| African trypanosomiasis | |
|---|---|
| Other names | Sleeping sickness, African sleeping sickness |
 | |
| Trypanosoma forms in a blood smear | |
| Specialty | Infectious disease |
| Symptoms | Stage 1: Fevers, headaches, itchiness, joint pains Stage 2: Trouble sleeping, confusion, poor coordination |
| Usual onset | 1–3 weeks post exposure |
| Causes | Trypanosoma brucei spread by tsetse flies |
| Diagnostic method | Blood smear, lumbar puncture |
| Medication | Pentamidine, suramin, eflornithine |
| Prognosis | Fatal without treatment |
| Frequency | 11,000 |
| Deaths | 3,500 |
African trypanosomiasis, also known as African sleeping sickness or simply sleeping sickness, is an insect-borne parasitic disease of humans and other animals. It is caused by protozoa of the species Trypanosoma brucei. Humans are infected by two types, Trypanosoma brucei gambiense (TbG) and Trypanosoma brucei rhodesiense (TbR). TbG causes over 98% of reported cases. Both are usually transmitted by the bite of an infected tsetse fly and are most common in rural areas.
Initially, the first stage of the disease is characterized by fevers, headaches, itchiness, and joint pains, beginning one to three weeks after the bite. Weeks to months later the second stage begins with confusion, poor coordination, numbness, and trouble sleeping. Diagnosis is by finding the parasite in a blood smear or in the fluid of a lymph node. A lumbar puncture is often needed to tell the difference between first and second stage disease.
Prevention of severe disease involves screening the population at risk with blood tests for TbG. Treatment is easier when the disease is detected early and before neurological symptoms occur. Treatment of the first stage is with the medications pentamidine or suramin. Treatment of the second stage involves eflornithine or a combination of nifurtimox and eflornithine for TbG. While melarsoprol works for both stages, it is typically only used for TbR, due to serious side effects. Without treatment sleeping sickness typically results in death.
The disease occurs regularly in some regions of sub-Saharan Africa with the population at risk being about 70 million in 36 countries. An estimated 11,000 people are currently infected with 2,800 new infections in 2015. In 2015 it caused around 3,500 deaths, down from 34,000 in 1990. More than 80% of these cases are in the Democratic Republic of the Congo. Three major outbreaks have occurred in recent history: one from 1896 to 1906 primarily in Uganda and the Congo Basin and two in 1920 and 1970 in several African countries. It is classified as a neglected tropical disease. Other animals, such as cows, may carry the disease and become infected in which case it is known as animal trypanosomiasis.
Signs and symptoms
African
trypanosomiasis symptoms occur in two stages. The first stage, known as
the hemolymphatic phase, is characterized by fever, headaches, joint
pains, and itching. Fever is intermittent, with attacks lasting from a
day to a week, separated by intervals of a few days to a month or
longer. Invasion of the circulatory and lymphatic systems by the
parasites is associated with severe swelling of lymph nodes, often to tremendous sizes. Winterbottom's sign, the tell-tale swollen lymph nodes along the back of the neck, may appear. Occasionally, a chancre
(red sore) will develop at the location of the tsetse fly bite. If left
untreated, the disease overcomes the host's defenses and can cause more
extensive damage, broadening symptoms to include anemia, endocrine, cardiac, and kidney dysfunctions.
The second phase of the disease, the neurological phase, begins when the parasite invades the central nervous system by passing through the blood–brain barrier.
Disruption of the sleep cycle is a leading symptom of this stage and is
the one that gave the disease the name 'sleeping sickness.' Infected
individuals experience a disorganized and fragmented 24-hour rhythm of
the sleep-wake cycle, resulting in daytime sleep episodes and nighttime
periods of wakefulness.
Other neurological symptoms include confusion, tremor, general muscle weakness, hemiparesis, and paralysis of a limb. Parkinson-like
movements might arise due to non-specific movement disorders and speech
disorders. Individuals may also exhibit psychiatric symptoms such as
irritability, psychotic reactions, aggressive behaviour, or apathy which can sometimes dominate the clinical diagnosis.
