From Wikipedia, the free encyclopedia
| Turner syndrome |
|---|
| Other names | Ullrich–Turner syndrome, Bonnevie–Ullrich–Turner syndrome, gonadal dysgenesis; 45X, 45X0 |
|---|
 |
| Five girls and women with Turner syndrome |
| Specialty | Pediatrics, medical genetics |
|---|
| Symptoms | Webbed neck, short stature, swollen hands and feet |
|---|
| Complications | Heart defects, diabetes, low thyroid hormone |
|---|
| Onset | At birth |
|---|
| Duration | Long term |
|---|
| Causes | Missing an X chromosome |
|---|
| Diagnostic method | Physical signs, genetic testing |
|---|
| Medication | Human growth hormone, estrogen replacement therapy |
|---|
| Prognosis | Reduced life expectancy |
|---|
| Frequency | 1 in 2,000 to 5,000 |
|---|
Turner syndrome (TS), also known as 45,X, or 45,X0, is a genetic condition in which a female is partially or completely missing an X chromosome. Signs and symptoms vary among those affected. Often, a short and webbed neck, low-set ears, low hairline at the back of the neck, short stature, and swollen hands and feet are seen at birth. Typically, those affected do not develop menstrual periods, or breasts without hormone treatment and are unable to have children without reproductive technology. Heart defects, diabetes, and low thyroid hormone occur in the disorder more frequently than average. Most people with Turner syndrome have normal intelligence; however, many have problems with spatial visualization that may be needed in order to learn mathematics. Vision and hearing problems also occur more often than average.
Turner syndrome is not usually inherited; rather, it occurs during formation of the reproductive cells in a parent or in early cell division during development. No environmental risks are known, and the mother's age does not play a role. While most people have 46 chromosomes, people with Turner syndrome usually have 45 in some or all cells. The chromosomal abnormality is often present in just some cells, in which case it is known as Turner syndrome with mosaicism. In these cases the symptoms are usually fewer, and possibly none occur at all. Diagnosis is based on physical signs and genetic testing.
No cure for Turner syndrome is known. Treatment may help with symptoms. Human growth hormone injections during childhood may increase adult height. Estrogen replacement therapy can promote development of the breasts and hips. Medical care is often required to manage other health problems with which Turner syndrome is associated.
Turner syndrome occurs in between one in 2,000 and one in 5,000 females at birth. All regions of the world and cultures are affected about equally. Generally people with Turner syndrome have a shorter life expectancy, mostly due to heart problems and diabetes. American endocrinologist Henry Turner first described the condition in 1938. In 1964, it was determined to be due to a chromosomal abnormality.
Presentation
Turner syndrome has a number of physical and psychological impacts, including short stature, heart defects, neck webbing, delayed or absent puberty, and infertility. The phenotype of Turner syndrome is affected by mosaicism,
where cell lines with a single sex chromosome are combined with those
with multiple. Around 40%–50% of cases of Turner syndrome are true
"monosomy X" with a 45,X0 karyotype, while the remainder are mosaic for
another cell line, most commonly 46,XX, or have other structural
abnormalities of the X chromosome. The classic features of Turner syndrome, while distinctive, may be rarer than previously thought; incidental diagnosis, such as in biobank samples or prenatal testing for older mothers, finds many girls and women with few traditional signs of Turner syndrome.
Physiological
Height
Height comparison for women with full and mosaic Turner's compared to
trisomy X and the general population
Turner syndrome is associated with short stature. The mean adult
height of women with Turner syndrome without growth hormone therapy is
around 20 cm (8 in) shorter than the mean of women in the general
population. Mosaicism affects height in Turner syndrome; a large population sample drawn from the UK Biobank found women with 45,X0 karyotypes to have an average height of 145 cm (4 ft 9 in), while those with 45,X0/46,XX karyotypes averaged 159 cm (5 ft 2+1⁄2 in). The strength of the association between Turner syndrome and short stature is such that idiopathic short stature alone is a major diagnostic indication.
