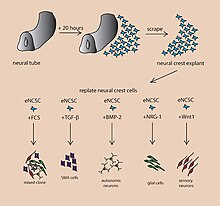
A cerebral organoid describes artificially grown, in vitro, miniature organs resembling the brain. Cerebral organoids are created by culturing human pluripotent stem cells in a three-dimensional rotational bioreactor and develop over a course of months.[1] The human brain is an extremely complex system of heterogeneous tissues and consists of an extremely diverse array of neurons. This complexity has made studying the brain and understanding how it works a difficult task in neuroscience, especially when it comes to neurodegenerative diseases. The purpose of creating an in vitro neurological model is to study these diseases in a more simple and variable space; free of in vivo limitations, especially when working with humans. The varying physiology between human and other mammalian models limits the scope of study in neurological disorders. Cerebral organoids are synthesized tissues that contain several types of nerve cells and have anatomical features that resemble mammalian brains. Cerebral organoids are most similar to layers of neurons called the cortex and choroid plexus. In some cases, structures similar to the retina, meninges and hippocampus can form.[1][2] Stem cells have the potential to grow into many different types of tissues and their fate is dependent on many factors. Below is an image showing some of the chemical factors that can lead stem cells to differentiate into various neural tissues. Similar techniques are used on stem cells used to grow cerebral organoids.[3]
Instructive growth factors regulating fate decisions in embryonic NCCs.
Model development
Using human pluripotent stem cells to create in vitro cerebral organoids allows researchers to summarize current developmental mechanisms for human neural tissue as well as study the roots of human neurological diseases. Cerebral organoids are an investigative tool, used to understand how disease pathology works. These organoids can be used in experiments that current in vitro methods are too simple for, while also being more human applicable than rodent or other mammalian models. Historically, major breakthroughs in how the brain works have resulted from injury or disorder in human brain function, leading to understanding of how regions of the brain work. An in vitro human brain model would allow for the next wave in understanding of the human brain.[1][3]Applications
In addition to being used as tools to study disease pathology and treatments, future application of cerebral organoids include direct implantation into a host, like a human being. The organoid can fuse with host tissue in areas of neurodegeneration, being incorporated with the host vasculature and be immunologically silent.[4] A list of potential applications for cerebral organoids is highlighted below.Potential applications
-
- Tissue morphogenesis with respect to cerebral organoids covers how neural organs form in vertebrates. Cerebral organoids can serve as in vitro tools to study the formation, modulate it, and further understand the mechanisms controlling it.[5]
- Migration Assays
-
- Cerebral organoids can help to study cell migration. Neural glial cells cover a wide variety of neural cells, some of which move around the neurons. The factors that govern their movements can be studied using cerebral organoids.[3]
- Clonal lineage tracing
- Clonal lineage tracing is part of fate mapping, where the lineage of differentiated tissues is traced to the pluripotent progenitors. The local stimuli released and mechanism of differentiation can be studied using cerebral organoids as a model.[5]
- Transplantation
-
- Cerebral organoids can be used to grow specific brain regions and transplant them into regions of neurodegeneration as a therapeutic treatment.
- Cell fate potential
- Cross species developmental timing
-
- Cerebral organoids provide a unique insight into the timing of development of neural tissues and can be used as a tool to study the differences across species.[5]
-
- Cerebral organoids can be used as simple models of complex brain tissues to study the effects of drugs and to screen them for initial safety and efficacy.
- Cell replacement therapy
-
- Cerebral organoids can be used as a simple model to show how cell replacement therapy would work on brain tissues.[5]
- Cell-type specific genome assays
Disease
Organoids can be used to study the crucial early stages of brain development, test drugs and, because they can be made from living cells, study individual patients.,[2] In one case, a cerebral organoid grown from a patient with microcephaly demonstrated related symptoms and revealed that apparently the cause is overly rapid development, followed by slower brain growth. Microencephaly is a developmental condition in which the brain remains undersized, producing an undersized head and debilitation. Microcephaly is not suitable for mouse models, which do not replicate the condition.[2] The primary form of the disease is thought to be caused by a homozygous mutation in the microcephalin gene. The disease is difficult to reproduce in mouse models because mice lack the developmental stages for an enlarged cerebral cortex that humans have. Naturally, a disease which affects this development would be impossible to show in a model which does not have it to begin with.[6] To use cerebral organoids to model a human's microcephaly, one group of researchers has taken patient skin fibroblasts and reprogrammed them using four well known reprogramming factors. These include OCT4, SOX2, MYC and KLF4. The reprogrammed sample was able to be cloned into induced pluripotent stem cells. The cells were cultured into a cerebral organoid following a process described in the cerebral organoid creation section below. The organoid that resulted had decreased numbers of neural progenitor cells and smaller tissues. Additionally, the patient derived tissues displayed fewer and less frequent neuroepithelial tissues made of progenitors, decreased radial glial stem cells, and increased neurons. These results suggest that the underlying mechanism of microcephaly is caused by cells prematurely differentiating into neurons leaving a deficit of radial glial cells.[1]Construction
To make an organoid, an embryoid (tissue that has some embryonic features) grown from natural stem cells is used. Embryos have three layers: endoderm, mesoderm and ectoderm. Each turns into various body parts. The nervous system grows from the ectoderm (which also contributes dental enamel and the epidermis).[3] Ectodermal cells were placed into gel droplets and floated in a nutrient broth in a rotating bioreactor, which supported cell growth without forming by the container. After ten days the organoid developed neurons. After 30 days it displayed regions similar to parts of brains. Lacking a blood supply, cerebral organoids reach about 4 mm across and can last a year or more.[2] The general procedure can be broken down into 5 steps. First human pluripotent stem cells are cultured. They are then allowed to cultivate into an embryoid body. Next the cell culture is induced to form a neuroectoderm. The neuroectoderm is then grown in a matrigel droplet. The matrigel provides nutrients and the neuroectoderm starts to proliferate and grow. However, the lack of vasculature limits the size the organoid can grow. This has been the major limitation in organoid development, however new methods using a spinning bioreactor have allowed an increase in the availability of nutrients to cells inside the organoid. This last step has been the key breakthrough in organoid development.[7] Spinning bioreactors have been used increasingly in cell culture and tissue growth applications. The reactor is able to deliver faster cell doubling times, increased cell expansion and increased extra-cellular matrix components when compared to statically cultured cells.[8]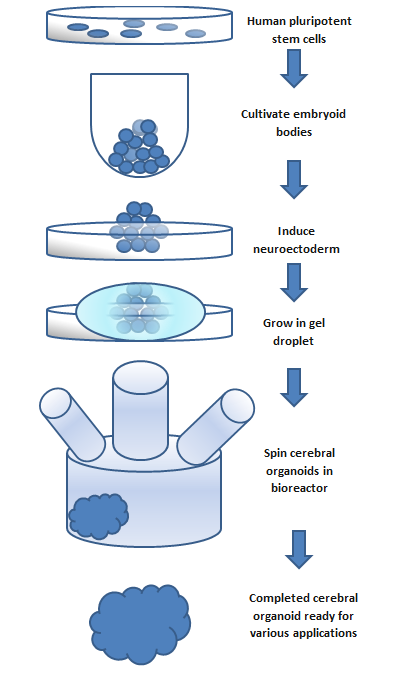
Figure: This flow chart outlines the
basic steps to create a cerebral
organoid. The process takes a span
of months and the size of the
organoid is limited to the
availability of nutrients. Newer
methods allow development of
cerebrovascular organoids,[9] and
micro pumps to provide circulation
through them are being developed,
as explained in this video by
Dr George M. Church.