Without treatment, the disease is invariably fatal, with progressive
mental deterioration leading to coma, systemic organ failure, and death.
An untreated infection with T. b. rhodesiense will cause death within months whereas an untreated infection with T. b. gambiense will cause death after several years. Damage caused in the neurological phase is irreversible.
Cause
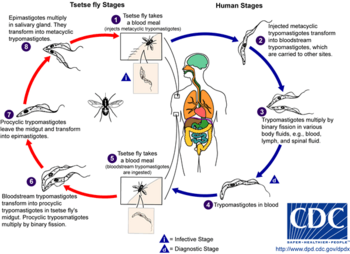
The life cycle of the Trypanosoma brucei parasites.
Trypanosoma brucei gambiense accounts for the majority of
African trypanosomiasis cases, with humans as the main reservoir needed
for the transmission, while Trypanosoma brucei rhodesiense is mainly zoonotic, with the occasional human infection.
African Trypanosomiasis is dependent on the interaction of the parasite
(trypanosome) with the tsetse flies (vector), as well as the host
(human for Trypanosoma brucei gambiense, and animals for Trypanosoma brucei rhodesiense). The risk of contracting African Trypanosomiasis is dependent on coming in contact with an infected tsetse fly.
Trypanosoma brucei
There are two subspecies of the parasite that are responsible for starting the disease in humans. Trypanosoma brucei gambiense causes the diseases in west and central Africa, whereas Trypanosoma brucei rhodesiense
has a limited geographical range and is responsible for causing the
disease in east and southern Africa. In addition, a third subspecies of
the parasite known as Trypanosoma brucei brucei is responsible for affecting animals but not humans.
Humans are the main reservoir for T. b. gambiense but this species can also be found in pigs and other animals. Wild game animals and cattle are the main reservoir of T. b. rhodesiense.
These parasites primarily infect individuals in sub-Saharan Africa
because that is where the vector (tsetse fly) is located. The two human
forms of the disease also vary greatly in intensity. T. b. gambiense causes a chronic condition
that can remain in a passive phase for months or years before symptoms
emerge and the infection can last about 3 years before death occurs.
T. b. rhodesiense is the acute
form of the disease, and death can occur within months since the
symptoms emerge within weeks and it is more virulent and faster
developing than T. b. gambiense. Furthermore, trypanosomes are surrounded by a coat that is composed of variant surface glycoproteins
(VSG). These proteins act to protect the parasite from any lytic
factors that are present in human plasma. The host's immune system
recognizes the glycoproteins present on the coat of the parasite leading
to the production of different antibodies (IgM and IgG).
These antibodies will then act to destroy the parasites that
circulate around the blood. However, from the several parasites present
in the plasma, a small number of them will experience changes in their
surface coats resulting in the formation of new VSGs. Thus, the
antibodies produced by the immune system will no longer recognize the
parasite leading to proliferation until new antibodies are created to
combat the novel VSGs. Eventually the immune system will no longer be
able to fight off the parasite due to the constant changes in VSGs and
infection will arise.
Vector
The tsetse fly (genus Glossina) is a large, brown, biting fly that serves as both a host and vector for the trypanosome
parasites. While taking blood from a mammalian host, an infected tsetse
fly injects metacyclic trypomastigotes into skin tissue. From the bite,
parasites first enter the lymphatic system and then pass into the
bloodstream. Inside the mammalian host, they transform into bloodstream
trypomastigotes, and are carried to other sites throughout the body,
reach other body fluids (e.g., lymph, spinal fluid), and continue to
replicate by binary fission.
The entire life cycle of African trypanosomes is represented by
extracellular stages. A tsetse fly becomes infected with bloodstream
trypomastigotes when taking a blood meal on an infected mammalian host.
In the fly's midgut, the parasites transform into procyclic
trypomastigotes, multiply by binary fission, leave the midgut, and
transform into epimastigotes. The epimastigotes reach the fly's salivary
glands and continue multiplication by binary fission.
The entire life cycle of the fly takes about three weeks. In addition to the bite of the tsetse fly, the disease can be transmitted by:
- Mother-to-child infection: the trypanosome can sometimes cross the placenta and infect the fetus.