Growth delay in Turner syndrome does not begin at birth; most neonates with the condition have a birth weight
in the lower end of the normal range. Height begins to lag in
toddlerhood, with a delayed growth velocity becoming apparent as early
as 18 months. When girls with Turner syndrome begin school, their height
is usually still not remarkably unusual; marked short stature becomes
obvious in mid-childhood. In undiagnosed preadolescents and adolescents,
growth delay may be mistaken for a side effect of delayed puberty and
improperly treated. Short stature in Turner syndrome and its counterpoint, tall stature in sex chromosome polysomy conditions such as Klinefelter syndrome, XYY syndrome, and trisomy X, is caused by the short-stature homeobox gene on the X and Y chromosomes. The absence of a copy of the SHOX
gene in Turner's inhibits skeletal growth, resulting both in overall
short stature and in a distinctive pattern of skeletal malformations
including micrognathia (small chin), cubitus valgus (abnormal forearm angles), and short fingers.
When Turner syndrome is diagnosed in early life, growth hormone therapy
can decrease the degree of short stature. The use of growth hormone
therapy in Turner's originated from a series of studies in the 1980s
finding it to substantially increase the height of treated girls,
compared to prior adult height predictions and Turner's growth charts; treatment with human growth hormone appears to increase expected adult height by approximately 7 cm (3 in) from an otherwise expected norm of 142 cm (4 ft 8 in)–147 cm (4 ft 10 in). In some cases oxandrolone,
a steroid with a relatively mild masculinizing effect, may be used
alongside growth hormone. The addition of oxandrolone to a Turner's
treatment regimen adds around 2 cm (1 in) to the final height.
Oxandrolone is used particularly often in girls diagnosed later in
their growth period, due to the reduced impact of growth hormone alone
in this population. However, oxandrolone use runs the risk of delayed
breast development, voice deepening, increased body hair, or clitoromegaly. The effects of growth hormone therapy are at their strongest during the first year of treatment and taper off over time.
Physical features
Webbed neck in a teenage girl with Turner syndrome
In addition to short stature, Turner syndrome is associated with a
number of characteristic physical features. These include a webbed neck,
a low hairline, a small chin and jaw, a high-arched palate, and a broad chest with wide-spaced nipples. Lymphedema (swelling) of the hands and feet is common at birth and sometimes persistent throughout the lifespan. Some Turner's stigmata, such as cubitus valgus and shortened fingers, are related to SHOX gene dosage effects.
A number of the external manifestations of Turner syndrome are
focused on the limbs, hands, and feet. Lymphedema at birth is one of the
classic features of the syndrome; though it often resolves during
toddlerhood, recurrence in later life is frequent, often without
apparent cause. Cases where the retained X chromosome was inherited from
the mother more often experience lymphedema than those where it was
from the father. As a consequence of lymphedema's effects on nail
anatomy, females with Turner syndrome frequently have small hypoplastic nails. Shortened metacarpal bones, particularly the fourth metacarpal, are a frequent finding.
The body shape of individuals with Turner syndrome is frequently quite
broad and stocky, as the growth deficiency is more pronounced in the
length of bones than in their width. Scoliosis is common in Turner syndrome, and is seen in 40% of girls without growth hormone treatment.
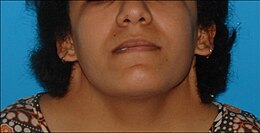
Facial features associated with Turner syndrome include prominent ears, a low hairline, a webbed neck, a small chin with dental malocclusion, and downslanting palpebral fissures
(the opening between the eyelids). These are thought to be related to
lymphedema during the fetal period, specifically to the presence and
resorption of excess fluids in the head and neck region. Neck webbing is a particularly distinctive trait of Turner syndrome, leading to many neonatal diagnoses. The underlying etiology
of neck webbing is related to prenatal blood flow issues, and even in
populations without Turner's has broad health consequences; the rate of
congenital heart disease in webbed neck is 150-fold higher than in the
general population, while the feature is also associated with reduced
height and minor developmental impairments. Some women with Turner syndrome have premature facial wrinkling.[14] Acne is less common in teenage girls and women with Turner syndrome, though the reasons why are unclear.
