthcare access in the two
countries published in 2006 concluded that U.S. residents are one third
less likely to have a regular medical doctor, one fourth more likely to
have unmet healthcare needs, and are more than twice as likely to forgo
needed medicines.
The study noted that access problems "were particularly dire for the US
uninsured." Those who lack insurance in the U.S. were much less
satisfied, less likely to have seen a doctor, and more likely to have
been unable to receive desired care than both Canadians and insured
Americans.
Another cross-country study compared access to care based on immigrant status in Canada and the U.S.
Findings showed that in both countries, immigrants had worse access to
care than non-immigrants. Specifically, immigrants living in Canada were
less likely to have timely Pap tests compared with native-born
Canadians; in addition, immigrants in the U.S. were less likely to have a
regular medical doctor and an annual consultation with a health care
provider compared with native-born Americans. In general, immigrants in
Canada had better access to care than those in the U.S., but most of the
differences were explained by differences in socioeconomic status
(income, education) and insurance coverage across the two countries.
However, immigrants in the U.S. were more likely to have timely Pap
tests than immigrants in Canada.
Cato Institute
has expressed concerns that the U.S. government has restricted the
freedom of Medicare patients to spend their own money on healthcare, and
has contrasted these developments with the situation in Canada, where
in 2005 the Supreme Court of Canada ruled that the province of Quebec
could not prohibit its citizens from purchasing covered services through
private health insurance. The institute has urged the Congress to
restore the right of American seniors to spend their own money on
medical care.
Coverage for Mental Health
The Canada Health Act covers the services of psychiatrists, who are medical doctors with additional training in psychiatry but does not cover treatment by a psychologist or psychotherapist unless the practitioner is also a medical doctor. Goods and Services Tax or Harmonized Sales Tax (depending on the province) applies to the services of psychotherapists.
Some provincial or territorial programs and some private insurance
plans may cover the services of psychologists and psychotherapists, but
there is no federal mandate for such services in Canada. In the U.S.,
the Affordable Care Act
includes prevention, early intervention, and treatment of mental and/or
substance use disorders as an "essential health benefit" (EHB) that
must be covered by health plans that are offered through the Health Insurance Marketplace.
Under the Affordable Care Act, most health plans must also cover
certain preventive services without a copayment, co-insurance, or
deductible.
In addition, the U.S. Mental Health Parity and Addiction Equity Act
(MHPAEA) of 2008 mandates "parity" between mental health and/or
substance use disorder (MH/SUD) benefits and medical/surgical benefits
covered by a health plan. Under that law, if a health care plan offers
mental health and/or substance use disorder benefits, it must offer the
benefits on par with the other medical/surgical benefits it covers.
Wait times
One
complaint about both the U.S. and Canadian systems is waiting times,
whether for a specialist, major elective surgery, such as hip replacement, or specialized treatments, such as radiation for breast cancer;
wait times in each country are affected by various factors. In the
United States, access is primarily determined by whether a person has
access to funding to pay for treatment and by the availability of
services in the area and by the willingness of the provider to deliver
service at the price set by the insurer. In Canada, the wait time is set
according to the availability of services in the area and by the
relative need of the person needing treatment.
As reported by the Health Council of Canada,
a 2010 Commonwealth survey found that 39% of Canadians waited 2 hours
or more in the emergency room, versus 31% in the U.S.; 43% waited 4
weeks or more to see a specialist, versus 10% in the U.S. The same
survey states that 37% of Canadians say it is difficult to access care
after hours (evenings, weekends or holidays) without going to the
emergency department over 34% of Americans. Furthermore, 47% of
Canadians and 50% of Americans who visited emergency departments over
the past two years feel that they could have been treated at their
normal place of care if they were able to get an appointment.
A report published by Health Canada in 2008 included statistics on self-reported wait times for diagnostic services. The median wait time for diagnostic services such as MRI and CAT scans is two weeks with 89.5% waiting less than 3 months. The median wait time to see a special physician is a little over four weeks with 86.4% waiting less than 3 months. The median wait time for surgery is a little over four weeks with 82.2% waiting less than 3 months. In the U.S., patients on Medicaid,
the low-income government programs, can wait three months or more to
see specialists. Because Medicaid payments are low, some have claimed
that some doctors do not want to see Medicaid patients. For example, in Benton Harbor, Michigan,
specialists agreed to spend one afternoon every week or two at a
Medicaid clinic, which meant that Medicaid patients had to make
appointments not at the doctor's office, but at the clinic, where
appointments had to be booked months in advance. A 2009 study found that on average the wait in the United States to see a medical specialist is 20.5 days.