- Laboratories: accidental infections, for example, through the handling of blood of an infected person and organ transplantation, although this is uncommon.
- Blood transfusion
- Sexual contact (This may be possible)
Horse-flies (Tabanidae) and stable flies (Muscidae) possibly play a role in transmission of nagana (the animal form of sleeping sickness) and the human disease form.
| Sleeping sickness | Trypanosoma | Distribution | Vector |
|---|---|---|---|
| Chronic form | T. brucei gambiense | Western Africa | G. palpalis
G. tachinoides
G. fuscipes G. morsitans |
| Acute form | T. brucei rhodesiense | Eastern Africa | G. morsitans
G. swynnertoni
G. pallidipes G. fuscipes |
Mechanism
Tryptophol is a chemical compound that induces sleep in humans. It is produced by the trypanosomal parasite in sleeping sickness.
Diagnosis
Two areas from a blood smear from a person with African trypanosomiasis, thin blood smear stained with Giemsa:
Typical trypomastigote stages (the only stages found in people), with a
posterior kinetoplast, a centrally located nucleus, an undulating
membrane, and an anterior flagellum. The two Trypanosoma brucei subspecies that cause human trypanosomiasis, T. b. gambiense and T. b. rhodesiense, are indistinguishable morphologically. The trypanosomes' length range is 14 to 33 µm, Source: CDC
The gold standard for diagnosis is identification of trypanosomes in a
sample by microscopic examination. Samples that can be used for
diagnosis include chancre fluid, lymph node aspirates, blood, bone marrow, and, during the neurological stage, cerebrospinal fluid.
Detection of trypanosome-specific antibodies can be used for diagnosis,
but the sensitivity and specificity of these methods are too variable
to be used alone for clinical diagnosis. Further, seroconversion occurs after the onset of clinical symptoms during a T. b. rhodesiense infection, so is of limited diagnostic use.
Trypanosomes can be detected from samples using two different
preparations. A wet preparation can be used to look for the motile
trypanosomes. Alternatively, a fixed (dried) smear can be stained using Giemsa's or Field's
technique and examined under a microscope. Often, the parasite is in
relatively low abundance in the sample, so techniques to concentrate the
parasites can be used prior to microscopic examination. For blood
samples, these include centrifugation followed by examination of the buffy coat;
mini anion-exchange/centrifugation; and the quantitative buffy coat
(QBC) technique. For other samples, such as spinal fluid, concentration
techniques include centrifugation followed by examination of the
sediment.
Three serological tests are also available for detection of the
parasite: the micro-CATT, wb-CATT, and wb-LATEX. The first uses dried
blood, while the other two use whole blood samples. A 2002 study found
the wb-CATT to be the most efficient for diagnosis, while the wb-LATEX
is a better exam for situations where greater sensitivity is required.
Prevention
Currently there are few medically related prevention options for
African Trypanosomiasis (i.e. no vaccine exists for immunity). Although
the risk of infection from a tsetse fly bite is minor (estimated at less
than 0.1%), the use of insect repellants, wearing long-sleeved
clothing, avoiding tsetse-dense areas, implementing bush clearance
methods and wild game culling are the best options to avoid infection
available for local residents of affected areas.
In July 2000, a resolution was passed to form the Pan African
Tsetse and Trypanosomiasis Eradication Campaign (PATTEC). The campaign
works to eradicate the tsetse vector population levels and subsequently
the protozoan disease, by use of insecticide-impregnated targets, fly
traps, insecticide-treated cattle, ultra-low dose aerial/ground spraying
(SAT) of tsetse resting sites and the sterile insect technique (SIT).
The use of SIT in Zanzibar proved effective in eliminating the entire
population of tsetse flies but was expensive and is relatively
impractical to use in many of the endemic countries afflicted with
African trypanosomiasis.
A pilot program in Senegal has reduced the tsetse fly population by as much as 99% by introducing male flies which have been sterilized by exposure to gamma rays.