An infant with Turner syndrome
Other physical features connected to the condition include long eyelashes, sometimes including an additional set of eyelashes, and unusual dermatoglyphics (fingerprints). Some women with Turner's report being unable to create fingerprint passwords due to hypoplastic dermatoglyphics. Unusual dermatoglyphics are common to chromosome anomalies and in the case of Turner's may be a consequence of fetal lymphedema. Keloid
scars, or raised hypertrophic scars growing beyond the boundaries of
the original wound, are potentially associated with Turner syndrome;
however, the association is underresearched. Though traditional medical
counselling on the topic urges conservatism about elective procedures
such as ear piercing due to the risk of severe scarring, the actual
consequences are unclear. Keloids in Turner syndrome are particularly
frequent following surgical procedures to reduce neck webbing.
Turner syndrome has been associated with unusual patterns of hair
growth, such as patches of short and long hair. Armpit and pubic hair is
often sparse, while arm and leg hair is often thick. Though armpit hair
is reduced in amount and thickness, the pattern in which it is
implanted in the skin is as in men, rather than as in women.
Cardiac
Approximately half of individuals with Turner syndrome have congenital heart defects. CHDs associated with Turner syndrome include bicuspid aortic valves (30%), coarctation of the aorta (15%), and abnormalities of the arteries in the head and neck. A rare but potentially fatal complication of heart defects in Turner syndrome is aortic dissection, where the inner layer of the aorta
tears open. Aortic dissection is six times as common in females with
Turner syndrome as the general population and accounts for 8% of all
deaths in the syndrome. The risk is substantially increased for
individuals with bicuspid aortic valves, who make up 95% of patients
with aortic dissection compared to 30% of all Turner's patients, and
coarctation of the aorta, who make up 90% and 15% respectively.
Coronary artery disease
onsets earlier in life in women with Turner syndrome compared to
controls, and mortality from cardiac events is increased. This is
thought to be in part a function of the relationship between Turner
syndrome and obesity;
women with Turner syndrome have a higher percentage of body fat for
their weight than control women, and their short stature makes weight
control more difficult. Though coronary artery disease is frequently
thought a disease of older adults, young women with Turner syndrome are
more likely to develop the disease than their 46,XX peers. Treatment
recommendations for women with Turner syndrome and coronary artery
disease are as in the general population, but as Turner's increases the
risk of type 2 diabetes, women with insulin resistance must weigh up the
benefits of prophylactic or early statin treatment with the risk of diabetes.
Internal medicine
Turner
syndrome is associated with a broad variety of health considerations,
such as liver and kidney issues, obesity, diabetes, and hypertension. Liver dysfunction is common in women with Turner syndrome, with 50%–80% having elevated liver enzymes. Non-alcoholic fatty liver disease
is increased in prevalence in Turner syndrome, likely related in part
to both conditions' associations with obesity. Hepatic vascular diseases
are also seen in the syndrome as an aspect of Turner syndrome's broader
vascular and cardiac impacts. Primary biliary cholangitis
is more common in 45,X0 than 46,XX women. An unclear association exists
between estrogen replacement therapy and liver dysfunction in Turner
syndrome; some studies imply estrogen therapy worsens such conditions,
while others imply improvement.
Kidney issues, such as horseshoe kidney, are sometimes observed in Turner syndrome.
Horseshoe kidney, where the kidneys are fused together in a U-shape,
occurs in around 10% of Turner's cases compared to less than 0.5% of the
general population. A missing kidney is observed in as many as 5% of
individuals with Turner syndrome, compared to around 0.1% of the
population. A duplicated ureter, where two ureters
drain a single kidney, occurs in as much as 20%–30% of the Turner
syndrome population. Kidney malformations in Turner syndrome may be more
common in mosaicism than in the full 45,X0 karyotype.
Serious complications of the kidney anomalies associated with Turner
syndrome are rare, although there is some risk of issues such as obstructive uropathy, where the flow of urine from the kidneys is blocked.