In a 2009 survey of physician appointment wait times in the
United States, the average wait time for an appointment with an
orthopedic surgeon in the country as a whole was 17 days. In Dallas,
Texas the wait was 45 days (the longest wait being 365 days).
Nationwide across the U.S. the average wait time to see a family doctor
was 20 days. The average wait time to see a family practitioner in Los
Angeles, California was 59 days and in Boston, Massachusetts it was 63
days.
Studies by the Commonwealth Fund
found that 42% of Canadians waited 2 hours or more in the emergency
room, vs. 29% in the U.S.; 57% waited 4 weeks or more to see a
specialist, vs. 23% in the U.S., but Canadians had more chances of
getting medical attention at nights, or on weekends and holidays than
their American neighbors without the need to visit an ER (54% compared
to 61%). Statistics from the Canadian free market think tank Fraser Institute
in 2008 indicate that the average wait time between the time when a
general practitioner refers a patient for care and the receipt of
treatment was almost four and a half months in 2008, roughly double what
it had been 15 years before.
A 2003 survey of hospital administrators conducted in Canada, the
U.S., and three other countries found dissatisfaction with both the
U.S. and Canadian systems. For example, 21% of Canadian hospital
administrators, but less than 1% of American administrators, said that
it would take over three weeks to do a biopsy for possible breast cancer
on a 50-year-old woman; 50% of Canadian administrators versus none of
their American counterparts said that it would take over six months for a
65-year-old to undergo a routine hip replacement surgery. However, U.S.
administrators were the most negative about their country's system.
Hospital executives in all five countries expressed concerns about
staffing shortages and emergency department waiting times and quality.
In a letter to the Wall Street Journal, Robert Bell, the President and CEO of University Health Network, Toronto, said that Michael Moore's film Sicko
"exaggerated the performance of the Canadian health system — there is
no doubt that too many patients still stay in our emergency departments
waiting for admission to scarce hospital beds." However, "Canadians
spend about 55% of what Americans spend on health care and have longer
life expectancy and lower infant mortality rates. Many Americans have
access to quality healthcare. All Canadians have access to similar care
at a considerably lower cost." There is "no question" that the lower
cost has come at the cost of "restriction of supply with sub-optimal
access to services," said Bell. A new approach is targeting waiting
times, which are reported on public websites.
In 2007 Shona Holmes, a Waterdown, Ontario woman who had a Rathke's cleft cyst removed at the Mayo Clinic in Arizona, sued the Ontario government for failing to reimburse her $95,000 in medical expenses.
Holmes had characterized her condition as an emergency, said she was
losing her sight and portrayed her condition as a life-threatening brain
cancer.
In July 2009 Holmes agreed to appear in television ads broadcast in the
United States warning Americans of the dangers of adopting a
Canadian-style health care system.
The ads she appeared in triggered debates on both sides of the border.
After her ad appeared critics pointed out discrepancies in her story,
including that Rathke's cleft cyst, the condition she was treated for, was not a form of cancer, and was not life-threatening.
Price of health care and administration overheads
Healthcare
is one of the most expensive items of both nations' budgets. In the
United States, the various levels of government spend more per capita
than levels of government do in Canada. In 2004, Canada
government-spending was $2,120 (in US dollars) per person, while the
United States government-spending $2,724.
A 1999 report found that after exclusions, administration
accounted for 31.0% of healthcare expenditures in the United States, as
compared with 16.7% in Canada. In looking at the insurance element, in
Canada, the provincial single-payer insurance system operated with
overheads of 1.3%, comparing favourably with private insurance overheads
(13.2%), U.S. private insurance overheads (11.7%) and U.S. Medicare and
Medicaid program overheads (3.6% and 6.8% respectively). The report
concluded by observing that gap between U.S. and Canadian spending on
administration had grown to $752 per capita and that a large sum might
be saved in the United States if the U.S. implemented a Canadian-style
system.
