Slow-wave sleep (SWS), often referred to as deep sleep, consists of stage three of non-rapid eye movement sleep. Initially, SWS consisted of both Stage 3, which has 20–50 percent delta wave activity, and Stage 4, which has more than 50 percent delta wave activity.
Overview
This period of sleep is called slow-wave sleep because the EEG activity is synchronized, producing slow waves with a frequency range of 0.5–2 Hz
and peak-to-peak amplitude greater than 75µV. The first section of the
wave signifies a "down state", which is an inhibition or hyperpolarizing
phase in which the neurons in the neocortex
are silent. This is the period when the neocortical neurons are able to
rest. The second section of the wave signifies an "up state", which is
an excitation or depolarizing phase in which the neurons fire briefly at
a high rate. The principal characteristics during slow-wave sleep that
contrast with REM sleep are moderate muscle tone, slow or absent eye movement, and lack of genital activity.
Slow-wave sleep is considered important for memory consolidation. This is sometimes referred to as "sleep-dependent memory processing".
Impaired memory consolidation has been seen in individuals with primary
insomnia who thus do not perform as well as those who are healthy in
memory tasks following a period of sleep.
Furthermore, slow-wave sleep improves declarative memory (which
includes semantic and episodic memory). A central model has been
hypothesized that the long-term memory storage is facilitated by an
interaction between the hippocampal and neocortical networks. In several studies, after the subjects have had training to learn a declarative memory task, the density of human sleep spindles
present was significantly higher than the signals observed during the
control tasks that involved similar visual stimulation and
cognitively-demanding tasks but did not require learning.
This associated with the spontaneously occurring wave oscillations that
account for the intracellular recordings from thalamic and cortical
neurons.
Specifically, SWS presents a role in spatial declarative memory. Reactivation of the hippocampus during SWS is detected after the spatial learning task. In addition, a correlation can be observed between the amplitude of hippocampal activity during SWS and the improvement in spatial memory performance, such as route retrieval, on the following day.
A memory reactivation experiment during SWS was conducted using
odor as a cue, given that it does not disturb ongoing sleep, over a
prior learning task and sleep sessions. The region of the hippocampus
was activated in response to odor re-exposure during SWS. This stage of
sleep has an exclusive role as a context cue that reactivates the
memories and favors their consolidation.
A further study demonstrated that when subjects heard sounds associated
with previously shown pictures-locations, the reactivation of
individual memory representations was significantly higher during SWS
compared to other sleep stages.
Affective representations are generally better remembered during
sleep compared to neutral ones. Emotions with negative salience
presented as a cue during SWS show better reactivation, therefore an
enhanced consolidation in comparison to neutral memories. The former was
predicted by sleep spindles over SWS, which discriminates the memory processes during sleep as well as facilitating emotional memory consolidation.
Acetylcholine
plays an essential role in hippocampus-dependent memory consolidation.
An increased level of cholinergic activity during SWS is known to be
disruptive for memory processing. Considered that acetylcholine is a
neurotransmitter that modulates the direction of information flow
between the hippocampus and neocortex during sleep, its suppression is
necessary during SWS in order to consolidate sleep-related declarative
memory.
Sleep deprivation studies with humans suggest that the primary
function of slow-wave sleep may be to allow the brain to recover from
its daily activities. Glucose metabolism in the brain increases as a
result of tasks that demand mental activity. Another function affected by slow-wave sleep is the secretion of growth hormone, which is always greatest during this stage. It is also thought to be responsible for a decrease in sympathetic and increase in parasympathetic neural activity.
Prior to 2007 the American Academy of Sleep Medicine (AASM) divided Slow-wave sleep into stages 3 and 4.
The two stages are now combined as "Stage three" or N3. An epoch (30
seconds of sleep) which consists of 20% or more slow-wave (delta) sleep
is now considered to be stage three.
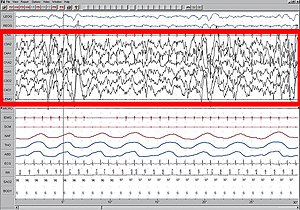
Electroencephalographic characteristics
Polysomnogram demonstrating SWS, stage four.
High amplitude EEG is highlighted in red.
Large 75-microvolt (0.5–2.0 Hz) delta waves predominate the electroencephalogram (EEG). Stage N3 is defined by the presence of 20% delta waves in any given 30-second epoch of the EEG during sleep, by the current 2007 AASM guidelines.