Women with Turner syndrome are more likely than average to have
high blood pressure; as many as 60% of women with the condition are
hypertensive. Isolated diastolic hypertension often precedes systolic hypertension
in the condition and may develop at a young age. Treatments for
hypertension in Turner syndrome are as in the general population.
Approximately 25%–80% of women with Turner syndrome have some level of insulin resistance, and a minority develop type 2 diabetes. The risk of diabetes in Turner syndrome varies by karyotype and appears to be raised by specific deletions of the short arm
of the X chromosome (Xp). One study found that while a relatively low
9% of women with Xq (long arm) deletions had type 2 diabetes, 18% of
those with full 45,X0 karyotypes did, as well as 23% with Xp deletions.
43% of women with isochromosome Xq, who both lacked the short arm and had an additional copy of the long arm, developed type 2 diabetes.
Though part of the diabetes risk in Turner syndrome is a function of
weight control, some is independent; age- and weight-matched women with
non-Turner's ovarian failure have a lower diabetes risk than in Turner
syndrome. Growth hormone treatment plays an unclear role in diabetes
risk, as does estrogen supplementation.
The association between Turner syndrome and other diseases, such
as cancer, is unclear. Overall, women with Turner syndrome do not appear
more likely to develop cancer than women with 46,XX karyotypes, but the
specific pattern of what cancers are highest risk seems to differ. The
risk of breast cancer appears lower in Turner's than in control women, perhaps due to decreased levels of estrogen. Neuroblastoma,
a cancer of infancy and early childhood, has been reported in girls
with Turner syndrome. Tumours of the nervous system, both the central nervous system and the peripheral nervous system, are overrepresented amongst cancers in Turner syndrome. Furthermore, about 5.5% of Turner syndrome individuals have an extra, abnormal small supernumerary marker chromosome (sSMC) which consists of part of a Y chromosome. This partial Y chromosome-bearing sSMC may include the SRY gene located on the p arm of the Y chromosome at band 11.2 (notated as Yp11.2). This gene encodes the testis-determining factor protein (also known as sex-determining region Y protein). Turner syndrome individuals with this SRY gene-containing sSMC have a very real increased risk of developing gonadal tissue neoplasms such as gonadoblastomas and in situ seminomas (also termed dysgerminomas to indicate that this tumor has the pathology of the testicular tumor, seminoma, but develops in ovaries). In one study, 34 Turner syndrome girls without overt evidence of these tumors were found at preventative surgery to have a gonadoblastoma (7 cases), dysgerminoma (1 case), or non-specific in situ gonadal neoplasm (1 case).
Turner syndrome girls with this sSMC otherwise have typical features of
the Turner syndrome except for a minority who also have hirsutism and/or clitoral enlargement. Surgical removal of the gonads has been recommended to remove the threat of developing these sSMC-associated neoplasms. Tuner syndrome individuals with an sSMC that lacks the SRY gene are not at an increased risk of developing these cancers.
Sensory
Hearing
loss is common in Turner syndrome. Though at birth hearing is generally
normal, chronic middle ear problems are frequent throughout childhood,
which can cause permanent conductive hearing loss. In adulthood, sensorineural hearing loss
occurs more often than in 46,XX women and at younger ages; though
differing thresholds of hearing loss make it difficult to compare
between studies, younger adult women with Turner syndrome are routinely
found to have disproportionate rates of hearing issues, with sometimes
up to half of women in their 20s and 30s having poor hearing.
This hearing loss is progressive; at the age of 40, women with Turner
syndrome have equivalent hearing loss to 46,XX women aged 60, on
average. Cohort studies imply hearing loss may be more common in women who also have metabolic syndrome. The high prevalence of sensorineural hearing loss in Turner syndrome appears to be related to SHOX deficiency.