However, U.S. government spending covers less than half of all
healthcare costs. Private spending is also far greater in the U.S. than
in Canada. In Canada, an average of $917 was spent annually by
individuals or private insurance companies for health care, including
dental, eye care, and drugs. In the U.S., this sum is $3,372. In 2006, healthcare consumed 15.3% of U.S. annual GDP. In Canada, only 10% of GDP was spent on healthcare.
This difference is a relatively recent development. In 1971 the nations
were much closer, with Canada spending 7.1% of GDP while the U.S. spent
7.6%.
Some who advocate against greater government involvement in
healthcare have asserted that the difference in costs between the two
nations is partially explained by the differences in their demographics. Illegal immigrants, more prevalent in the U.S. than in Canada,
also add a burden to the system, as many of them do not carry health
insurance and rely on emergency rooms — which are legally required to
treat them under EMTALA — as a principal source of care. In Colorado, for example, an estimated 80% of undocumented immigrants do not have health insurance.
The mixed system in the United States has become more similar to the Canadian system. In recent decades, managed care
has become prevalent in the United States, with some 90% of privately
insured Americans belonging to plans with some form of managed care. In managed care,
insurance companies control patients' health care to reduce costs, for
instance by demanding a second opinion prior to some expensive
treatments or by denying coverage for treatments not considered worth
their cost.
Administrative costs are also higher in the United States than in Canada.
Through all entities in its public–private system, the US spends more per capita than any other nation in the world, but is the only wealthy industrialized country in the world that lacks some form of universal healthcare. In March 2010, the US Congress passed regulatory reform of the American health insurance system. However, since this legislation is not fundamental healthcare
reform, it is unclear what its effect will be and as the new
legislation is implemented in stages, with the last provision in effect
in 2018, it will be some years before any empirical evaluation of the
full effects on the comparison could be determined.
Healthcare costs in both countries are rising faster than inflation.
As both countries consider changes to their systems, there is debate
over whether resources should be added to the public or private sector.
Although Canadians and Americans have each looked to the other for ways
to improve their respective health care systems, there exists a substantial amount of conflicting information regarding the relative merits of the two systems. In the U.S., Canada's mostly monopsonistic health system is seen by different sides of the ideological spectrum as either a model to be followed or avoided.
Medical professionals
Some of the extra money spent in the United States goes to physicians, nurses, and other medical professionals. According to health data collected by the OECD, average income for physicians in the United States in 1996 was nearly twice that for physicians in Canada. In 2012, the gross average salary for doctors in Canada was CDN$328,000. Out of the gross amount, doctors pay for taxes, rent, staff salaries and equipment.
When comparing average incomes of doctors in Canada and U.S., it should
be kept in mind that malpractice insurance premiums may differ
significantly between Canada and the U.S., and the proportion of doctors
who are specialists differs. In Canada, less than half of doctors are
specialists whereas more than 70% of doctors are specialists in the U.S.
Canada has fewer doctors per capita than the United States. In
the U.S, there were 2.4 doctors per 1,000 people in 2005; in Canada,
there were 2.2.
Some doctors leave Canada to pursue career goals or higher pay in the
U.S., though significant numbers of physicians from countries such as
China, India, Pakistan and South Africa immigrate to practice in Canada.
Many Canadian physicians and new medical graduates also go to the U.S.
for post-graduate training in medical residencies. As it is a much
larger market, new and cutting-edge sub-specialties are more widely
available in the U.S. as opposed to Canada. However, statistics
published in 2005 by the Canadian Institute for Health Information
(CIHI), show that, for the first time since 1969 (the period for which
data are available), more physicians returned to Canada than moved
abroad.
Drugs
Both Canada
and the United States have limited programs to provide prescription
drugs to the needy. In the U.S., the introduction of Medicare Part D
has extended partial coverage for pharmaceuticals to Medicare
beneficiaries. In Canada all drugs given in hospitals fall under
Medicare, but other prescriptions do not. The provinces all have some
programs to help the poor and seniors have access to drugs, but while
there have been calls to create one, no national program exists. About two thirds of Canadians have private prescription drug coverage, mostly through their employers.
In both countries, there is a significant population not fully covered
by these programs. A 2005 study found that 20% of Canada's and 40% of
America's sicker adults did not fill a prescription because of cost.
Furthermore, the 2010 Commonwealth Fund International Health
Policy Survey indicates that 4% of Canadians indicated that they did not
visit a doctor because of cost compared with 22% of Americans.