Regular active surveillance, involving detection and prompt
treatment of new infections, and tsetse fly control is the backbone of
the strategy used to control sleeping sickness. Systematic screening
of at-risk communities is the best approach, because case-by-case
screening is not practical in endemic regions. Systematic screening may
be in the form of mobile clinics or fixed screening centres where teams
travel daily to areas of high infection rates. Such screening efforts
are important because early symptoms are not evident or serious enough
to warrant people with gambiense disease to seek medical attention,
particularly in very remote areas. Also, diagnosis of the disease is
difficult and health workers may not associate such general symptoms
with trypanosomiasis. Systematic screening allows early-stage disease to
be detected and treated before the disease progresses, and removes the
potential human reservoir. A single case of sexual transmission of West African sleeping sickness has been reported.
Treatment
First stage
The current treatment for first-stage disease is intravenous or intramuscular pentamidine for T. b. gambiense or intravenous suramin for T. b. rhodesiense.
Fexinidazole has been approved in the Democratic Republic Congo for T.b. gambiense sleeping sickness. Benefits include that it is taken by mouth and treats both stages of the disease.
Second stage
For T. b. gambiense a regimen involving the combination of nifurtimox and eflornithine, nifurtimox-eflornithine combination treatment (NECT), or eflornithine alone appear to be more effective and result in fewer side effects. These treatments may replace melarsoprol when available with the combination being first line. NECT has the benefit of requiring less injections of eflornithine.
Intravenous melarsoprol was previously the standard treatment for
second-stage (neurological phase) disease and is effective for both
types. Melarsoprol is the only treatment for second stage T. b. rhodesiense; however, it causes death in 5% of people who take it. Resistance to melarsoprol can occur.
Epidemiology
Deaths per 100,000 population due to African trypanosomiasis by country in 2002.
In 2010, it caused around 9,000 deaths, down from 34,000 in 1990. As of 2000, the disability-adjusted life-years (9 to 10 years) lost due to sleeping sickness are 2.0 million. From 2010-2014, there was an estimated 55 million people at risk for gambiense African Trypanosomiasis and over 6 million people at risk for rhodesiense African Trypanosomiasis.
In 2014, the World Health Organization reported 3,797 cases of Human
African Trypanosomiasis when the predicted number of cases were to be
5,000. The number of total reported cases in 2014 is an 86% reduction to
the total number of cases reported in 2000.
The disease has been recorded as occurring in 37 countries, all
in sub-Saharan Africa. It occurs regularly in southeast Uganda and
western Kenya, and killed more than 48,000 Africans in 2008. The Democratic Republic of the Congo is the most affected country in the world, accounting for 75% of the Trypanosoma brucei gambiense cases.
The population at risk being about 69 million with one third of this
number being at a 'very high' to 'moderate' risk and the remaining two
thirds at a 'low' to 'very low' risk.
The number of people being affected by the disease has declined. At
this rate, sleeping sickness elimination is a possibility. The World
Health Organization plans to eradicate sleeping sickness by the year
2020.
Prognosis
If untreated, T. b. gambiense
almost always results in death, with only a few individuals shown in a
long-term 15 year follow-up to have survived after refusing treatment. T. b. rhodesiense, being a more acute and severe form of the disease, is consistently fatal if not treated. Disease progression greatly varies depending on disease form. For individuals which are infected by T. b. gambiense,
which accounts for 98% of all of the reported cases, a person can be
infected for months or even years without signs or symptoms until the
advanced disease stage, where it is too late to be treated successfully.
For individuals affected by T. b. rhodesiense, which accounts
for 2% of all reported cases, symptoms appear within weeks or months of
the infection. Disease progression is rapid and invades the central
nervous system, causing death within a short amount of time.
History
In 1903, David Bruce recognized the tsetse fly as the arthropod vector.
The condition has been present in Africa for thousands of years.
Because of a lack of travel between indigenous people, sleeping
sickness in humans had been limited to isolated pockets. This changed
after Arab slave traders entered central Africa from the east, following the Congo River, bringing parasites along. Gambian sleeping sickness travelled up the Congo River, and then further east.
An Arab writer of the 14th century left the following description
in the case of a sultan of the Mali Kingdom: "His end was to be
overtaken by the sleeping sickness (illat an-nawm) which is a
disease that frequently befalls the inhabitants of these countries
especially their chieftains. Sleep overtakes one of them in such a
manner that it is hardly possible to awake him."