Ocular and visual disorders are also increased in prevalence in
Turner syndrome. More than half of individuals with Turner syndrome have
some form of eye disorder. This may be a consequence of shared genes on
the X chromosome in both eye and ovary development. Nearly half of cases have hyperopia or myopia, usually mild. Strabismus,
or misalignment of the eye, occurs in around one-fifth to one-third of
girls with Turner syndrome. As with strabismus outside the Turner's
context, it may be treated with glasses, patching, or surgical
correction. Esotropia, where the eye turns inwards, is more common than exotropia, where it turns outwards. Ptosis,
or a drooping eyelid, is a common facial manifestation of Turner
syndrome; it usually has no appreciable impact on vision, but severe
cases may limit visual range and require surgical correction. The rate of red-green colourblindness in Turner syndrome is 8%, the same as in men. This is due to red-green colourblindness being an X-linked recessive
condition; in people with a single X chromosome, whether normal males
or Turner females, only a single mutated X is necessary for symptoms.
Red-green colourblindness may be underdiagnosed in the Turner context,
as the rarity of the condition in females reduces the likelihood of
screening, and practitioners may not connect that the karyotype of
Turner syndrome increases the risk from the female baseline.
Autoimmune
Women with Turner syndrome are two to three times as likely to develop autoimmune disorders as the general population. Specific autoimmune disorders linked to Turner syndrome include Hashimoto's disease, vitiligo, psoriasis and psoriatic arthritis, alopecia, and celiac disease. Inflammatory bowel disease is also common, while the prevalence of type 1 diabetes is unclear, though appears increased.
Thyroid disease is common in Turner syndrome. Hypothyroidism
is prevalent; 30%–50% of women with Turner syndrome have Hashimoto's
disease, where the thyroid gland is slowly destroyed by an autoimmune
reaction. By age 50, half of women with Turner syndrome have subclinical
or clinical hypothyroidism. Hyperthyroidism and Graves' disease
are also increased in prevalence, though more modestly. The Turner's
presentation of hyperthyroidism is as in the general population, while
the presentation of hypothyroidism is often atypical, with a mild early
presentation yet a more severe progression.
Women with isochromosome Xq are more likely to develop autoimmune
thyroid disease than women with other forms of Turner syndrome.
The risk of irritable bowel syndrome is increased around fivefold in Turner syndrome, and that of ulcerative colitis
around fourfold. Celiac disease is also increased in prevalence, with
around 4%–8% of Turner's patients having comorbid celiac disease
compared to 0.5%–1% of the general population. Diagnosis of such
conditions is difficult due to their nonspecific early symptoms. In the
Turner's context, diagnosis may in particular be missed due to growth
delay; such conditions cause growth delay and failure to thrive when
they onset in childhood, but as girls with Turner syndrome already have
such delay, symptoms may be overlooked and ascribed to the original
condition.
Alopecia areata,
or recurrent patchy hair loss, is three times as common in Turner
syndrome as the general population. Alopecia in the Turner syndrome
context is frequently treatment-resistant, also seen in other chromosome
aneuploidies such as Down syndrome.
Psoriasis is common in Turner syndrome, although the precise prevalence
is unclear. Turner's psoriasis may be related to growth hormone
treatment, as psoriasis as a side effect of such therapies has been
reported in patients without the karyotype. Psoriasis may progress to psoriatic arthritis,
and this progression may be more common in Turner syndrome. Vitiligo
has been reported in conjunction with Turner syndrome, but the risk is
unclear and may be a side effect of increased clinical attention to
autoimmune disease in this population.
Puberty
Histopathology of ovarian tissue in mosaic (A and B) and full (C) Turner syndrome
Puberty is delayed or absent in Turner syndrome. A 2019 literature
review found that 13% of women with a 45,X0 karyotype could expect to
experience spontaneous thelarche (breast development), while 9% would undergo spontaneous menarche
(beginning of menstruation). These numbers were higher in women with
mosaic Turner's; 63% with 45,X0/46,XX karyotypes experienced spontaneous
thelarche and 39% spontaneous menarche, while 88% with 45,X0/47,XXX
(the presence of a trisomy X
cell line) experienced spontaneous thelarche and 66% spontaneous
menarche. Unexpectedly, women with Y-chromosome cells also had increased
rates of thelarche and menarche compared to the 45,X0 baseline, at 41%
and 19%. However, few women with trisomy X or Y-chromosome cell lines
were covered in the review, impeding extrapolation from these results. 6% of women with Turner syndrome have regular menstrual cycles; the rest experience primary or secondary amenorrhea or other menstrual dysfunction.