Additionally, 21% of Americans have said that they did not fill a
prescription for medicine or have skipped doses due to cost. That is
compared with 10% of Canadians.
One of the most important differences between the two countries
is the much higher cost of drugs in the United States. In the U.S., $728
per capita is spent each year on drugs, while in Canada it is $509.
At the same time, consumption is higher in Canada, with about 12
prescriptions being filled per person each year in Canada and 10.6 in
the United States.
The main difference is that patented drug prices in Canada average
between 35% and 45% lower than in the United States, though generic
prices are higher.
The price differential for brand-name drugs between the two countries
has led Americans to purchase upward of $1 billion US in drugs per year
from Canadian pharmacies.
There are several reasons for the disparity. The Canadian system
takes advantage of centralized buying by the provincial governments that
have more market heft and buy in bulk, lowering prices. By contrast,
the U.S. has explicit laws that prohibit Medicare or Medicaid
from negotiating drug prices. In addition, price negotiations by
Canadian health insurers are based on evaluations of the clinical
effectiveness of prescription drugs,
allowing the relative prices of therapeutically similar drugs to be
considered in context. The Canadian Patented Medicine Prices Review
Board also has the authority to set a fair and reasonable price on
patented products, either comparing it to similar drugs already on the
market, or by taking the average price in seven developed nations.
Prices are also lowered through more limited patent protection in
Canada. In the U.S., a drug patent may be extended five years to make up
for time lost in development. Some generic drugs are thus available on Canadian shelves sooner.
The pharmaceutical industry is important in both countries,
though both are net importers of drugs. Both countries spend about the
same amount of their GDP on pharmaceutical research, about 0.1% annually
Technology
The United States spends more on technology than Canada. In a 2004 study on medical imaging in Canada, it was found that Canada had 4.6 MRI scanners per million population while the U.S. had 19.5 per million. Canada's 10.3 CT scanners per million also ranked behind the U.S., which had 29.5 per million.
The study did not attempt to assess whether the difference in the
number of MRI and CT scanners had any effect on the medical outcomes or
were a result of overcapacity but did observe that MRI scanners are used
more intensively in Canada than either the U.S. or Great Britain.
This disparity in the availability of technology, some believe, results
in longer wait times. In 1984 wait times of up to 22 months for an MRI were alleged in Saskatchewan.
However, according to more recent official statistics (2007), all
emergency patients receive MRIs within 24 hours, those classified as
urgent receive them in under 3 weeks and the maximum elective wait time
is 19 weeks in Regina and 26 weeks in Saskatoon, the province's two
largest metropolitan areas.
According to the Health Council of Canada's 2010 report
"Decisions, Decisions: Family doctors as gatekeepers to prescription
drugs and diagnostic imaging in Canada", the Canadian federal government
invested $3 billion over 5 years (2000–2005) in relation to diagnostic
imaging and agreed to invest a further $2 billion to reduce wait times.
These investments led to an increase in the number of scanners across
Canada as well as the number of exams being performed. The number of CT
scanners increased from 198 to 465 and MRI scanners increased from 19
to 266 (more than tenfold) between 1990 and 2009. Similarly, the number
of CT exams increased by 58% and MRI exams increased by 100% between
2003 and 2009. In comparison to other OECD countries, including the US,
Canada's rates of MRI and CT exams falls somewhere in the middle.
Nevertheless, the Canadian Association of Radiologists claims that as
many as 30% of diagnostic imaging scans are inappropriate and contribute
no useful information.
Malpractice litigation
The extra cost of malpractice lawsuits is a proportion of health spending in both the U.S. (1.7% in 2002)
and Canada (0.27% in 2001 or $237 million). In Canada the total cost of
settlements, legal fees, and insurance comes to $4 per person each
year,
but in the United States it is over $16. Average payouts to American
plaintiffs were $265,103, while payouts to Canadian plaintiffs were
somewhat higher, averaging $309,417. However, malpractice suits are far more common in the U.S., with 350% more suits filed each year per person.
While malpractice costs are significantly higher in the U.S., they make
up only a small proportion of total medical spending. The total cost of
defending and settling malpractice lawsuits in the U.S. in 2004 was
over $28 billion. Critics say that defensive medicine consumes up to 9% of American healthcare expenses., but CBO studies suggest that it is much smaller.