Longer periods of SWS occur in the first part of the night,
primarily in the first two sleep cycles (roughly three hours). Children
and young adults will have more total SWS in a night than older adults.
The elderly may not go into SWS at all during many nights of sleep.
Slow-wave sleep is an active phenomenon probably brought about by the activation of serotonergic neurons of the raphe system.
The slow-wave seen in the cortical EEG is generated through thalamocortical communication through the thalamocortical neurons. In the TC neurons this is generated by the "slow oscillation" and is dependent on membrane potential bistability,
a property of these neurons due to an electrophysiological component
known as "I t window". "I t window" is due to the overlap underneath
activation and inactivation curves if plotted for T-type calcium
channels (inward current). If these two curves are multiplied, and
another line superimposed on the graph to show a small Ik leak current
(outward), then the interplay between these inward (I t window) and
outward (small Ik leak), three equilibrium points
are seen at −90, −70 and −60 mv, −90 and −60 being stable and −70
unstable. This property allows the generation of slow waves due to an
oscillation between two stable points. It is important to note that in in vitro, mGluR must be activated on these neurons to allow a small Ik leak, as seen in in vivo situations.
Functions
Hemispheric asymmetries in the human sleep
Slow-wave
sleep is necessary for survival. Some animals, such as dolphins and
birds, have the ability to sleep with only one hemisphere of the brain,
leaving the other hemisphere awake to carry out normal functions and to
remain alert. This kind of sleep is called unihemispheric slow-wave sleep
and it is also partially observable in human beings. Indeed, a study
reported a unilateral activation of the somatosensorial cortex when a
vibrating stimulus was put on the hand of human subjects. The recordings
show an important inter-hemispheric change during the first hour of
non-REM sleep and consequently the presence of a local and use-dependent
aspect of sleep. Another experiment detected a greater number of delta waves in the frontal and central regions of the right hemisphere.
Considering that SWS is the only sleep stage that reports human
deep sleep as well as being used in studies with mammals and birds, it
is also adopted in experiments revealing the role of hemispheric
asymmetries during sleep. A predominance of the left hemisphere in the
neural activity can be observed in the default-mode network during SWS.
This asymmetry is correlated with the sleep-onset-latency, which is a
sensitive parameter of the so-called first night effect, in other words
of the reduced quality of sleep during the first session in the
laboratory.
The left hemisphere is shown to be more sensitive to deviant
stimuli during the first night compared to the following nights of an
experiment. This asymmetry explains further the reduced sleep of half
the brain during SWS. Indeed, in comparison to the right one, the left
hemisphere plays a vigilant role during SWS.
Furthermore, a faster behavioral reactivity is detected in the
left hemisphere during SWS of the first night. The rapid awakening is
correlated to the regional asymmetry in the activities of SWS. These
findings show that the hemispheric asymmetry in SWS plays a role as a
protective mechanism. SWS is therefore sensitive to danger and
non-familiar environment, creating a need for vigilance and reactivity
during sleep.
Neural control of slow-wave sleep
Several
neurotransmitters are involved in sleep and waking patterns:
acetylcholine, norepinephrine, serotonin, histamine, and orexin.
Neocortical neurons fire spontaneously during slow-wave sleep, thus
they seem to play a role during this period of sleep. Also, these
neurons appear to have some sort of internal dialogue, which accounts
for the mental activity during this state where there is no information
from external signals because of the synaptic inhibition at the thalamic
level. The rate of recall of dreams during this state of sleep is
relatively high compared to the other levels of the sleep cycle. This
indicates that mental activity is closer to real life events.
Physical healing and growth
Slow-wave
sleep is the constructive phase of sleep for recuperation of the
mind-body system in which it rebuilds itself after each day. Substances
that have been ingested into the body while an organism is awake are
synthesized into complex proteins of living tissue. Growth hormones are
also secreted to facilitate the healing of muscles as well as repairing
damage to any tissues. Lastly, glial cells within the brain are restored with sugars to provide energy for the brain.
Learning and synaptic homeostasis
Learning and memory formation occurs during wakefulness by the process of long-term potentiation;
SWS is associated with the regulation of synapses thus potentiated. SWS
has been found to be involved in the downscaling of synapses, in which
strongly stimulated or potentiated synapses are kept while weakly
potentiated synapses either diminish or are removed. This may be helpful for recalibrating synapses for the next potentiation during wakefulness and for maintaining synaptic plasticity. Notably, new evidence is showing that reactivation and rescaling may be co-occurring during sleep.
