| Vagus nerve | |
|---|---|

Plan of the upper portions of the glossopharyngeal, vagus, and accessory nerves.
| |
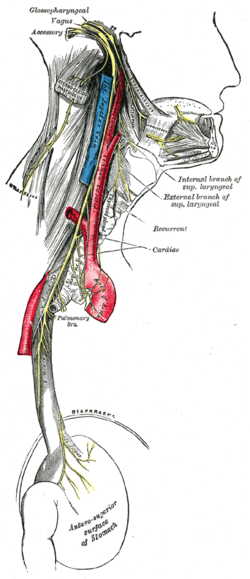
Course and distribution of the glossopharyngeal, vagus, and accessory nerves.
| |
| Details | |
| Innervates | Levator veli palatini, Salpingopharyngeus, Palatoglossus, Palatopharyngeus, Superior pharyngeal constrictor, Middle pharyngeal constrictor, visceratyppi, Inferior pharyngeal constrictor, viscera rass |
| Identifiers | |
| Latin | nervus vagus |
| MeSH | D014630 |
| NeuroNames | 702 |
| TA | A14.2.01.153 |
| FMA | 5731 |
The vagus nerve, historically cited as the pneumogastric nerve, is the tenth cranial nerve or CN X, and interfaces with the parasympathetic control of the heart, lungs, and digestive tract. The vagus nerves are paired but are normally referred to in the singular. It is the longest nerve of the autonomic nervous system in the human body.
Structure
Upon leaving the medulla oblongata between the pyramid and the inferior cerebellar peduncle, the vagus nerve extends through the jugular foramen, then passes into the carotid sheath between the internal carotid artery and the internal jugular vein down to the neck, chest, and abdomen, where it contributes to the innervation of the viscera, reaching all the way to the colon. Besides giving some output to various organs, the vagus nerve comprises between 80% and 90% of afferent nerves mostly conveying sensory information about the state of the body's organs to the central nervous system.
The right and left vagus nerves descend from the cranial vault through the jugular foramina, penetrating the carotid sheath
between the internal and external carotid arteries, then passing
posterolateral to the common carotid artery. The cell bodies of visceral afferent fibers of the vagus nerve are located bilaterally in the inferior ganglion of the vagus nerve (nodose ganglia).
The right vagus nerve gives rise to the right recurrent laryngeal nerve, which hooks around the right subclavian artery and ascends into the neck between the trachea and esophagus. The right vagus then crosses anterior to the right subclavian artery, runs posterior to the superior vena cava, descends posterior to the right main bronchus, and contributes to cardiac, pulmonary, and esophageal plexuses. It forms the posterior vagal trunk at the lower part of the esophagus and enters the diaphragm through the esophageal hiatus.
The left vagus nerve enters the thorax between left common carotid artery and left subclavian artery and descends on the aortic arch. It gives rise to the left recurrent laryngeal nerve, which hooks around the aortic arch to the left of the ligamentum arteriosum
and ascends between the trachea and esophagus. The left vagus further
gives off thoracic cardiac branches, breaks up into the pulmonary
plexus, continues into the esophageal plexus, and enters the abdomen as
the anterior vagal trunk in the esophageal hiatus of the diaphragm.
- Pharyngeal nerve
- Superior laryngeal nerve
- Superior cervical cardiac branches of vagus nerve
- Inferior cervical cardiac branch
- Recurrent laryngeal nerve
- Thoracic cardiac branches
- Branches to the pulmonary plexus
- Branches to the esophageal plexus
- Anterior vagal trunk
- Posterior vagal trunk
- Hering-Breuer reflex in alveoli
The vagus runs parallel to the common carotid artery and internal jugular vein inside the carotid sheath.
Nuclei
- The dorsal nucleus of vagus nerve – which sends parasympathetic output to the viscera, especially the intestines
- The nucleus ambiguus – which gives rise to the branchial efferent motor fibers of the vagus nerve and preganglionic parasympathetic neurons that innervate the heart
- The solitary nucleus – which receives afferent taste information and primary afferents from visceral organs
- The spinal trigeminal nucleus – which receives information about deep/crude touch, pain, and temperature of the outer ear, the dura of the posterior cranial fossa and the mucosa of the larynx
Development
The motor division of the vagus nerve is derived from the basal plate of the embryonic medulla oblongata, while the sensory division originates from the cranial neural crest.
Function
The vagus nerve supplies motor parasympathetic fibers to all the organs (except the adrenal glands), from the neck down to the second segment of the transverse colon. The vagus also controls a few skeletal muscles, including:
- Cricothyroid muscle
- Levator veli palatini muscle
- Salpingopharyngeus muscle
- Palatoglossus muscle
- Palatopharyngeus muscle
- Superior, middle and inferior pharyngeal constrictors
- Muscles of the larynx (speech).
This means that the vagus nerve is responsible for such varied tasks as heart rate, gastrointestinal peristalsis, sweating, and quite a few muscle movements in the mouth, including speech (via the recurrent laryngeal nerve). It also has some afferent fibers that innervate the inner (canal) portion of the outer ear (via the auricular branch, also known as Alderman's nerve) and part of the meninges.
Efferent vagus nerve fibers innervating the pharynx and back of the throat are responsible for the gag reflex. In addition, 5-HT3 receptor-mediated afferent vagus stimulation in the gut due to gastroenteritis is a cause of vomiting. Stimulation of the vagus nerve in the cervix uteri (as in some medical procedures) can lead to a vasovagal response.