Ancillary expenses
There
are a number of ancillary costs that are higher in the U.S.
Administrative costs are significantly higher in the U.S.; government
mandates on record keeping and the diversity of insurers, plans and
administrative layers involved in every transaction result in greater
administrative effort. One recent study comparing administrative costs
in the two countries found that these costs in the U.S. are roughly
double what they are in Canada.
Another ancillary cost is marketing, both by insurance companies and
health care providers. These costs are higher in the U.S., contributing
to higher overall costs in that nation.
Healthcare outcomes
In the World Health Organization's rankings of healthcare system performance
among 191 member nations published in 2000, Canada ranked 30th and the
U.S. 37th, while the overall health of Canadians was ranked 35th and
Americans 72nd.
However, the WHO's methodologies, which attempted to measure how
efficiently health systems translate expenditure into health, generated
broad debate and criticism.
Researchers caution against inferring healthcare quality from
some health statistics. June O'Neill and Dave O'Neill point out that
"... life expectancy and infant mortality
are both poor measures of the efficacy of a health care system because
they are influenced by many factors that are unrelated to the quality
and accessibility of medical care".
In 2007, Gordon H. Guyatt et al. conducted a meta-analysis, or
systematic review, of all studies that compared health outcomes for
similar conditions in Canada and the U.S., in Open Medicine, an
open-access peer-reviewed Canadian medical journal. They concluded,
"Available studies suggest that health outcomes may be superior in
patients cared for in Canada versus the United States, but differences
are not consistent." Guyatt identified 38 studies addressing conditions
including cancer, coronary artery disease, chronic medical illnesses and
surgical procedures. Of 10 studies with the strongest statistical
validity, 5 favoured Canada, 2 favoured the United States, and 3 were
equivalent or mixed. Of 28 weaker studies, 9 favoured Canada, 3 favoured
the United States, and 16 were equivalent or mixed. Overall, results
for mortality favoured Canada with a 5% advantage, but the results were
weak and varied. The only consistent pattern was that Canadian patients
fared better in kidney failure.
In terms of population health, life expectancy
in 2006 was about two and a half years longer in Canada, with Canadians
living to an average of 79.9 years and Americans 77.5 years. Infant and child mortality rates are also higher in the U.S.
Some comparisons suggest that the American system underperforms
Canada's system as well as those of other industrialized nations with
universal coverage.
For example, a ranking by the World Health Organization of health care
system performance among 191 member nations, published in 2000, ranked
Canada 30th and the U.S. 37th, and the overall health of Canada 35th to
the American 72nd.
The WHO did not merely consider health care outcomes, but also placed
heavy emphasis on the health disparities between rich and poor, funding
for the health care needs of the poor, and the extent to which a country
was reaching the potential health care outcomes they believed were
possible for that nation. In an international comparison of 21 more
specific quality indicators conducted by the Commonwealth Fund
International Working Group on Quality Indicators, the results were more
divided. One of the indicators was a tie, and in 3 others, data was
unavailable from one country or the other. Canada performed better on 11
indicators; such as survival rates for colorectal cancer, childhood leukemia,
and kidney and liver transplants. The U.S. performed better on 6
indicators, including survival rates for breast and cervical cancer, and
avoidance of childhood diseases such as pertussis and measles. It
should be noted that the 21 indicators were distilled from a starting
list of 1000. The authors state that, "It is an opportunistic list,
rather than a comprehensive list."
Some of the difference in outcomes may also be related to
lifestyle choices. The OECD found that Americans have slightly higher
rates of smoking and alcohol consumption than do Canadians as well as significantly higher rates of obesity. A joint US-Canadian study found slightly higher smoking rates among Canadians.
Another study found that Americans have higher rates not only of
obesity, but also of other health risk factors and chronic conditions,
including physical inactivity, diabetes, hypertension, arthritis, and
chronic obstructive pulmonary disease.
While a Canadian systematic review
stated that the differences in the systems of Canada and the United
States could not alone explain differences in healthcare outcomes,
the study didn't consider that over 44,000 Americans die every year due
to not having a single payer system for healthcare in the United States
and it didn't consider the millions more that live without proper
medical care due to a lack of insurance.