In girls with Turner syndrome who do not experience spontaneous puberty, exogenous
estrogen is used to induce and maintain feminization. Estrogen
replacement is recommended to begin at around age 11–12, although some
parents prefer to delay the induction of puberty in girls with lower
social and emotional preparedness. The dose of estrogen in induced
puberty begins at 10% of adult estrogen levels and is steadily increased
at six-month intervals, with a full adult dose attained two to three
years after the beginning of treatment. Estrogen replacement may
interfere with growth hormone therapy, due to the closing effects of
estrogen on growth plates; individuals must weigh up their preferences
for taller height versus greater feminization.
Fertility
Women
with Turner syndrome are infertile. Only 2%–5% are capable of pregnancy
without fertility treatment, most with mosaic karyotypes. Early in
gestation, fetuses with Turner syndrome have a normal number of gametes
in their developing ovaries, but this starts decreasingly rapidly as
early as 18 weeks of pregnancy; by birth, girls with the condition have
markedly reduced follicular counts. Women with Turner syndrome who wish to raise families but are incapable of conception with their own oocytes have the options of adoption or of pregnancy with donor eggs; the latter has a comparable success rate to donor pregnancy in women with 46,XX karyotypes.
Pregnancy in Turner syndrome is inherently high-risk; the maternal death rate is 2%.
Usually, estrogen replacement therapy is used to spur the growth
of secondary sexual characteristics at the time when puberty should
onset. While very few women with Turner syndrome menstruate
spontaneously, estrogen therapy requires a regular shedding of the
uterine lining ("withdrawal bleeding") to prevent its overgrowth.
Withdrawal bleeding can be induced monthly, like menstruation, or less
often, usually every three months, if the patient desires. Estrogen
therapy does not make a woman with nonfunctional ovaries fertile, but it
plays an important role in assisted reproduction; the health of the
uterus must be maintained with estrogen if an eligible woman with Turner
Syndrome wishes to use IVF (using donated oocytes).
Especially in mosaic cases of Turner syndrome that contains
Y-chromosome (e.g. 45,X/46,XY) due to the risk of development of ovarian
malignancy (most common is gonadoblastoma) gonadectomy is recommended. Turner syndrome is characterized by primary amenorrhoea, premature ovarian failure (hypergonadotropic hypogonadism), streak gonads
and infertility (however, technology (especially oocyte donation)
provides the opportunity of pregnancy in these patients). Failure to
develop secondary sex characteristics (sexual infantilism) is typical.
Cognition
Neurodevelopmental
Individuals with Turner syndrome have normal intelligence. Verbal IQ is usually higher than performance IQ; one review of thirteen studies found an average verbal IQ of 101 compared to an average performance IQ of 89.
People with Turner syndrome have normal intelligence, and
demonstrate relative strengths in verbal skills, but may exhibit weaker
nonverbal skills – particularly in arithmetic, select visuospatial
skills, and processing speed. Turner syndrome does not typically cause intellectual disability
or impair cognition. However, learning difficulties are common among
women with Turner syndrome, particularly a specific difficulty in
perceiving spatial relationships, such as nonverbal learning disorder. This may also manifest itself as a difficulty with motor control or with mathematics.
While it is not correctable, in most cases it does not cause difficulty
in daily living. Most Turner syndrome patients are employed as adults
and lead productive lives.
Also, a rare variety of Turner syndrome, known as "Ring-X Turner
syndrome", has about a 60% association with intellectual disability. This variety accounts for around 2–4% of all Turner syndrome cases.
Psychological
Social difficulties appear to be an area of vulnerability for young women.