The vagus nerve also plays a role in satiation following food consumption. Knocking out vagal nerve receptors has been shown to cause hyperphagia (greatly increased food intake).
Vagus nerve and the heart
H&E stained fibers of the vagus nerve (bottom right) innervate the sinoatrial node tissue (middle left)
Parasympathetic innervation of the heart is partially controlled by the vagus nerve and is shared by the thoracic ganglia. Vagal and spinal ganglionic nerves mediate the lowering of the heart rate. The right vagus branch innervates the sinoatrial node.
In healthy people, parasympathetic tone from these sources are
well-matched to sympathetic tone. Hyperstimulation of parasympathetic
influence promotes bradyarrhythmias. When hyperstimulated, the left vagal branch predisposes the heart to conduction block at the atrioventricular node.
At this location, neuroscientist Otto Loewi first demonstrated that nerves secrete substances called neurotransmitters,
which have effects on receptors in target tissues. In his experiment,
Loewi electrically stimulated the vagus nerve of a frog heart, which
slowed the heart. Then he took the fluid from the heart and transferred
it to a second frog heart without a vagus nerve. The second heart slowed
down without an electrical stimulation. Loewi described the substance
released by the vagus nerve as vagusstoff, which was later found to be acetylcholine. Drugs that inhibit the muscarinic receptors (anticholinergics) such as atropine and scopolamine,
are called vagolytic because they inhibit the action of the vagus nerve
on the heart, gastrointestinal tract, and other organs.
Anticholinergic drugs increase heart rate and are used to treat bradycardia.
Physical and emotional effects
Excessive activation of the vagal nerve during emotional stress, which is a parasympathetic overcompensation for a strong sympathetic nervous system response associated with stress, can also cause vasovagal syncope due to a sudden drop in cardiac output, causing cerebral hypoperfusion. Vasovagal syncope affects young children and women more than other groups. It can also lead to temporary loss of bladder control under moments of extreme fear.
Research has shown that women having had complete spinal cord injury can experience orgasms through the vagus nerve, which can go from the uterus, cervix, and, it is presumed, the vagina to the brain.
Insulin signaling activates the adenosine triphosphate (ATP)-sensitive potassium (KATP) channels in the arcuate nucleus,
decreases AgRP release, and through the vagus nerve, leads to decreased
glucose production by the liver by decreasing gluconeogenic enzymes: Phosphoenolpyruvate carboxykinase, Glucose 6-phosphatase.
Clinical significance
Vagus nerve stimulation
Vagus nerve stimulation (VNS) therapy using a neurostimulator implanted in the chest is a treatment used since 1997 to control seizures in epilepsy patients and has been approved for treating drug-resistant cases of clinical depression. A non-invasive VNS device that stimulates an afferent branch of the vagus nerve is also being developed and will soon undergo trials.
Clinical trials have started in Antwerp, Belgium, using VNS for the treatment of tonal tinnitus after a breakthrough study published in early 2011 by researchers at the University of Texas - Dallas showed successful tinnitus-suppression in rats when tones were paired with brief pulses of stimulation of the vagus nerve.
VNS may also be achieved by one of the vagal maneuvers:
holding the breath for a few seconds, dipping the face in cold water,
coughing, or tensing the stomach muscles as if to bear down to have a
bowel movement. Patients with supraventricular tachycardia, atrial fibrillation, and other illnesses may be trained to perform vagal maneuvers (or find one or more on their own).
Vagus nerve blocking (VBLOC) therapy is similar to VNS but used only during the day. In a six-month open-label trial
involving three medical centers in Australia, Mexico, and Norway, vagus
nerve blocking helped 31 obese participants lose an average of nearly
15 percent of their excess weight. As of 2008 a year-long 300-participant double-blind, phase II trial had begun.
Vagotomy
Vagotomy
(cutting of the vagus nerve) is a now-obsolete therapy that was
performed for peptic ulcer disease. Vagotomy is currently being
researched as a less invasive alternative weight-loss procedure to gastric bypass surgery.
The procedure curbs the feeling of hunger and is sometimes performed in
conjunction with putting bands on patients' stomachs, resulting in an
average of 43% of excess weight lost at six months with diet and
exercise.
One serious side effect of a vagotomy is a vitamin B12 deficiency later in life – perhaps after about 10 years – that is similar to pernicious anemia. The vagus normally stimulates the stomach's parietal cells to secrete acid and intrinsic factor. Intrinsic factor is needed to absorb vitamin B12
from food. The vagotomy reduces this secretion and ultimately leads to
the deficiency, which, if left untreated, causes nerve damage,
tiredness, dementia, paranoia, and ultimately death.
Researchers from Aarhus University and Aarhus University Hospital
have demonstrated that vagotomy prevents (halves the risk of) the
development of Parkinson's disease, suggesting that Parkinson's disease begins in the gastrointestinal tract and spreads via the vagus nerve to the brain.
Or giving further evidence to the theory that dysregulated
environmental stimuli, such as that received by the vagus nerve from the
gut, may have a negative effect on the dopamine reward system of the substantia nigra, thereby causing Parkinsons disease.
Chagas disease
The neuropathy in Chagas disease spreads in part via the major parasympathetic branches of the vagus nerve.
History
Etymology
The Latin word vagus means literally "wandering" (the words vagrant, vagabond, and vague come from the same root). Sometimes the right and left branches together are spoken of in the plural and are thus called vagi (/ˈveɪdʒaɪ/VAY-jy). The vagus was also historically called the pneumogastric nerve since it innervates both the lungs and the stomach.