The United States and Canada have different racial makeups,
different obesity rates and different alcoholism rates, which would
likely cause the US to have a shorter average life expectancy and higher
infant mortality even with equal healthcare provided. The US population
is 12.2% African Americans and 16.3% Hispanic Americans (2010 Census),
whereas Canada has only 2.5% African Canadians and 0.97% Hispanic
Canadians (2006 Census). African Americans have higher mortality rates
than any other racial or ethnic group for eight of the top ten causes of
death. The cancer incidence rate among African Americans is 10% higher than among European Americans. U.S. Latinos have higher rates of death from diabetes, liver disease, and infectious diseases than do non-Latinos. Adult African Americans and Latinos have approximately twice the risk as European Americans of developing diabetes. The infant mortality rates for African Americans is twice that of whites.
Unfortunately, directly comparing infant mortality rates between
countries is difficult, as countries have different definitions of what
qualifies as an infant death.
Another issue with comparing the two systems is the baseline
health of the patient's for which the systems must treat. Canada has
only half the obesity rate that the US system must deal with (14.3% vs
30.6%). On average, obesity reduces life expectancy by 6–7 years.
A 2004 study found that Canada had a slightly higher mortality rate for acute myocardial infarction (heart attack) because of the more conservative Canadian approach to revascularizing (opening) coronary arteries.
Cancer
Numerous
studies have attempted to compare the rates of cancer incidence and
mortality in Canada and the U.S., with varying results. Doctors who
study cancer epidemiology warn that the diagnosis of cancer is
subjective, and the reported incidence of a cancer will rise if screening is more aggressive, even if the real
cancer incidence is the same. Statistics from different sources may
not be compatible if they were collected in different ways. The proper
interpretation of cancer statistics has been an important issue for many
years. Dr. Barry Kramer of the National Institutes of Health
points to the fact that cancer incidence rose sharply over the past few
decades as screening became more common. He attributes the rise to
increased detection of benign early stage cancers that pose little risk
of metastasizing.
Furthermore, though patients who were treated for these benign cancers
were at little risk, they often have trouble finding health insurance
after the fact.
Cancer survival time increases with later years of diagnosis,
because cancer treatment improves, so cancer survival statistics can
only be compared for cohorts in the same diagnosis year. For example, as
doctors in British Columbia adopted new treatments, survival time for
patients with metastatic breast cancer increased from 438 days for those
diagnosed in 1991–1992, to 667 days for those diagnosed in 1999–2001.
An assessment by Health Canada found that cancer mortality rates are almost identical in the two countries.
Another international comparison by the National Cancer Institute of
Canada indicated that incidence rates for most, but not all, cancers
were higher in the U.S. than in Canada during the period studied
(1993–1997). Incidence rates for certain types, such as colorectal and
stomach cancer, were actually higher in Canada than in the U.S.
In 2004, researchers published a study comparing health outcomes in the
Anglo countries. Their analysis indicates that Canada has greater
survival rates for both colorectal cancer and childhood leukemia, while
the United States has greater survival rates for Non-Hodgkin's lymphoma
as well as breast and cervical cancer.
A study based on data from 1978 through 1986 found very similar survival rates in both the United States and in Canada. However, a study based on data from 1993 through 1997 found lower cancer survival rates among Canadians than among Americans.
A few comparative studies have found that cancer survival rates
vary more widely among different populations in the U.S. than they do in
Canada. Mackillop and colleagues compared cancer survival rates in
Ontario and the U.S. They found that cancer survival was more strongly
correlated with socio-economic class in the U.S. than in Ontario.
Furthermore, they found that the American survival advantage in the four
highest quintiles was statistically significant. They strongly
suspected that the difference due to prostate cancer was a result of
greater detection of asymptomatic cases in the U.S. Their data
indicates that neglecting the prostate cancer data reduces the American
advantage in the four highest quintiles and gives Canada a statistically
significant advantage in the lowest quintile. Similarly, they believe
differences in screening mammography may explain part of the American
advantage in breast cancer. Exclusion of breast and prostate cancer
data results in very similar survival rates for both countries.
Hsing et al. found that prostate cancer mortality incidence rate
ratios were lower among U.S. whites than among any of the nationalities
included in their study, including Canadians. U.S. African Americans in
the study had lower rates than any group except for Canadians and U.S.
whites.
Echoing the concerns of Dr. Kramer and Professor Mackillop, Hsing later
wrote that reported prostate cancer incidence depends on screening.