Counseling affected individuals and their families about the need to
carefully develop social skills and relationships may prove useful in
advancing social adaptation. Women with Turner syndrome may experience
adverse psychosocial outcomes which can be improved through early
intervention and the provision of appropriate psychological and
psychiatric care. Genetic, hormonal, and medical problems associated
with Turner syndrome are likely to affect psychosexual development of
female adolescent patients, and thus influence their psychological
functioning, behavior patterns, social interactions, and learning
ability. Although Turner syndrome constitutes a chronic medical
condition, with possible physical, social, and psychological
complications in a woman's life, hormonal and estrogen replacement
therapy, and assisted reproduction, are treatments that can be helpful
for Turner syndrome patients and improve their quality of life. Research shows a possible association between age at diagnosis and increased substance use and depressive symptoms.
Prenatal
Despite the excellent postnatal prognosis, 99% of Turner syndrome conceptions are thought to end in miscarriage or stillbirth, and as many as 15% of all spontaneous abortions have the 45,X karyotype.
Among cases that are detected by routine amniocentesis or chorionic
villus sampling, one study found that the prevalence of Turner syndrome
among tested pregnancies was 5.58 and 13.3 times higher, respectively,
than among live neonates in a similar population.
Cause
Turner
syndrome is caused by the absence of one complete or partial copy of the
X chromosome in some or all the cells. The abnormal cells may have only
one X (monosomy) (45,X) or they may be affected by one of several types of partial monosomy like a deletion of the short p arm of one X chromosome (46,X,del(Xp)) or the presence of an isochromosome with two q arms (46,X,i(Xq)) Turner syndrome has distinct features due to the lack of pseudoautosomal regions, which are typically spared from X-inactivation.
In mosaic individuals, cells with X monosomy (45,X) may occur along
with cells that are normal (46,XX), cells that have partial monosomies,
or cells that have a Y chromosome (46,XY). The presence of mosaicism is estimated to be relatively common in affected individuals (67–90%).
The (46,X,i(Xq) isochromosome in the Turner syndrome is classified as an small supernumerary marker chromosome
(sSMC). Two of the types of sSMCs in this syndrome contain parts of the
genetic material from either an X or, much less frequently, Y
chromosome and may or may not contain an XIST gene. In normal females, the XIST
gene occurs on the X chromosome inherited from her mother but not on
the X chromosome inherited from her father. The gene is not present on Y
chromosomes and in normal females resides on and functions to
inactivate many of the genes located on its own maternal but not the
father's X chromosome. Turner syndrome females with (46,X,i(Xq) sSMC
consisting of a partial X chromosome that does not contain the XIST
gene express at least some of this sSMC's genetic material and
therefore contain excesses of this material. In consequence, they have a
more serious form of the Turner syndrome that ranges form moderately
severe to extremely severe. The extremely severe cases have anencephaly (absence of a major portion of the brain, skull, and scalp), agenesis of the corpus callosum (lack of the thick tract of nerve fibers that connect the left and right cerebral hemispheres),
and complex heart deformities. Individuals with Turner syndrome that
have partial X chromosome containing(46,X,i(Xq) sSMCs that have the XIST gene do not express this sSMC's genetic material and do not have the more severe manifestations of the syndrome.
Inheritance
In the majority of cases where monosomy occurs, the X chromosome comes from the mother. This may be due to a nondisjunction in the father. Meiotic errors that lead to the production of X with p arm deletions or abnormal Y chromosomes are also mostly found in the father. Isochromosome X or ring chromosome X on the other hand are formed equally often by both parents. Overall, the functional X chromosome usually comes from the mother.
In most cases, Turner syndrome is a sporadic event, and for the
parents of an individual with Turner syndrome the risk of recurrence is
not increased for subsequent pregnancies. Rare exceptions may include
the presence of a balanced translocation of the X chromosome in a parent, or where the mother has 45,X mosaicism restricted to her germ cells.
Diagnosis
Prenatal
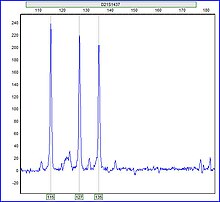
45,X
karyotype, showing an unpaired X at the lower right
Turner syndrome may be diagnosed by amniocentesis or chorionic villus sampling during pregnancy.