Problems associated with slow-wave sleep
Bedwetting, night terrors, and sleepwalking
are all common behaviors that can occur during stage three of sleep.
These occur most frequently amongst children, who then generally outgrow
them.
Another problem that may arise is sleep-related eating disorder. An
individual will sleep-walk leaving his or her bed in the middle of the
night seeking out food, and will eat not having any memory of the event
in the morning. Over half of individuals with this disorder become overweight.
Sleep-related eating disorder can usually be treated with dopaminergic
agonists, or topiramate, which is an anti-seizure medication. This
nocturnal eating throughout a family suggests that heredity may be a
potential cause of this disorder.
Effects of sleep deprivation
J. A. Horne (1978) reviewed several experiments with humans and
concluded that sleep deprivation has no effects on people’s
physiological stress response or ability to perform physical exercise.
It did, however, have an effect on cognitive functions. Some people
reported distorted perceptions or hallucinations and lack of
concentration on mental tasks. Thus, the major role of sleep does not
appear to be rest for the body, but rest for the brain.
When sleep-deprived humans sleep normally again, the recovery
percentage for each stage of sleep is not the same. Only seven percent
of stages one and two are regained, but 68 percent of stage-four
slow-wave sleep and 53 percent of REM sleep are regained. This suggests
that stage-four sleep (known today as the deepest part of stage-three
sleep) is more important than the other stages.
During slow-wave sleep, there is a significant decline in
cerebral metabolic rate and cerebral blood flow. The activity falls to
about 75 percent of the normal wakefulness level. The regions of the
brain that are most active when awake have the highest level of delta
waves during slow-wave sleep. This indicates rest is geographical. The
“shutting down” of the brain accounts for the grogginess and confusion
if someone is awakened during deep sleep since it takes the cerebral
cortex time to resume its normal functions.
According to J. Siegel (2005), sleep deprivation results in the build-up of free radicals and superoxides
in the brain. Free radicals are oxidizing agents that have one unpaired
electron, making them highly reactive. These free radicals interact
with electrons of biomolecules and damage cells. In slow-wave sleep, the
decreased rate of metabolism reduces the creation of oxygen byproducts,
thereby allowing the existing radical species to clear. This is a means
of preventing damage to the brain.
Amyloid-beta pathology
The accumulation of Amyloid beta
(Aβ) in the prefrontal cortex is associated with the disruption or
reduction of slow waves of NREM sleep. Therefore, this may reduce the
ability for memory consolidation in older adults.
Individual differences
Though
SWS is fairly consistent within the individual, it can vary across
individuals. Age and gender have been noted as two of the biggest
factors that affect this period of sleep. Aging is inversely
proportional to the amount of SWS beginning by midlife and therefore,
SWS declines with age. Sex differences have also been found, such that
females tend to have higher levels of SWS compared to males, at least up
until menopause. There have also been studies that have shown
differences between races. The results showed that there was a lower
percentage of SWS in African Americans compared to Caucasians, but since
there are many influencing factors (e.g. body mass index,
sleep-disordered breathing, obesity, diabetes, and hypertension) this
potential difference must be investigated further.
Mental disorders play a role in individual differences in the quality and quantity of SWS: subjects suffering from depression
show a lower amplitude of slow-wave activity compared to healthy
participants. Sex differences also persist in the former group:
depressed men present significantly lower SWA amplitude. This sex
divergence is twice as large as the one observed in healthy subjects.
However, no age-related difference concerning SWS can be observed in the
depressed group.
Brain regions
Some of the brain regions implicated in the induction of slow-wave sleep include:
- the parafacial zone (GABAergic neurons), located within the medulla oblongata
- the nucleus accumbens core (GABAergic medium spiny neurons; specifically, the subset of these neurons that expresses both D2-type dopamine receptors and adenosine A2A receptors), located within the striatum
- the ventrolateral preoptic area (GABAergic neurons), located within the hypothalamus
- the lateral hypothalamus (melanin-concentrating hormone-releasing neurons), located within the hypothalamus
Drugs
The chemical gamma-hydroxybutyric acid (GHB) has been studied to increase SWS. In the United States, the Food and Drug Administration (FDA) permits the use of GHB under the trade name Xyrem to reduce cataplexy attacks and excessive daytime sleepiness in patients with narcolepsy.
Trazodone
is also being investigated in connection with improving non-REM
slow-wave sleep, and related reductions in Alzheimer's-related buildup
of amyloid and tau.