Among whites in the U.S., the death rate for prostate cancer remained
constant, even though the incidence increased, so the additional
reported prostate cancers did not represent an increase in real prostate
cancers, said Hsing. Similarly, the death rates from prostate cancer in
the U.S. increased during the 1980s and peaked in early 1990. This is
at least partially due to "attribution bias" on death certificates,
where doctors are more likely to ascribe a death to prostate cancer than
to other diseases that affected the patient, because of greater
awareness of prostate cancer or other reasons.
Because health status is "considerably affected" by socioeconomic
and demographic characteristics, such as level of education and income,
"the value of comparisons in isolating the impact of the healthcare
system on outcomes is limited," according to health care analysts. Experts say that the incidence and mortality rates of cancer cannot be combined to calculate survival from cancer.
Nevertheless, researchers have used the ratio of mortality to
incidence rates as one measure of the effectiveness of healthcare. Data for both studies was collected from registries that are members of the North American Association of Central Cancer Registries, an organization dedicated to developing and promoting uniform data standards for cancer registration in North America.
Racial and ethnic differences
The
U.S. and Canada differ substantially in their demographics, and these
differences may contribute to differences in health outcomes between the
two nations. Although both countries have white majorities, Canada has a proportionately larger immigrant minority population. Furthermore, the relative size of different ethnic and racial groups vary widely in each country. Hispanics and peoples of African descent constitute a much larger proportion of the U.S. population. Non-Hispanic North American aboriginal peoples constitute a much larger proportion of the Canadian population. Canada also has a proportionally larger South Asian and East Asian population. Also, the proportion of each population that is immigrant is higher in Canada.
A study comparing aboriginal mortality rates in Canada, the U.S.
and New Zealand found that aboriginals in all three countries had
greater mortality rates and shorter life expectancies than the white
majorities.
That study also found that aboriginals in Canada had both shorter life
expectancies and greater infant mortality rates than aboriginals in the
United States and New Zealand. The health outcome differences between
aboriginals and whites in Canada was also larger than in the United
States.
Though few studies have been published concerning the health of Black Canadians, health disparities between whites and African Americans in the U.S. have received intense scrutiny.
African Americans in the U.S. have significantly greater rates of
cancer incidence and mortality. Drs. Singh and Yu found that neonatal
and postnatal mortality rates for American African Americans are more
than double the non-Hispanic white rate.
This difference persisted even after controlling for household income
and was greatest in the highest income quintile. A Canadian study also
found differences in neonatal mortality between different racial and
ethnic groups.
Although Canadians of African descent had a greater mortality rate
than whites in that study, the rate was somewhat less than double the
white rate.
The racially heterogeneous Hispanic population in the U.S. has
also been the subject of several studies. Although members of this
group are significantly more likely to live in poverty than are
non-Hispanic whites, they often have disease rates that are comparable
to or better than the non-Hispanic white majority. Hispanics have lower
cancer incidence and mortality, lower infant mortality, and lower rates
of neural tube defects.
Singh and Yu found that infant mortality among Hispanic sub-groups
varied with the racial composition of that group. The mostly white
Cuban population had a neonatal mortality rate (NMR) nearly identical
to that found in non-Hispanic whites and a postnatal mortality rate
(PMR) that was somewhat lower. The largely Mestizo, Mexican, Central, and South American Hispanic populations had somewhat lower NMR and PMR. The Puerto Ricans who have a mix of white and African ancestry had higher NMR and PMR rates.
Impact on economy
This graph depicts gross U.S. health care spending from 1960 to 2008.
In 2002, automotive companies claimed that the universal system in Canada saved labour costs. In 2004, healthcare cost General Motors $5.8 billion, and increased to $7 billion. The UAW also claimed that the resulting escalating healthcare premiums reduced workers' bargaining powers.
Flexibility
In Canada, increasing demands for healthcare, due to the aging population, must be met by either increasing taxes or reducing other government programs. In the United States, under the current system, more of the burden will be taken up by the private sector and individuals.
Since 1998, Canada's successive multibillion-dollar budget
surpluses have allowed a significant injection of new funding to the
healthcare system, with the stated goal of reducing waiting times for
treatment. However, this may be hampered by the return to deficit spending as of the 2009 Canadian federal budget.