The British naval surgeon John Atkins described the disease on his return from West Africa in 1734:
"The Sleepy Distemper (common among the Negroes) gives no other previous Notice, than a want of Appetite 2 or 3 days before; their sleeps are sound, and Sense and Feeling very little; for pulling, drubbing or whipping will scarce stir up Sense and Power enough to move; and the Moment you cease beating the smart is forgot, and down they fall again into a state of Insensibility, drivling constantly from the Mouth as in deep salivation; breathe slowly, but not unequally nor snort. Young people are more subject to it than the old; and the Judgement generally pronounced is Death, the Prognostik seldom failing. If now and then one of them recovers, he certainly loses the little Reason he had, and turns Ideot..."
In 1901, a devastating epidemic erupted in Uganda, killing more than 250,000 people, including about two-thirds of the population in the affected lakeshore areas. According to The Cambridge History of Africa, "It has been estimated that up to half the people died of sleeping-sickness and smallpox in the lands on either bank of the lower river Congo."
The causative agent and vector were identified in 1903 by David Bruce, and the subspecies of the protozoa were differentiated in 1910. Bruce had earlier shown that T. brucei was the cause of a similar disease in horses and cattle that was transmitted by the tse-tse fly (Glossina morsitans).
The first effective treatment, atoxyl, an arsenic-based drug developed by Paul Ehrlich and Kiyoshi Shiga, was introduced in 1910, but blindness was a serious side effect.
Suramin was first synthesized by Oskar Dressel and Richard Kothe in 1916 for Bayer.
It was introduced in 1920 to treat the first stage of the disease. By
1922, Suramin was generally combined with tryparsamide (another
pentavalent organoarsenic drug), the first drug to enter the nervous
system and be useful in the treatment of the second stage of the
gambiense form. Tryparsamide was announced in the Journal of Experimental Medicine in 1919 and tested in the Belgian Congo by Louise Pearce of the Rockefeller Institute
in 1920. It was used during the grand epidemic in West and Central
Africa on millions of people and was the mainstay of therapy until the
1960s. American medical missionary Arthur Lewis Piper was active in using tryparsamide to treat sleeping sickness in the Belgian Congo in 1925.
Pentamidine, a highly effective drug for the first stage of the disease, has been used since 1937. During the 1950s, it was widely used as a prophylactic
agent in western Africa, leading to a sharp decline in infection rates.
At the time, eradication of the disease was thought to be at hand.
The organoarsenical melarsoprol
(Arsobal) developed in the 1940s is effective for people with
second-stage sleeping sickness. However, 3–10% of those injected have
reactive encephalopathy (convulsions, progressive coma, or psychotic reactions), and 10–70% of such cases result in death; it can cause brain damage in those who survive the encephalopathy. However, due to its effectiveness, melarsoprol
is still used today. Resistance to melarsoprol is increasing, and
combination therapy with nifurtimox is currently under research.
Eflornithine
(difluoromethylornithine or DFMO), the most modern treatment, was
developed in the 1970s by Albert Sjoerdsma and underwent clinical trials
in the 1980s. The drug was approved by the United States Food and Drug Administration in 1990. Aventis, the company responsible for its manufacture, halted production in 1999. In 2001, Aventis, in association with Médecins Sans Frontières and the World Health Organization, signed a long-term agreement to manufacture and donate the drug.
In addition to sleeping sickness, previous names have included
negro lethargy, maladie du sommeil (Fr), Schlafkrankheit (Ger), African
lethargy, and Congo trypanosomiasis.
- The British-led Sleeping Sickness Commission collecting tsetse flies, Uganda and Nyasaland, 1908-1913
Research
The genome of the parasite has been sequenced
and several proteins have been identified as potential targets for drug
treatment. Analysis of the genome also revealed the reason why
generating a vaccine for this disease has been so difficult. T. brucei has over 800 genes that make proteins the parasite "mixes and matches" to evade immune system detection.
Using a genetically modified form of a bacterium that occurs
naturally in the gut of the vectors is being studied as a method of
controlling the disease.