Usually, fetuses with Turner syndrome can be identified by abnormal ultrasound findings (i.e., heart defect, kidney abnormality, cystic hygroma, ascites).
In a study of 19 European registries, 67.2% of prenatally diagnosed
cases of Turner syndrome were detected by abnormalities on ultrasound.
69.1% of cases had one anomaly present, and 30.9% had two or more
anomalies.
An increased risk of Turner syndrome may also be indicated by
abnormal triple or quadruple maternal serum screen. The fetuses
diagnosed through positive maternal serum screening are more often found
to have a mosaic karyotype than those diagnosed based on
ultrasonographic abnormalities, and conversely, those with mosaic
karyotypes are less likely to have associated ultrasound abnormalities.
Postnatal
Turner
syndrome can be diagnosed postnatally at any age. Often, it is
diagnosed at birth due to heart problems, an unusually wide neck or
swelling of the hands and feet. However, it is also common for it to go
undiagnosed for several years, often until the girl reaches the age of
puberty and fails to develop typically (the changes associated with
puberty do not occur). In childhood, a short stature can be indicative
of Turner syndrome.
A test called a karyotype,
also known as a chromosome analysis, analyzes the chromosomal
composition of the individual. This is the test of choice to diagnose
Turner syndrome.
Treatment
As a chromosomal condition, there is no cure for Turner syndrome. However, much can be done to minimize the symptoms.
While most of the physical findings are harmless, significant medical
problems can be associated with the syndrome. Most of these significant
conditions are treatable with surgery and other therapies including
hormonal therapy.
- Growth hormone, either alone or with a low dose of androgen, will increase growth and probably final adult height. Growth hormone is approved by the U.S. Food and Drug Administration for treatment of Turner syndrome and is covered by many insurance plans. There is evidence that this is effective, even in toddlers. A 2019 systematic review comparing effects of adding oxandrolone
to growth hormone treatment to growth hormone alone has found
moderate-quality evidence that the addition of oxandrolone leads to an
increase in final adult height of girls with Turner syndrome.
When the same review assessed the effects of adding Oxandrolone to
growth hormone treatment on speech, cognition and psychological status,
the results were inconclusive due to very-low quality evidence.
- Estrogen replacement therapy such as the birth control pill,
has been used since the condition was described in 1938 to promote
development of secondary sexual characteristics. Estrogens are crucial
for maintaining good bone integrity, cardiovascular health and tissue
health.
Women with Turner syndrome who do not have spontaneous puberty and who
are not treated with estrogen are at high risk for osteoporosis and
heart conditions.
- Modern reproductive technologies
have also been used to help women with Turner syndrome become pregnant
if they desire. For example, a donor egg can be used to create an
embryo, which is carried by the Turner syndrome woman.
- Uterine maturity is positively associated with years of estrogen
use, history of spontaneous menarche, and negatively associated with the
lack of current hormone replacement therapy.
Epidemiology
Turner syndrome occurs in between one in 2000 and one in 5000 females at birth.
Approximately 99 percent of fetuses with Turner syndrome spontaneously terminate during the first trimester. Turner syndrome accounts for about 10 percent of the total number of spontaneous abortions in the United States.
History
The syndrome is named after Henry Turner, an endocrinologist from Illinois, who described it in 1938. In Europe, it is often called Ullrich–Turner syndrome or Bonnevie–Ullrich–Turner syndrome to acknowledge that earlier cases had also been described by European doctors Kristine Bonnevie and Otto Ullrich. In Russian and USSR literature, it is called Shereshevsky–Turner syndrome to acknowledge that the condition was first described as hereditary in 1925 by the Soviet endocrinologist Nikolai Shereshevsky [ru], who believed that it was due to the underdevelopment of the gonads and the anterior pituitary gland and was combined with congenital malformations of internal development.
The first published report of a female with a 45,X karyotype was in 1959 by Charles Ford and colleagues in Harwell near Oxford, and Guy's Hospital in London. It was found in a 14-year-old girl with signs of Turner syndrome.