One historical problem with the U.S. system was known as job lock,
in which people become tied to their jobs for fear of losing their
health insurance. This reduces the flexibility of the labor market. Federal legislation passed since the mid-1980s, particularly COBRA and HIPAA, has been aimed at reducing job lock. However, providers of group health insurance in many states are permitted to use experience rating
and it remains legal in the United States for prospective employers to
investigate a job candidate's health and past health claims as part of a
hiring decision. Someone who has recently been diagnosed with cancer, for example, may face job lock
not out of fear of losing their health insurance, but based on
prospective employers not wanting to add the cost of treating that
illness to their own health insurance pool, for fear of future insurance
rate increases. Thus, being diagnosed with an illness can cause someone
to be forced to stay in their current job.
Politics of health
Politics of each country
More imaginative solutions in both countries have come from the sub-national level.
Canada
In Canada, the right-wing and now defunct Reform Party and its successor, the Conservative Party of Canada
considered increasing the role of the private sector in the Canadian
system. Public backlash caused these plans to be abandoned, and the
Conservative government that followed re-affirmed its commitment to
universal public medicine.
In Canada, it was Alberta
under the Conservative government that had experimented most with
increasing the role of the private sector in healthcare. Measures
included the introduction of private clinics allowed to bill patients
for some of the cost of a procedure, as well as 'boutique' clinics
offering tailored personal care for a fixed preliminary annual fee.
United States
In the U.S., President Bill Clinton attempted a significant restructuring of health care, but the effort collapsed under political pressure against it despite tremendous public support. The 2000 U.S. election saw prescription drugs become a central issue, although the system did not fundamentally change. In the 2004 U.S. election healthcare proved to be an important issue to some voters, though not a primary one.
In 2006, Massachusetts adopted a plan
that vastly reduced the number of uninsured making it the state with
the lowest percentage of non-insured residents in the union. It requires
everyone to buy insurance and subsidizes insurance costs for lower
income people on a sliding scale. Some have claimed that the state's program is unaffordable, which the state itself says is "a commonly repeated myth".
In 2009, in a minor amendment, the plan did eliminate dental, hospice
and skilled nursing care for certain categories of noncitizens covering
30,000 people (victims of human trafficking and domestic violence,
applicants for asylum and refugees) who do pay taxes.
In July 2009, Connecticut passed into law a plan called SustiNet, with the goal of achieving health care coverage of 98% of its residents by 2014.
US President Donald Trump has declared his intent to repeal the Affordable Care Act, but has failed to do so, thus far.
Private care
The
Canada Health Act of 1984 "does not directly bar private delivery or
private insurance for publicly insured services," but provides financial
disincentives for doing so. "Although there are laws prohibiting or
curtailing private health care in some provinces, they can be changed,"
according to a report in the New England Journal of Medicine.
Governments attempt to control health care costs by being the sole
purchasers and thus they do not allow private patients to bid up prices.
Those with non-emergency illnesses such as cancer cannot pay out of
pocket for time-sensitive surgeries and must wait their turn on waiting
lists. According to the Canadian Supreme Court in its 2005 ruling in Chaoulli v. Quebec, waiting list delays "increase the patient's risk of mortality or the risk that his or her injuries will become irreparable."
The ruling found that a Quebec provincial ban on private health
insurance was unlawful, because it was contrary to Quebec's own
legislative act, the 1975 Charter of Human Rights and Freedoms.
Consumer-driven healthcare
In the United States, Congress has enacted laws to promote consumer-driven healthcare with health savings accounts (HSAs), which were created by the Medicare bill signed by President George W. Bush on December 8, 2003. HSAs are designed to provide tax incentives
for individuals to save for future qualified medical and retiree health
expenses. Money placed in such accounts is tax-free. To qualify for
HSAs, individuals must carry a high-deductible health plan (HDHP). The higher deductible
shifts some of the financial responsibility for health care from
insurance providers to the consumer. This shift towards a market-based
system with greater individual responsibility increased the differences
between the US and Canadian systems.
Some economists who have studied proposals for universal
healthcare worry that the consumer driven healthcare movement will
reduce the social redistributive effects of insurance that pools
high-risk and low-risk people together. This concern was one of the
driving factors behind a provision of the Patient Protection and Affordable Care Act, informally known as Obamacare,
which limited the types of purchases which could be made with HSA
funds. For example, as of January 1, 2011, these funds can no longer be
used to buy over-the-counter drugs without a medical prescription.