Recent findings indicate that the parasite is unable to survive in the bloodstream without its flagellum. This insight gives researchers a new angle with which to attack the parasite.
Trypanosomiasis vaccines are undergoing research.
Additionally, the Drugs for Neglected Disease Initiative has contributed to the African sleeping sickness research by developing a compound called fexinidazole. This project was originally started in April 2007 and enrolled 749 people in the DRC and Central African Republic.
The results showed efficacy and safety in both stages of the disease,
both in adults and children ≥ 6 years old and weighing ≥ 20 kg. The European Medicines Agency approved it for first and second stage disease outside of Europe in November 2018. The treatment was approved in the DRC in December 2018.
Funding
For current funding statistics, human African trypanosomiasis is grouped with kinetoplastid infections. Kinetoplastids refer to a group of flagellate protozoa.
Kinetoplastid infections include African sleeping sickness, Chagas'
disease, and Leishmaniasis. All together, these three diseases accounted
for 4.4 million disability adjusted life years (DALYs) and an additional 70,075 recorded deaths yearly.
For kinetoplastid infections, the total global research and development
funding was approximately $136.3 million in 2012. Each of the three
diseases, African sleeping sickness, Chagas' disease, and Leishmaniasis
each received approximately a third of the funding, which was about
$36.8 million US dollars, $38.7 million US dollars, and $31.7 million US
dollars, respectively.
For sleeping sickness, funding was split into basic research,
drug discovery, vaccines, and diagnostics. The greatest amount of
funding was directed towards basic research of the disease;
approximately $21.6 million US dollars was directed towards that effort.
As for therapeutic development, approximately $10.9 million was
invested.
The top funder for kinetoplastid infection research and
development are public sources. About 62% of the funding comes from
high-income countries while 9% comes from low- and middle-income
countries. High-income countries' public funding is the largest
contributor to the neglected disease research effort. However, in recent
years, funding from high-income countries has been steadily decreasing;
in 2007, high-income countries provided 67.5% of the total funding
whereas, in 2012, high-income countries public funds only provided 60%
of the total funding for kinetoplastid infections. This downwards trend
leaves a gap for other funders, such as philanthropic foundations and
private pharmaceutical companies to fill.
Much of the progress that has been made in African sleeping
sickness and neglected disease research as a whole is a result of the
other non-public funders. One of these major sources of funding has come
from foundations, which have increasingly become more committed to
neglected disease drug discovery in the 21st century. In 2012,
philanthropic sources provided 15.9% of the total funding.
The Bill and Melinda Gates Foundation has been a leader in providing
funding for neglected disease drug development. They have provided
$444.1 million US dollars towards neglected disease research in 2012. To
date, they have donated over $1.02 billion US dollars towards the
neglected disease discovery efforts.
For kinetoplastid infections specifically, they have donated an
average of $28.15 million US dollars annually between the years 2007 to
2011.
They have labeled human African trypanosomiasis a high-opportunity
target meaning it is a disease that presents the greatest opportunity
for control, elimination, and eradication, through the development of
new drugs, vaccines, public-health programs, and diagnostics. They are
the second highest funding source for neglected diseases, immediately
behind the US National Institutes of Health.
At a time where public funding is decreasing and government grants for
scientific research are harder to obtain, the philanthropic world has
stepped in to push the research forward.
Another important component of increased interest and funding has
come from industry. In 2012, they contributed 13.1% total to the
kinetoplastid research and development effort, and have additionally
played an important role by contributing to public-private partnerships
(PPP) as well as product-development partnerships (PDP).
A public-private partnership is an arrangement between one or more
public entities and one or more private entities that exists to achieve a
specific health outcome or to produce a health product. The partnership
can exist in numerous ways; they may share and exchange funds,
property, equipment, human resources, and intellectual property. These
public-private partnerships and product-development partnerships have
been established to address challenges in pharmaceutical industry,
especially related to neglected disease research. These partnerships can
help increase the scale of the effort towards therapeutic development
by using different knowledge, skills, and expertise from different
sources. These types of partnerships have been shown to be more
effective than industry or public groups working independently.